Animal Physiology is the study of how the body functions at the cellular, tissue, organ, and system levels. It seeks to explain the mechanisms that allow animals to maintain life, adapt to their environments, and respond to internal and external challenges. For veterinary students and professionals, a strong foundation in physiology is essential for understanding health, diagnosing disease, and applying effective treatment strategies.
This course explores the major physiological systems of animals, including the nervous, cardiovascular, respiratory, digestive, endocrine, renal, and reproductive systems. Emphasis is placed on the integration of these systems, recognizing that no organ functions in isolation. Instead, the body operates as a coordinated unit, maintaining stability through complex regulatory processes.
A central concept in animal physiology is homeostasis, the ability of the body to maintain a stable internal environment despite changes in external conditions. Physiological systems work continuously to regulate parameters such as temperature, pH, fluid balance, and energy metabolism. Disruptions to these processes form the basis of disease, making physiology a critical bridge between basic science and clinical practice.
Throughout this course, students will examine:
The course adopts a comparative approach, highlighting similarities and differences among species such as companion animals, livestock, and equine species. This perspective is particularly important in veterinary medicine, where physiological variation directly influences clinical decision-making.
By the end of this course, learners will be able to:
Ultimately, Animal Physiology provides the framework for understanding why the body behaves the way it does-knowledge that is indispensable for every veterinarian, from student to practicing clinician.
Homeostasis is the ability of a living organism to maintain a relatively stable internal environment (also called the "milieu intérieur") despite changes in the external environment. Rather than a static state, it is a constant, fluctuating balance around a 'set point'. This fluctuating balance is called Dynamic Equilibrium.
A set point is the ideal value for a physiological variable (e.g., ~38–39°C in many domestic animals) that the body works to maintain for optimal health and stability. It acts as a reference point (like a thermostat setting) that the body constantly monitors, resisting deviations to keep internal conditions stable. Different species have different set points.
Normal range / Dynamic Range: Is the acceptable variation around the set point. Stress, age, disease, and environment can shift normal ranges.
Adjustment / Alteration : Set points can be adjusted in response to changing conditions, such as the hypothalamus raising the body temperature set point to create a fever to fight infection.
Every homeostatic control system consists of three main components:
Receptors (Sensors) are specialized cells or nerve endings that monitor the environment and detect a stimulus. A stimulus is a change in a variable like temperature or blood sugar. Examples:
The control center processes information and determines the response. Usually located in the central nervous system (CNS) or endocrine glands. Compares detected value to a set point.
Example:
Effectors are organs, tissues, or cells (like sweat glands or muscles) that carry out the instructions from the control centre to counteract the change and restore balance. Examples:
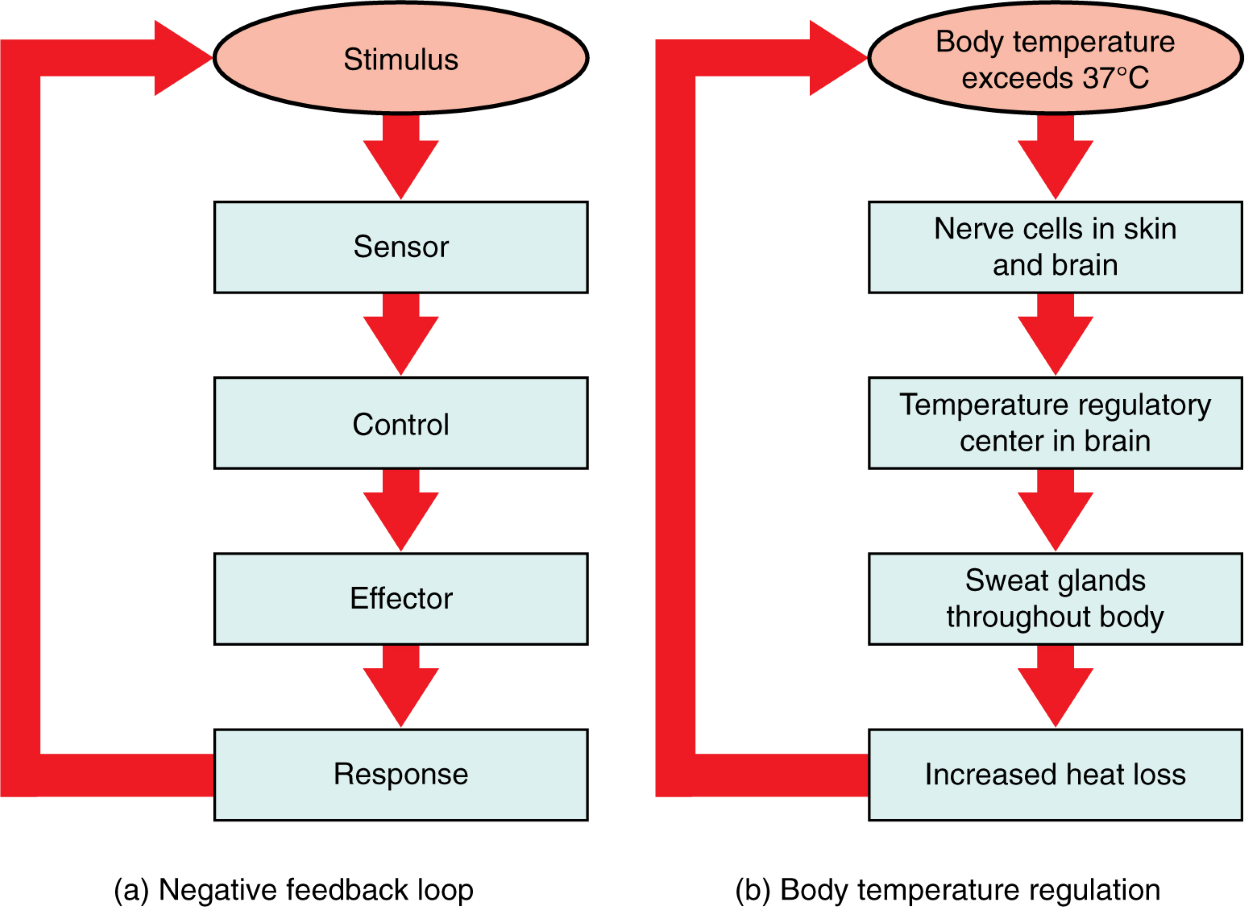
Negative feedback is a primary homeostatic mechanism that maintains stable internal conditions by reversing deviations from a set point. When a bodily parameter (e.g., temperature, blood sugar) shifts too high or low, sensors alert a control center, which triggers effectors to counteract the change, restoring balance.
Example: Thermoregulation
Increase in body temperature - sweating, vasodilation
Decrease in temperature - shivering, vasoconstriction
Negative feedback is stabilizing and maintains normal physiological ranges.
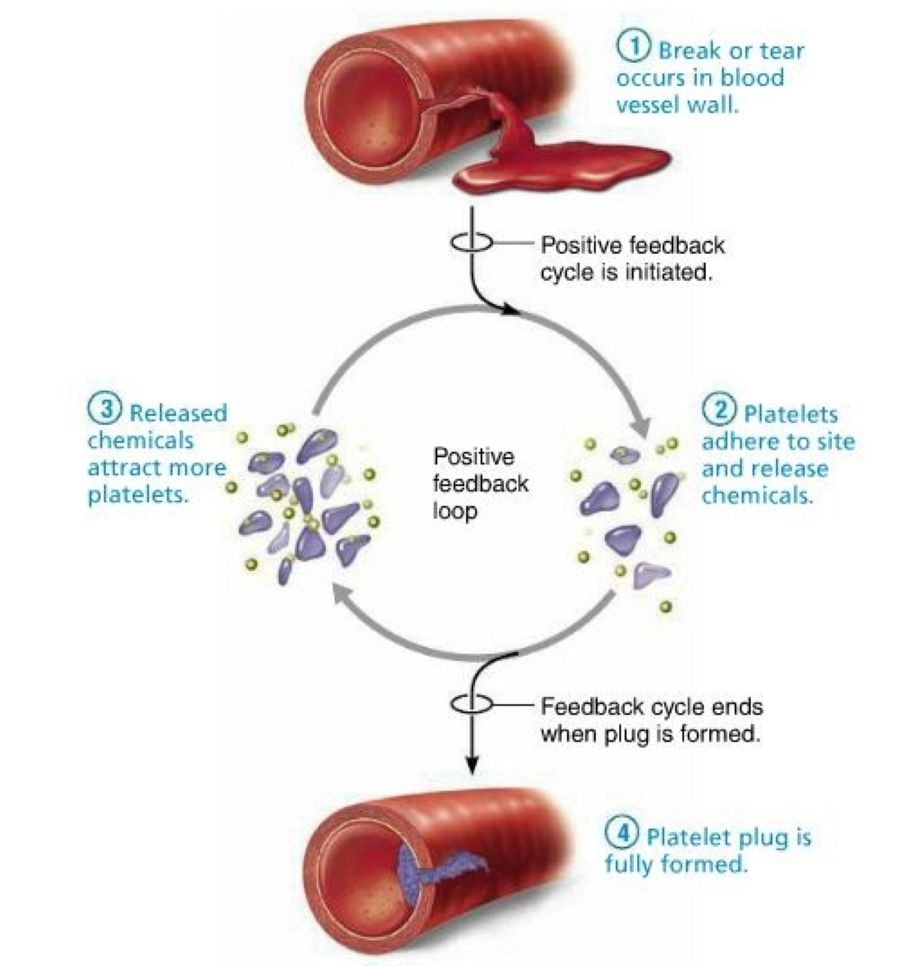
A response that amplifies the initial stimulus, pushing the system further in the same direction.
Examples:
Parturition (oxytocin release → stronger uterine contractions)
Blood clotting cascade
Positive feedback is typically short-lived and requires an external event to stop it.
The regulation of body temperature, or thermoregulation, is a fundamental aspect of animal physiology that ensures optimal functioning of biochemical and cellular processes. Most physiological reactions are temperature-sensitive, and even small deviations from the normal range can impair enzyme activity, metabolism, and overall health. Animals have therefore evolved mechanisms to maintain thermal balance with their environment, a process closely linked to homeostasis.
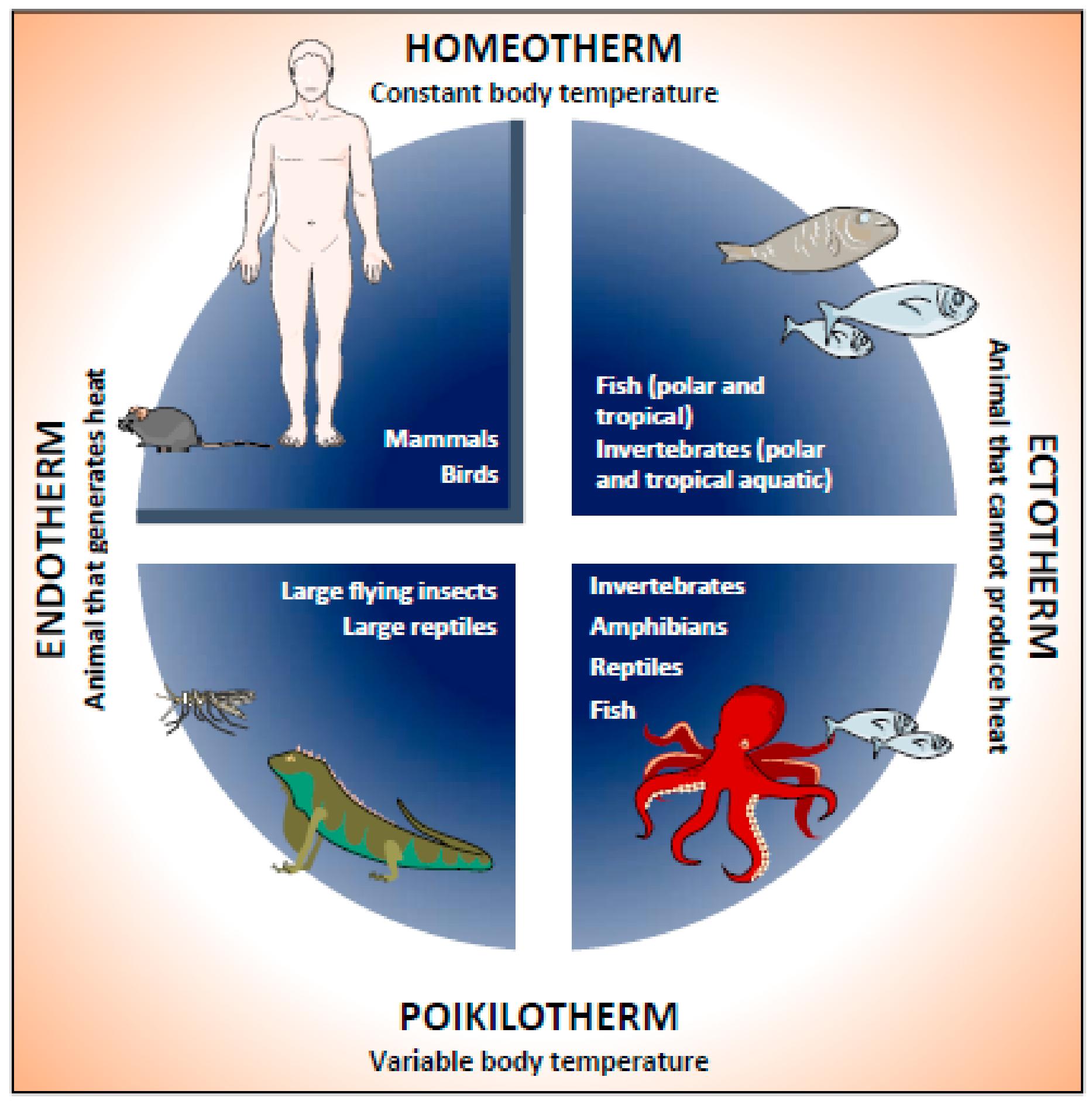
Animals can broadly be classified into endotherms and ectotherms based on how they regulate body temperature. Endotherms, such as mammals and birds, generate most of their body heat internally through metabolic processes. They maintain a relatively constant internal temperature regardless of environmental conditions. In contrast, ectotherms, including reptiles, amphibians, and fish, rely heavily on external heat sources and exhibit body temperatures that fluctuate with the environment.
Endothermy provides the advantage of sustained activity across a wide range of temperatures but comes at a high energetic cost. Ectothermy is energy-efficient but limits activity during unfavorable thermal conditions.
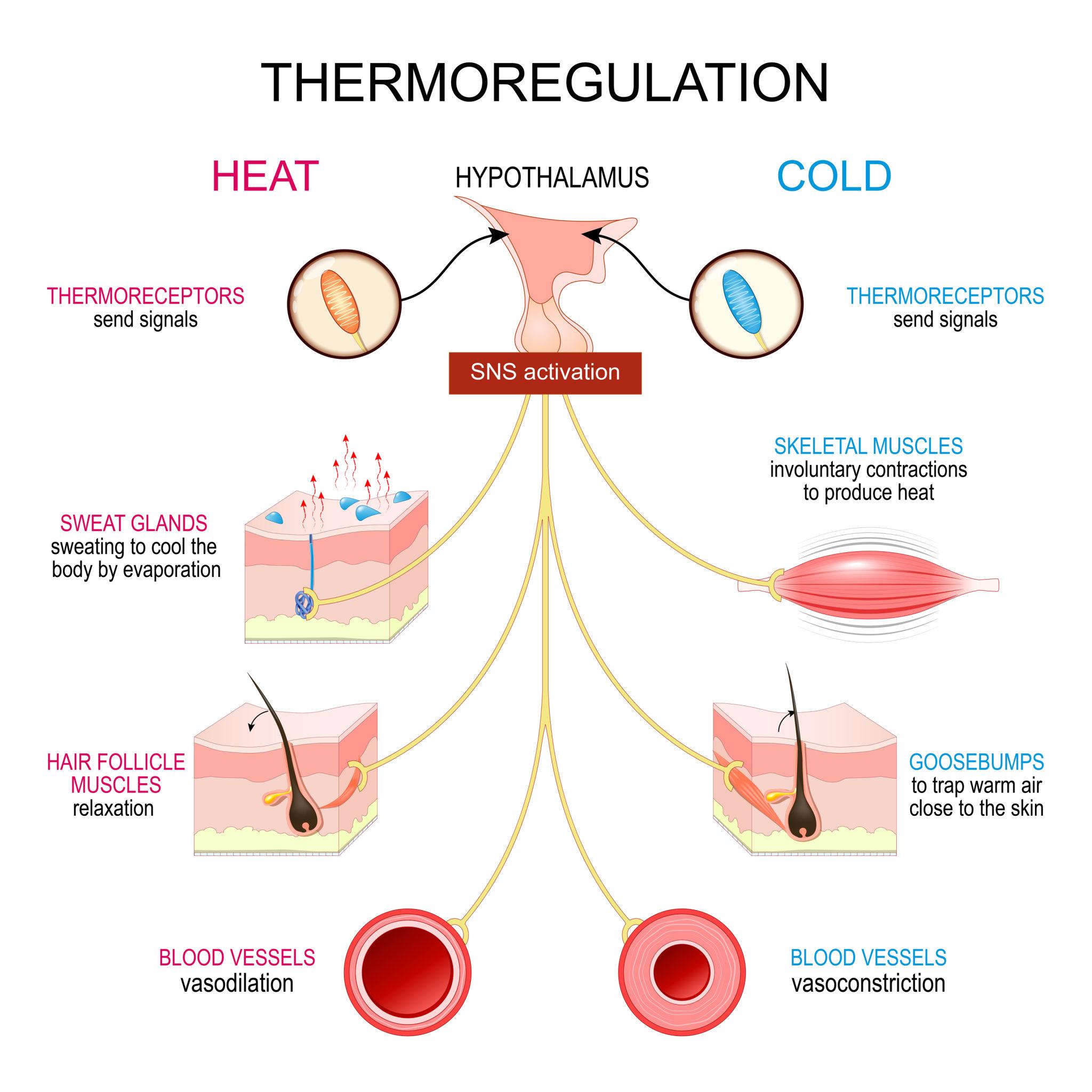
In vertebrates, the hypothalamus acts as the central control center for thermoregulation. It integrates sensory input from thermoreceptors located in the skin and core tissues. These receptors detect changes in external and internal temperatures and relay this information to the hypothalamus, which then initiates appropriate physiological and behavioral responses.
The hypothalamus functions similarly to a thermostat, comparing the current body temperature to a set point and activating mechanisms to either conserve heat or dissipate it.
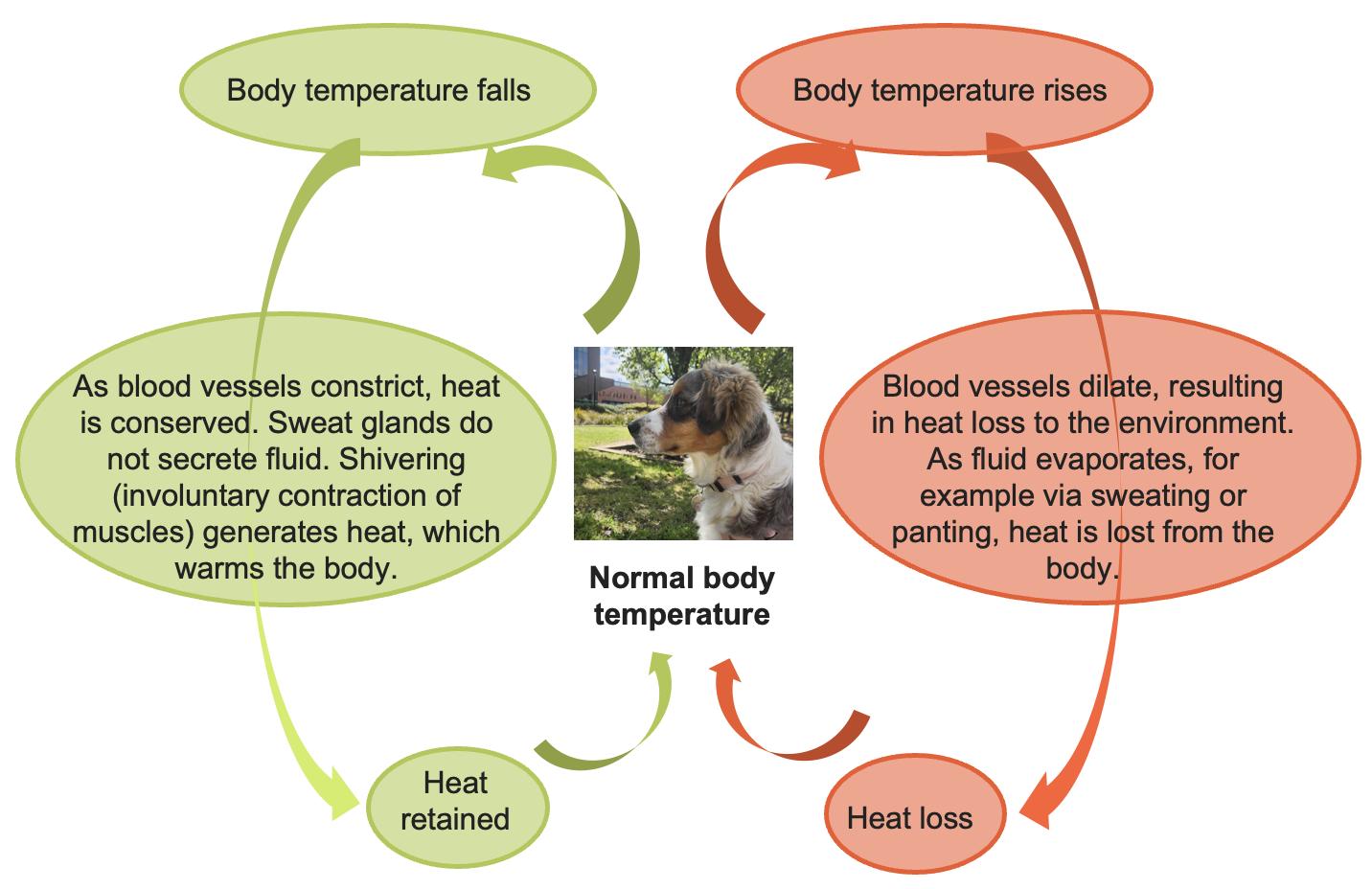
When body temperature falls below the set point, animals activate heat-generating and heat-conserving mechanisms. These include:
When body temperature rises above the set point, animals employ mechanisms to dissipate heat:
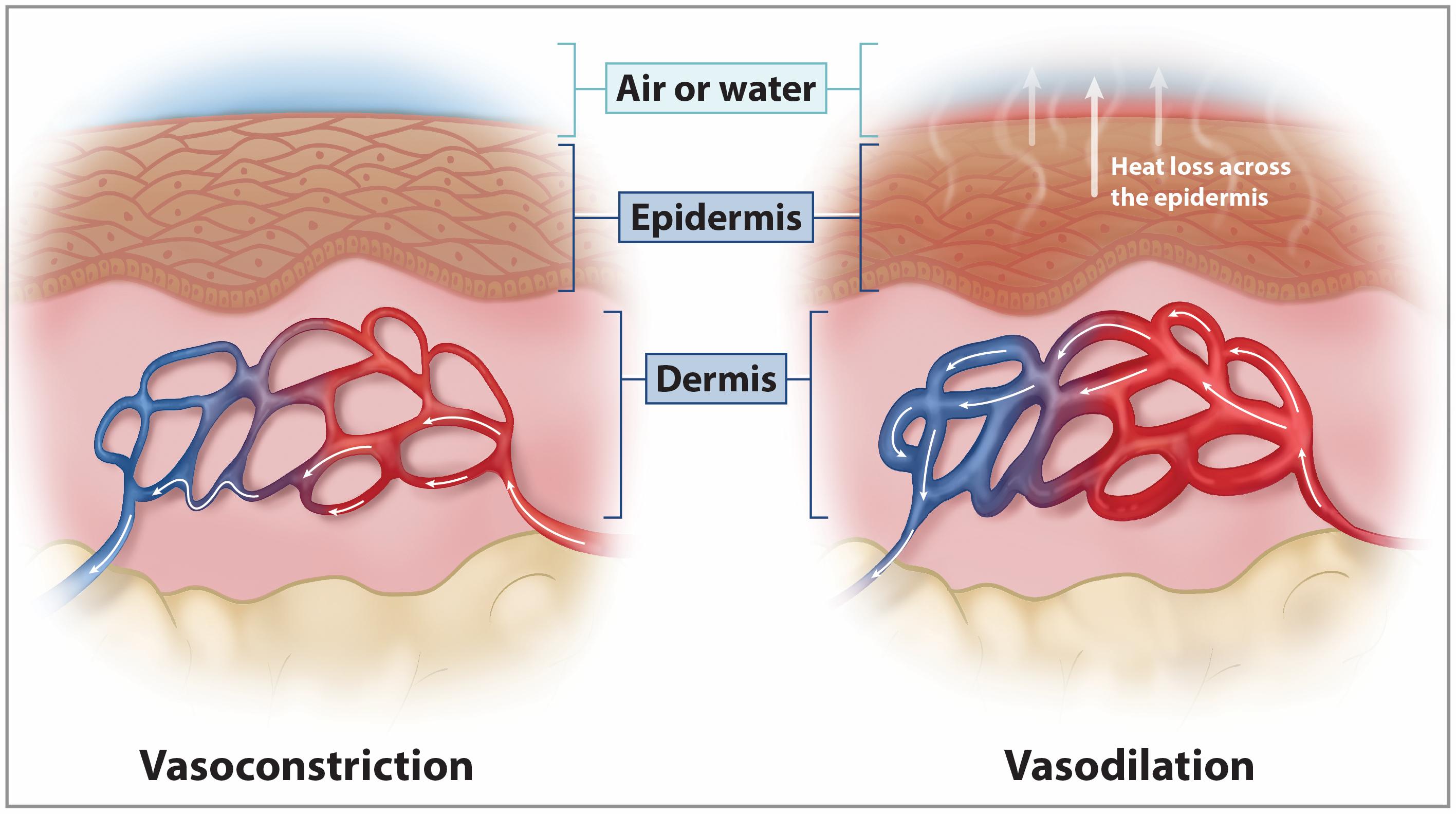
Thermoregulation is not solely a physiological process; it also involves significant behavioral adaptation. For instance, reptiles bask in the sun to raise their body temperature, while mammals may migrate or change activity patterns seasonally. These behavioral strategies often complement physiological mechanisms and can reduce the energetic cost of maintaining thermal balance.

The regulation of body temperature in animals is a complex, integrated process involving the nervous system, circulatory adjustments, metabolic activity, and behavior. Whether through internal heat production or reliance on environmental sources, animals have evolved diverse strategies to maintain thermal balance, ensuring survival and optimal physiological performance.
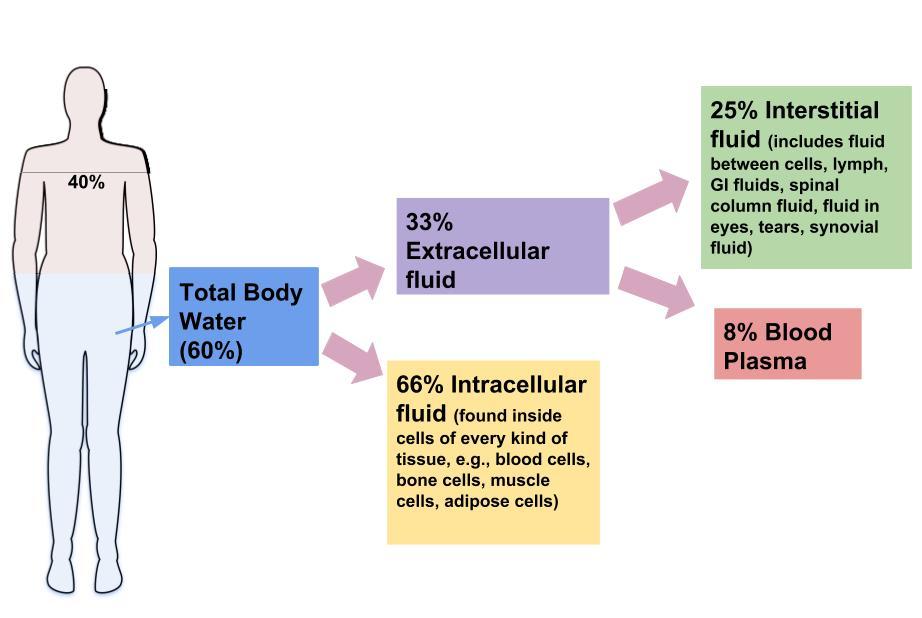
Fluid and electrolyte balance is a critical component of physiological homeostasis in animals, ensuring that cells function in a stable internal environment. Body fluids provide the medium for biochemical reactions, transport nutrients and waste products, and maintain cellular integrity. Electrolytes - such as sodium (Na⁺), potassium (K⁺), chloride (Cl⁻), and calcium (Ca²⁺) - play essential roles in nerve conduction, muscle contraction, and acid–base balance. Maintaining the correct volume, composition, and distribution of these fluids is therefore vital for survival.
Total body water is distributed into two main compartments: intracellular fluid (ICF) and extracellular fluid (ECF). The ICF, which is contained within cells, accounts for approximately two-thirds of total body water, while the ECF makes up the remaining one-third. The ECF is further divided into interstitial fluid (surrounding cells) and plasma (the liquid component of blood). The movement of water between these compartments is governed primarily by osmotic gradients, which are influenced by electrolyte concentrations. Sodium is the predominant cation in the ECF and plays a key role in regulating extracellular fluid volume, whereas potassium is the main intracellular cation and is essential for maintaining cellular function.
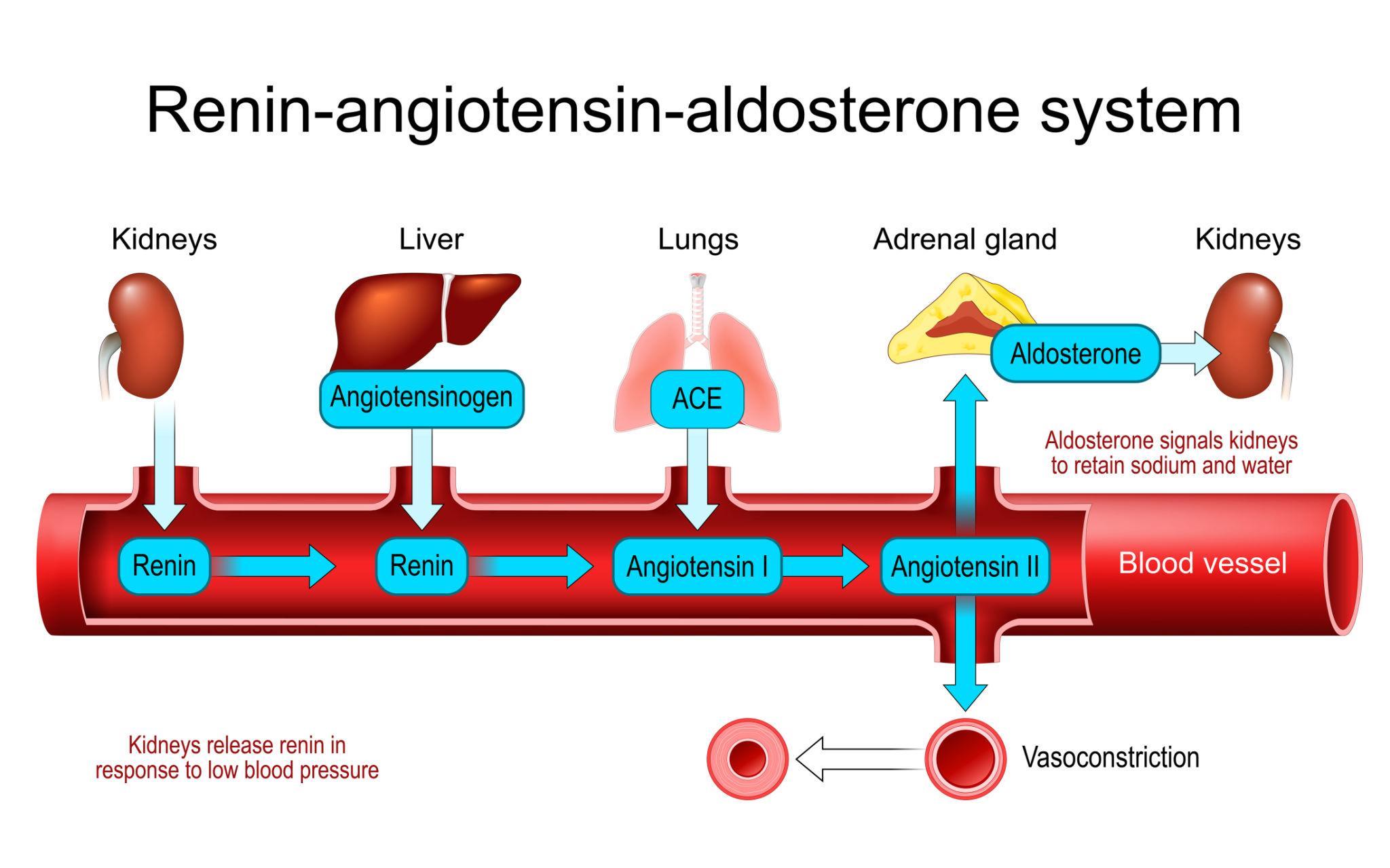
The body maintains fluid balance through a dynamic interplay between fluid intake and output. Intake occurs through drinking and feed consumption, as well as metabolic water production. Output occurs via urine, feces, respiration, and, in some species, sweating. The kidneys are the primary organs responsible for regulating fluid balance. They adjust urine volume and concentration in response to the body’s needs, conserving water during dehydration and excreting excess fluid when intake is high. This regulation is achieved through processes of filtration, reabsorption, and secretion within the nephron.
Several hormones are involved in maintaining fluid and electrolyte homeostasis:
Together, these hormonal systems allow precise control over fluid volume and electrolyte concentrations.
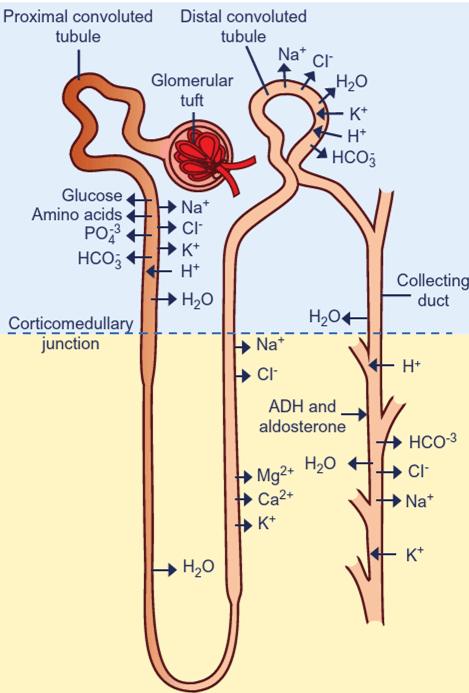
Electrolytes are regulated through dietary intake, renal excretion, and shifts between body compartments. Imbalances can significantly disrupt physiological function:
The balance of these ions is closely linked to acid–base homeostasis, as changes in hydrogen ion concentration can influence electrolyte distribution.
Fluid and electrolyte balance is closely tied to the regulation of blood pH. The body maintains acid–base balance through buffer systems, respiratory regulation (via carbon dioxide excretion), and renal mechanisms. The kidneys play a particularly important role by excreting hydrogen ions and reabsorbing bicarbonate, processes that are influenced by electrolyte levels.
Disruptions in fluid and electrolyte balance are common in veterinary practice and can arise from dehydration, diarrhea, renal disease, or endocrine disorders. For example:
Fluid and electrolyte balance is a complex, tightly regulated process involving the kidneys, endocrine system, and cellular mechanisms. By maintaining the proper distribution and composition of body fluids, animals are able to support essential physiological processes and adapt to changing internal and external conditions.
Acid–base balance refers to the regulation of hydrogen ion (H⁺) concentration in body fluids to maintain a stable pH, which is essential for normal cellular function. In most animals, particularly mammals, blood pH is tightly regulated within a narrow range (approximately 7.35–7.45). Even slight deviations from this range can disrupt enzyme activity, alter membrane potentials, and impair vital physiological processes.
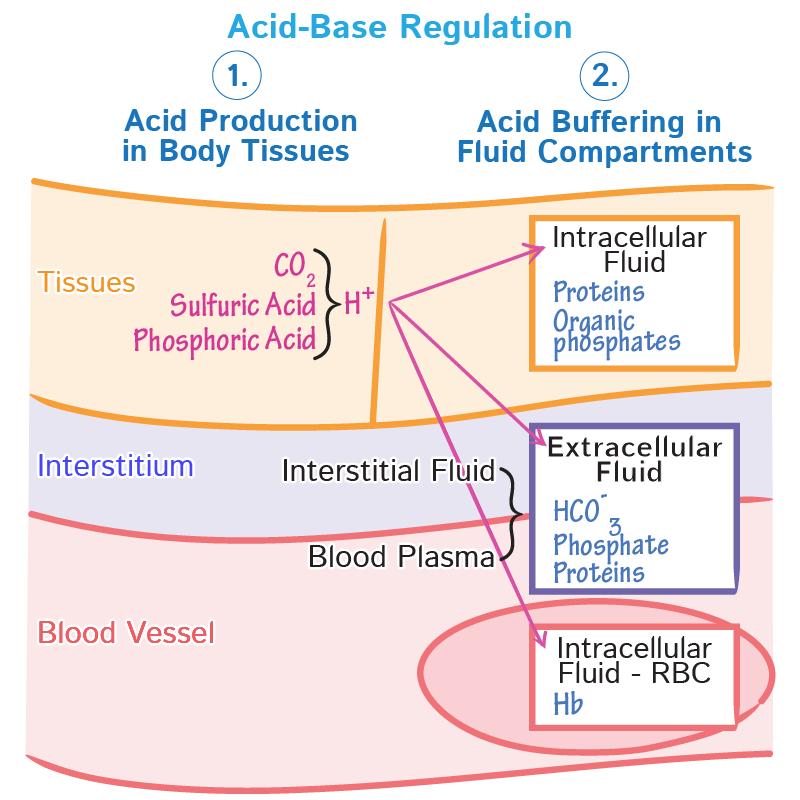
Acids are continuously produced in the body as by-products of metabolism. For example, the metabolism of carbohydrates and fats generates carbon dioxide (CO₂), which combines with water to form carbonic acid. Protein metabolism can produce stronger acids such as sulfuric and phosphoric acids. Bases, primarily in the form of bicarbonate (HCO₃⁻), act to neutralize these acids and maintain pH balance.
The first line of defense against changes in pH is the body’s buffer systems, which can rapidly bind or release hydrogen ions. The most important buffer system in extracellular fluid is the bicarbonate buffer system, involving carbonic acid (H₂CO₃) and bicarbonate (HCO₃⁻). This system minimizes sudden changes in pH by shifting the equilibrium between these components.
Other buffer systems include proteins (such as hemoglobin) and phosphate buffers, which are particularly important within cells and in renal tubules.
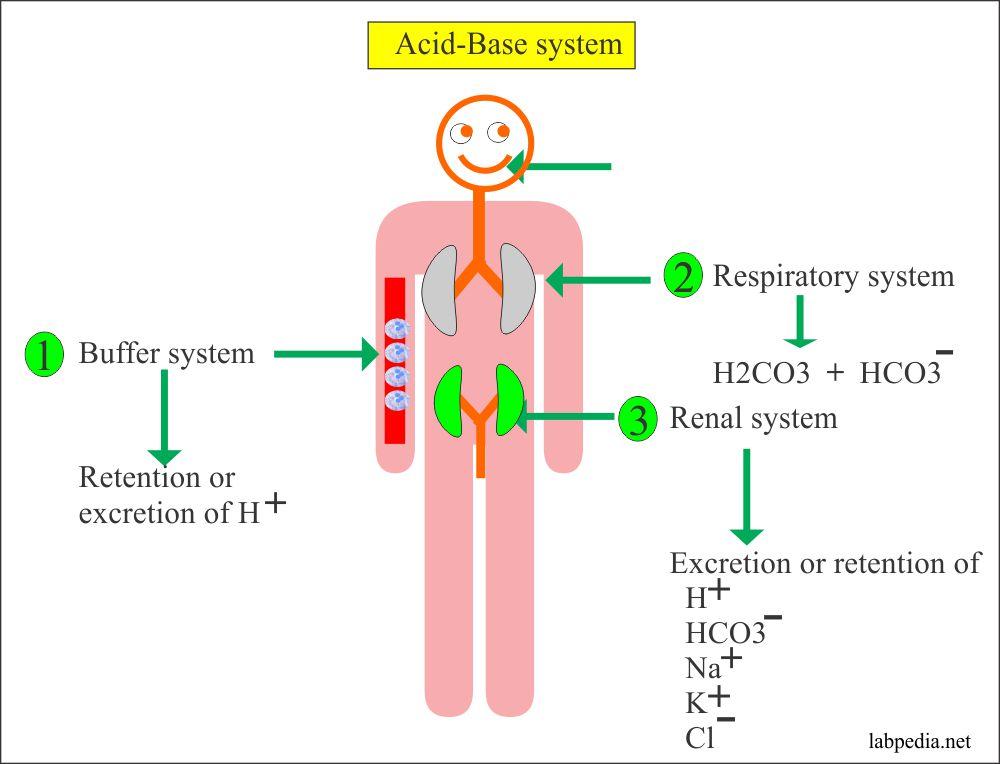
The respiratory system plays a key role in regulating acid–base balance by controlling the elimination of CO₂. Increased respiration (hyperventilation) leads to greater CO₂ excretion, reducing carbonic acid levels and increasing pH (making the blood more alkaline). Conversely, decreased respiration (hypoventilation) results in CO₂ retention, increasing acidity. This regulation occurs rapidly and is coordinated by respiratory centers in the brainstem, which respond to changes in blood pH and CO₂ levels.
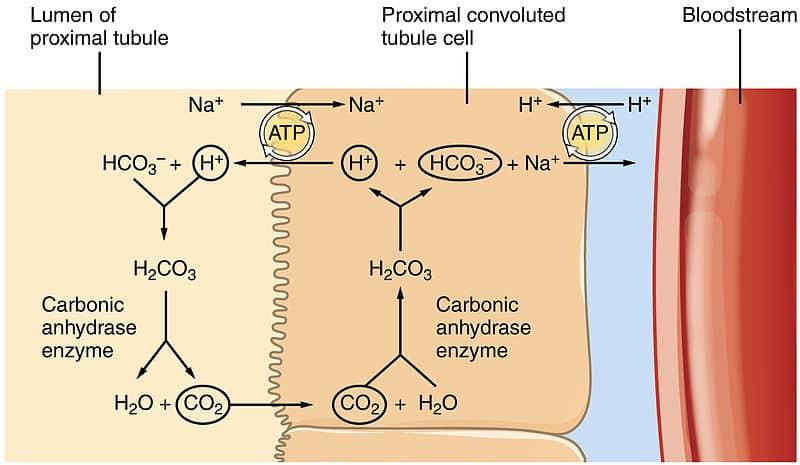
The kidneys provide long-term regulation of acid–base balance. They maintain pH by:
Although slower than respiratory adjustments, renal mechanisms are highly effective and essential for sustained pH control.
Disruptions in acid–base balance are broadly classified into:
The body attempts to compensate for these disturbances through respiratory or renal adjustments to restore normal pH.
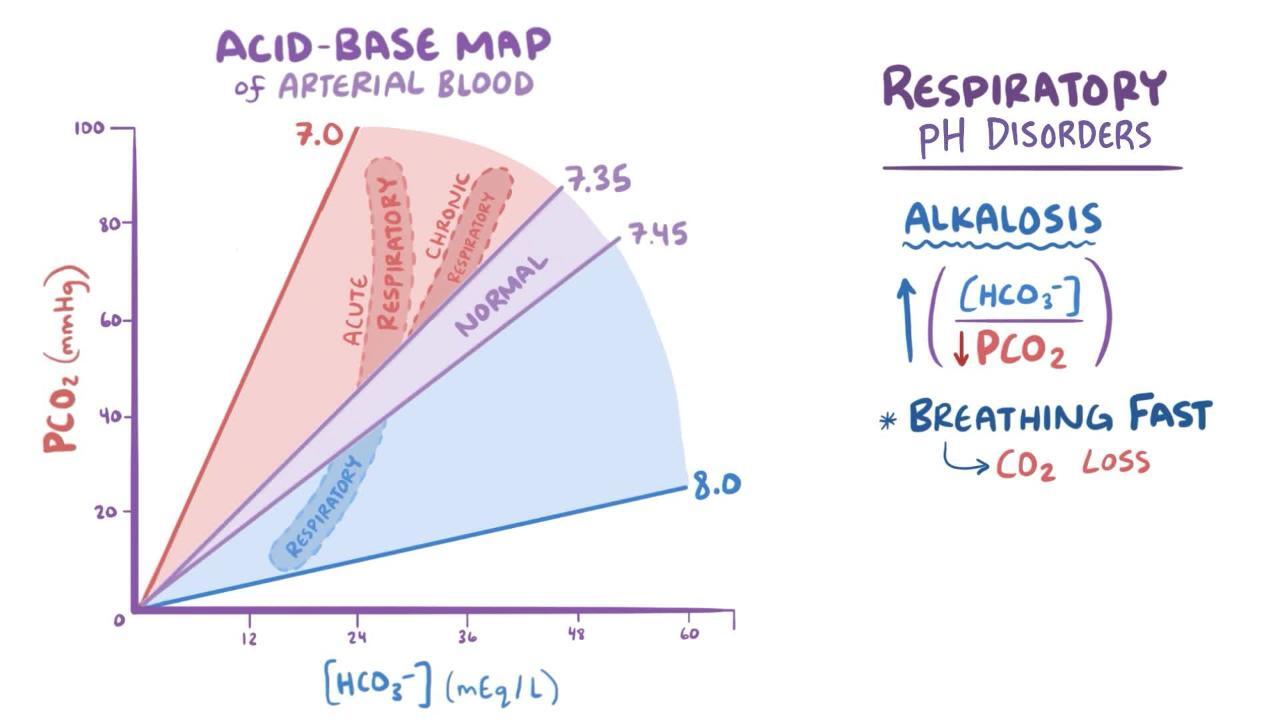
In veterinary medicine, acid–base imbalances are commonly encountered in conditions such as gastrointestinal disease, respiratory disorders, renal failure, and metabolic disturbances. For example, severe diarrhea in calves can lead to metabolic acidosis due to bicarbonate loss, while respiratory infections may impair CO₂ elimination. Diagnosis typically involves blood gas analysis and electrolyte measurement, allowing veterinarians to determine the nature of the imbalance and guide appropriate treatment.
Acid–base balance is a tightly regulated process involving buffer systems, the respiratory system, and renal function. Together, these mechanisms ensure that body pH remains within a narrow, life-sustaining range. Understanding these principles is essential in veterinary medicine for the diagnosis and management of a wide range of clinical conditions affecting animal health.
Energy regulation in animals centers on maintaining a stable supply of glucose, which serves as a primary energy source for many tissues, especially the brain and red blood cells. Because both excessive and insufficient blood glucose levels can be harmful, animals have evolved tightly controlled mechanisms to balance glucose production, storage, and utilization. This process is essential for sustaining metabolic homeostasis and supporting physiological functions.
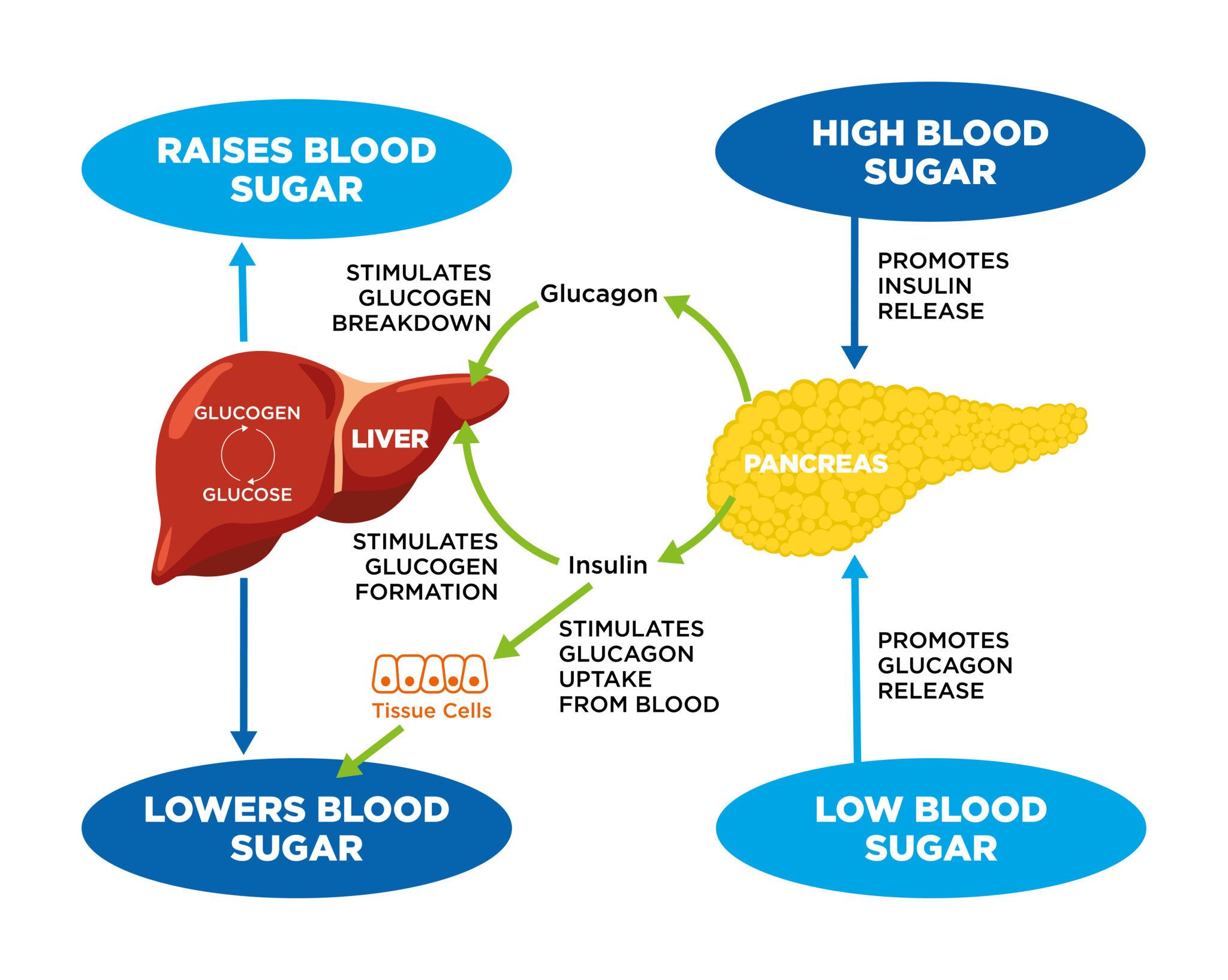
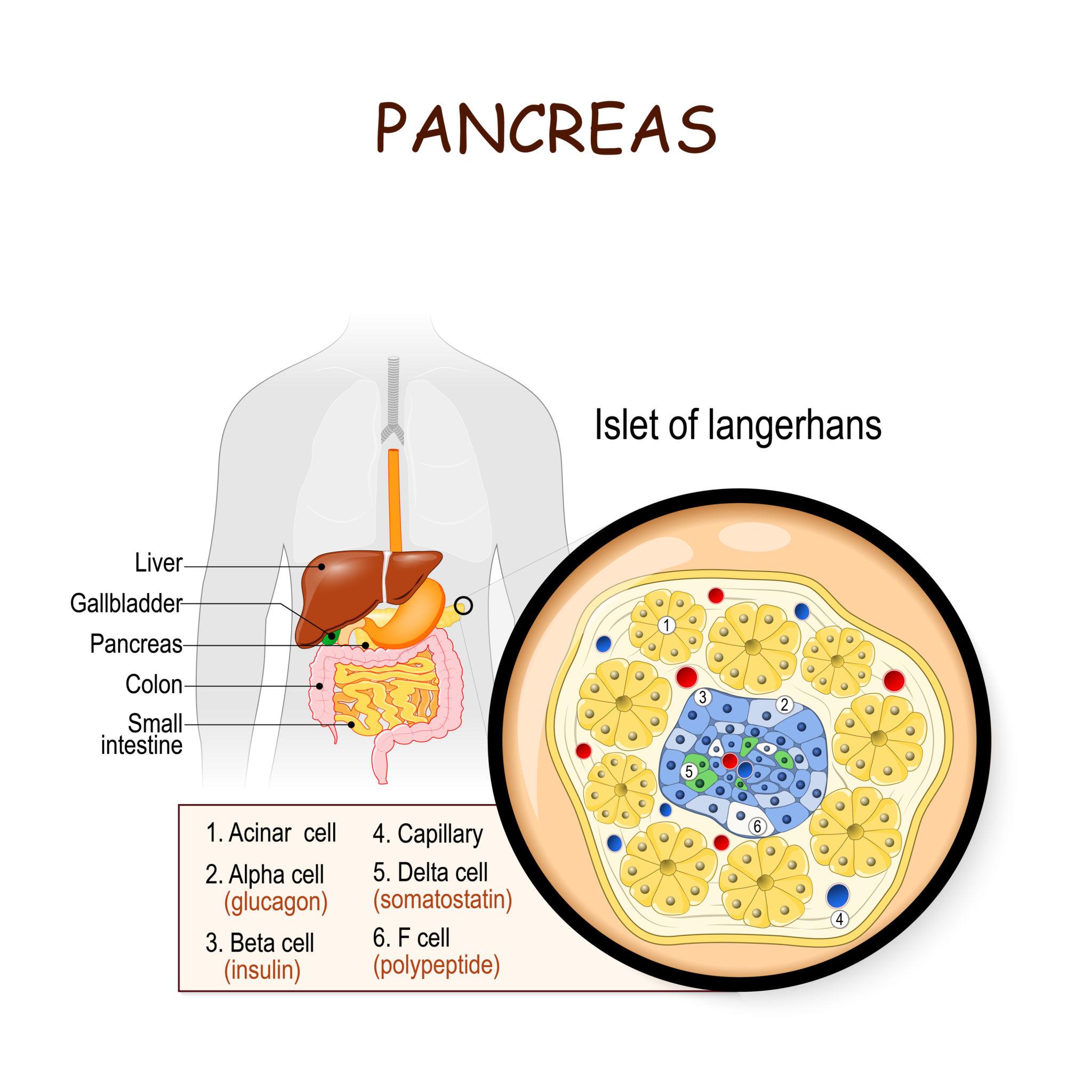
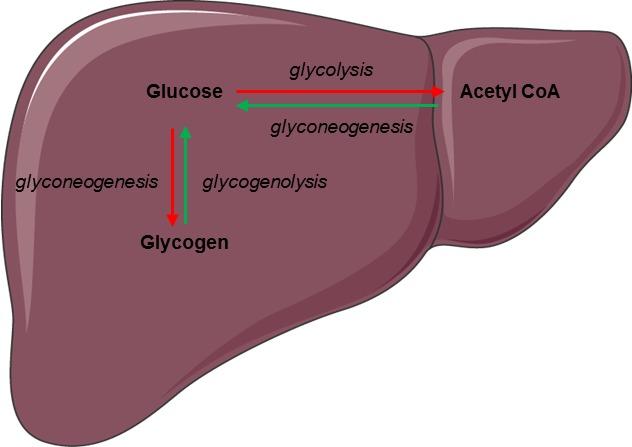
Glucose is derived from dietary carbohydrates, hepatic glycogen stores, and endogenous synthesis. After a meal, carbohydrates are digested and absorbed into the bloodstream, raising blood glucose levels. Excess glucose is stored in the liver and muscles as glycogen through glycogenesis . During periods of fasting or increased energy demand, glucose is released into the bloodstream through glycogenolysis (breakdown of glycogen) and gluconeogenesis, a process in which new glucose is synthesized from non-carbohydrate sources such as amino acids, glycerol, and lactate. The liver is the primary organ responsible for maintaining blood glucose levels, although the kidneys can also contribute during prolonged fasting.
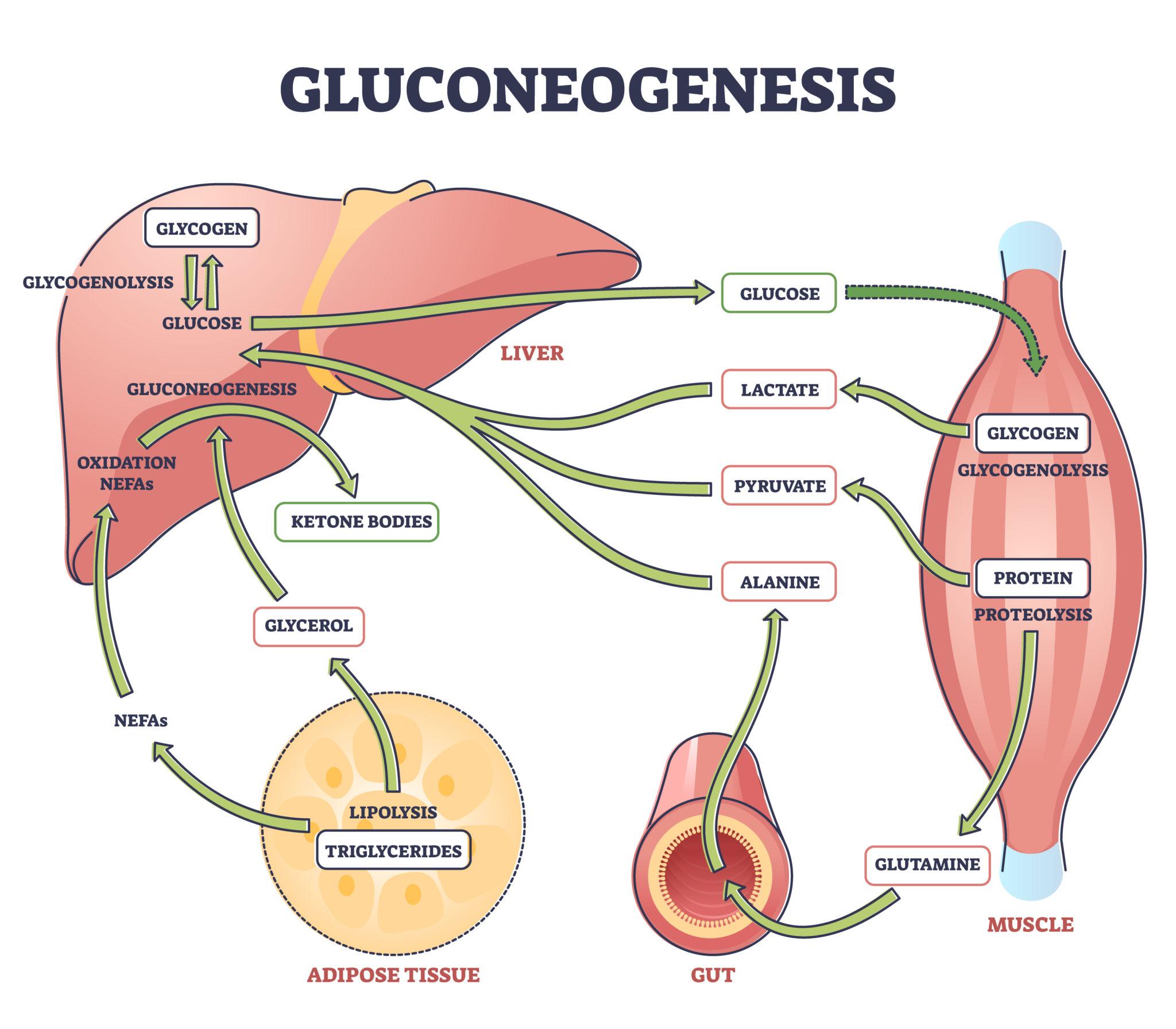
The regulation of blood glucose is primarily controlled by hormones produced by the pancreas, specifically within the islets of Langerhans:
These two hormones act antagonistically to maintain glucose within a narrow physiological range.
Other hormones also contribute to glucose regulation:
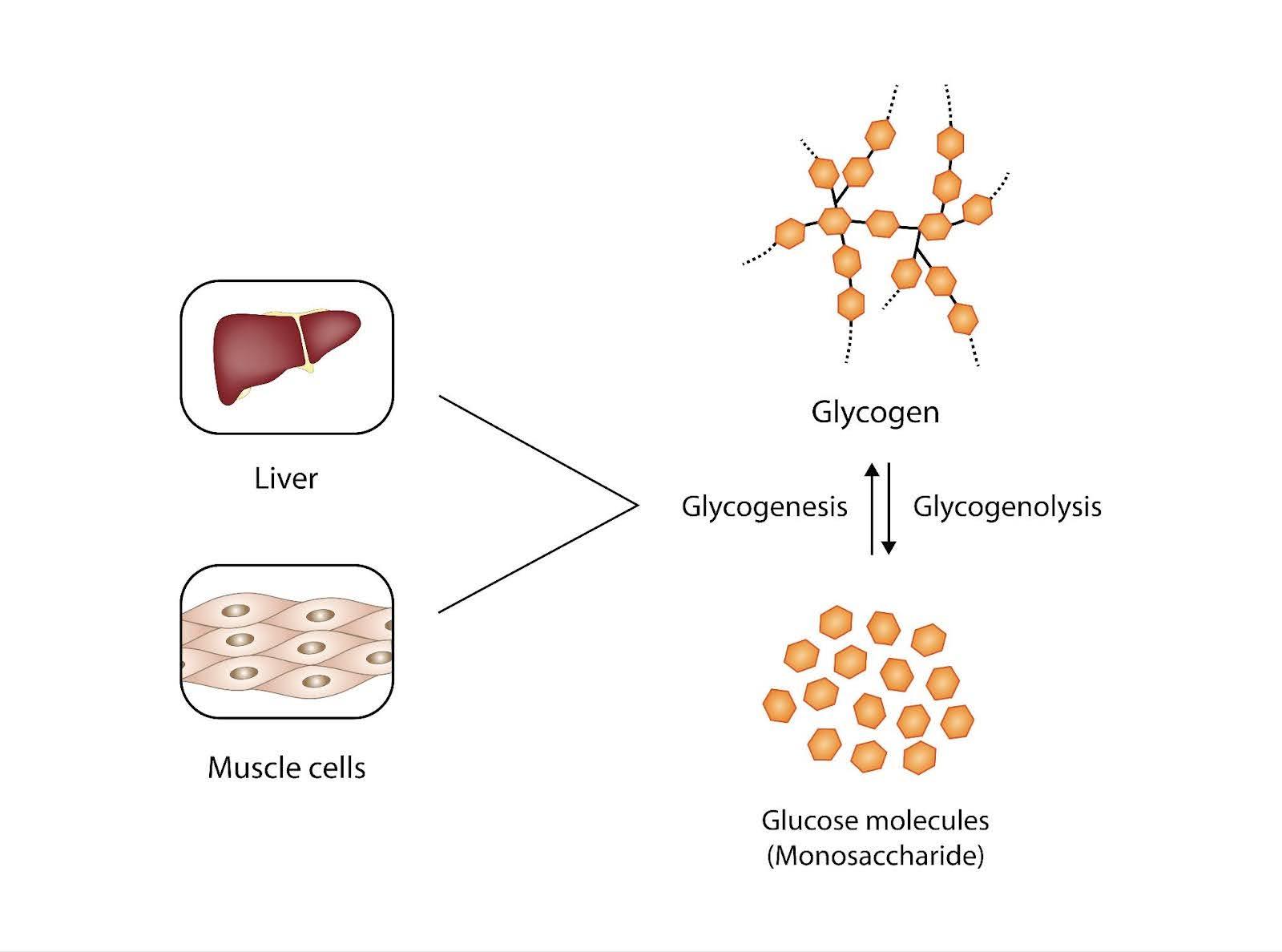
The liver plays a central role in glucose homeostasis. It acts as a buffer, storing excess glucose after feeding and releasing it during fasting. Hepatic enzymes regulate the interconversion of glucose and glycogen, as well as the synthesis of glucose from non-carbohydrate precursors.
Different tissues use glucose in distinct ways:
In ruminants, glucose metabolism differs significantly because dietary carbohydrates are fermented in the rumen to volatile fatty acids. As a result, glucose is largely produced through gluconeogenesis rather than direct absorption, highlighting species-specific adaptations in energy regulation.
Disorders of glucose regulation are important in veterinary medicine:
Glucose regulation is part of a broader energy balance system that includes lipid and protein metabolism. When glucose is abundant, energy is stored; when it is scarce, alternative energy sources are mobilized. This integration allows animals to adapt to changes in diet, activity level, and physiological state.
Energy (glucose) regulation in animals is a complex, hormone-driven process involving the pancreas, liver, and peripheral tissues. Through coordinated control of glucose storage, production, and utilization, animals maintain a stable energy supply necessary for survival. A clear understanding of these mechanisms is essential in veterinary medicine for managing metabolic diseases and optimizing animal health and productivity.
The balance of oxygen (O₂) and carbon dioxide (CO₂) is essential for maintaining cellular respiration and overall metabolic homeostasis in animals. Oxygen is required for aerobic energy production, while carbon dioxide is a metabolic waste product that must be efficiently removed to prevent acid–base disturbances. The regulation of these gases involves the coordinated function of the respiratory and circulatory systems.
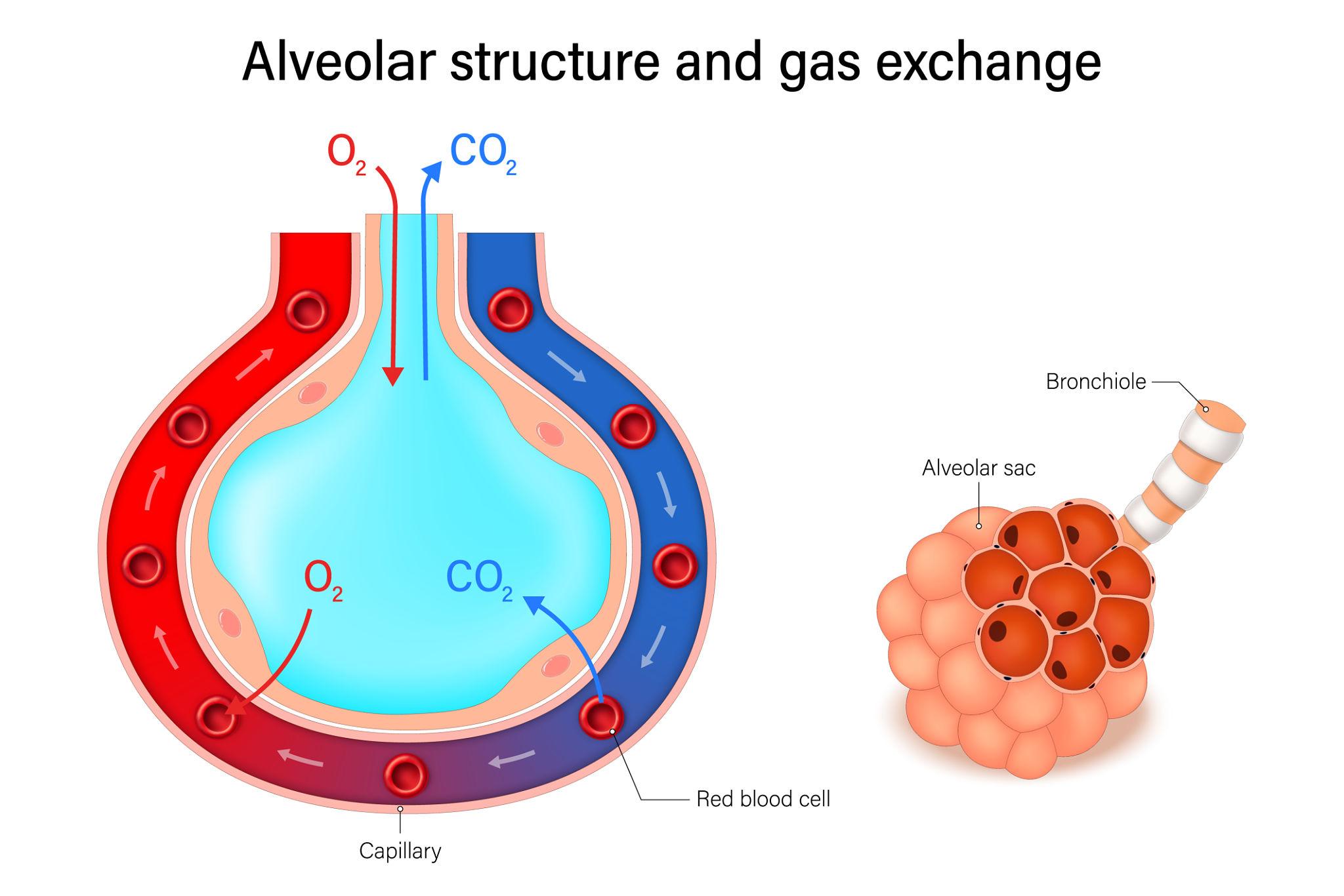
Oxygen enters the body through the process of ventilation and diffuses across the respiratory surfaces—such as the alveoli in mammals—into the bloodstream. The lungs provide a large surface area and a thin barrier to facilitate efficient gas exchange.
Once in the blood, oxygen is transported primarily bound to hemoglobin within red blood cells. Hemoglobin has a high affinity for oxygen in the lungs, where oxygen concentration is high, and releases it in peripheral tissues where oxygen levels are lower. This relationship is described by the oxygen–hemoglobin dissociation curve, which is influenced by factors such as pH, temperature, and CO₂ concentration.

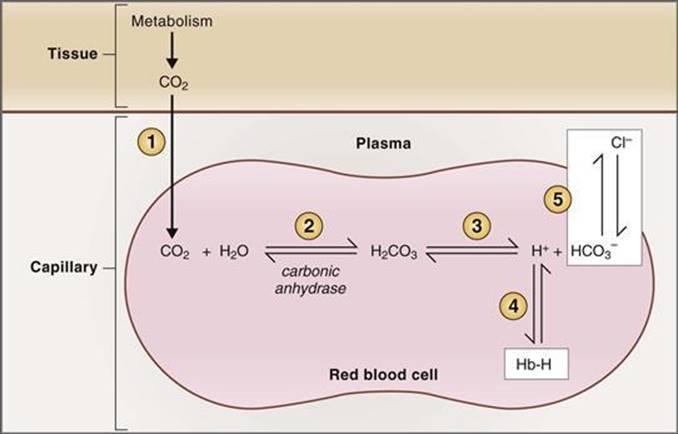
Carbon dioxide, produced during cellular metabolism, diffuses from tissues into the blood and is transported to the lungs for elimination. It is carried in three main forms:
The conversion of CO₂ to bicarbonate occurs in red blood cells and is facilitated by the enzyme carbonic anhydrase. This reaction also plays a key role in acid–base balance.
The lungs are the primary organs responsible for maintaining oxygen and carbon dioxide balance. Through ventilation, the lungs regulate the amount of oxygen entering the body and the amount of carbon dioxide being expelled.
Breathing is controlled by respiratory centers in the brainstem, which respond to changes in blood CO₂ levels, pH, and, to a lesser extent, oxygen levels. An increase in CO₂ concentration or a decrease in pH stimulates an increase in ventilation, enhancing CO₂ removal and oxygen uptake.
Efficient gas exchange depends not only on ventilation but also on adequate blood flow (perfusion) to the lungs. The matching of ventilation and perfusion ensures that oxygen is effectively absorbed and carbon dioxide is removed. Imbalances in this relationship, known as ventilation–perfusion (V/Q) mismatch, can impair gas exchange and lead to hypoxemia.
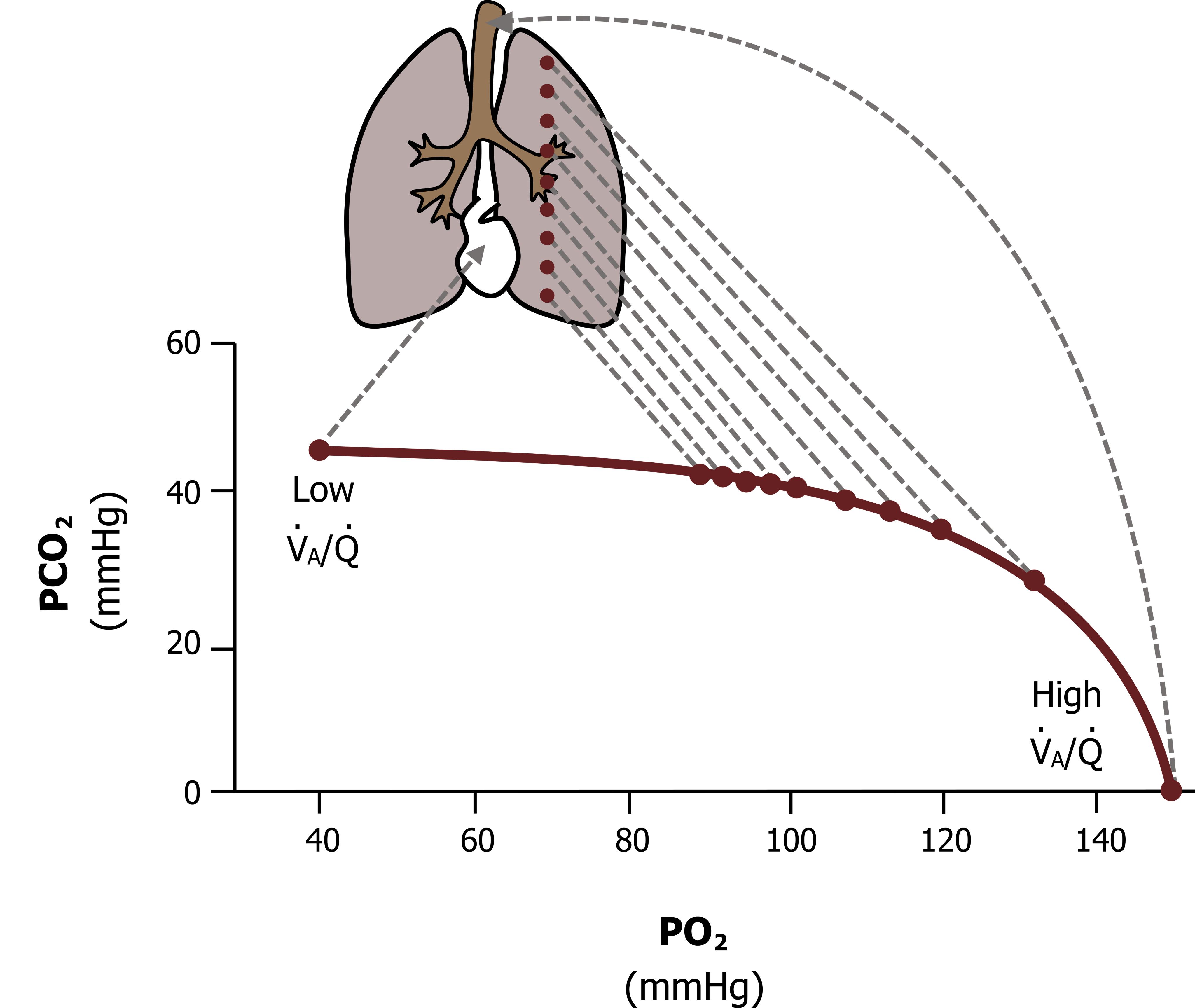
The balance of oxygen and carbon dioxide is closely linked to acid–base regulation. Elevated CO₂ levels increase the formation of carbonic acid, lowering blood pH, while reduced CO₂ levels have the opposite effect. This highlights the integration between respiratory function and pH regulation. Additionally, cardiovascular function plays a critical role by ensuring that oxygenated blood is delivered to tissues and carbon dioxide is transported back to the lungs. Any impairment in circulation can therefore disrupt gas balance.
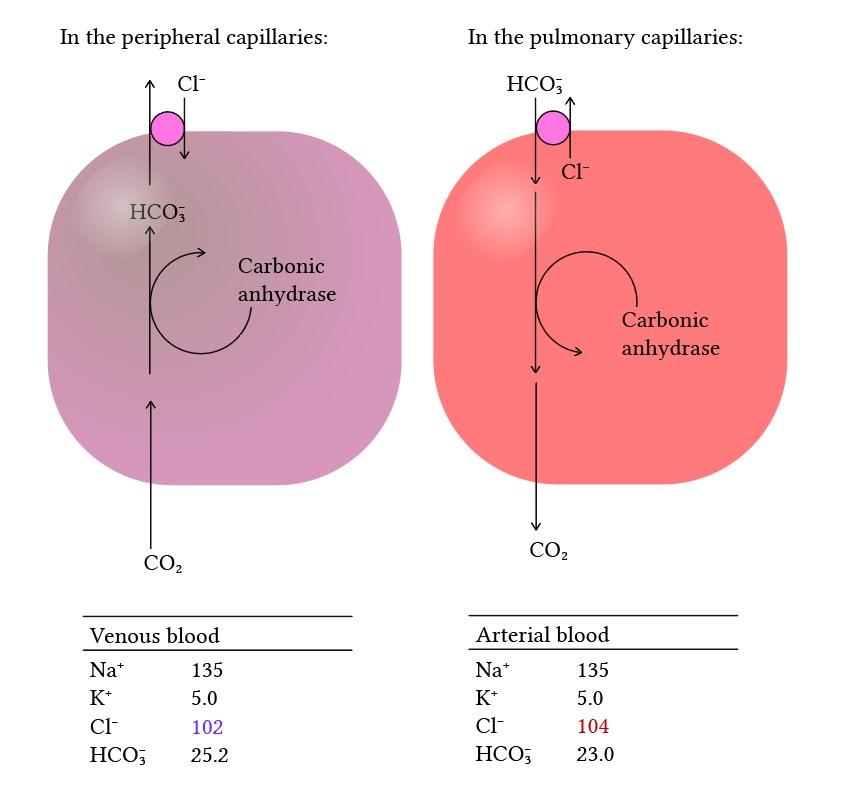
Disorders of oxygen and carbon dioxide balance are common in veterinary medicine and can arise from respiratory, cardiovascular, or metabolic causes:
Conditions such as pneumonia, airway obstruction, or pulmonary edema can significantly impair gas exchange, leading to life-threatening consequences if not managed promptly.
Different animal species exhibit variations in respiratory anatomy and physiology. For example, birds possess a highly efficient respiratory system with unidirectional airflow, while fish rely on gills for gas exchange in water. These adaptations reflect the diverse environmental challenges animals face in maintaining oxygen and carbon dioxide balance.
Oxygen and carbon dioxide balance in animals is maintained through the integrated function of the respiratory and circulatory systems. Efficient gas exchange, transport, and regulation ensure that tissues receive adequate oxygen for metabolism while removing carbon dioxide to prevent toxicity and acid–base imbalance. Understanding these processes is essential in veterinary medicine for diagnosing and managing respiratory and systemic disorders.
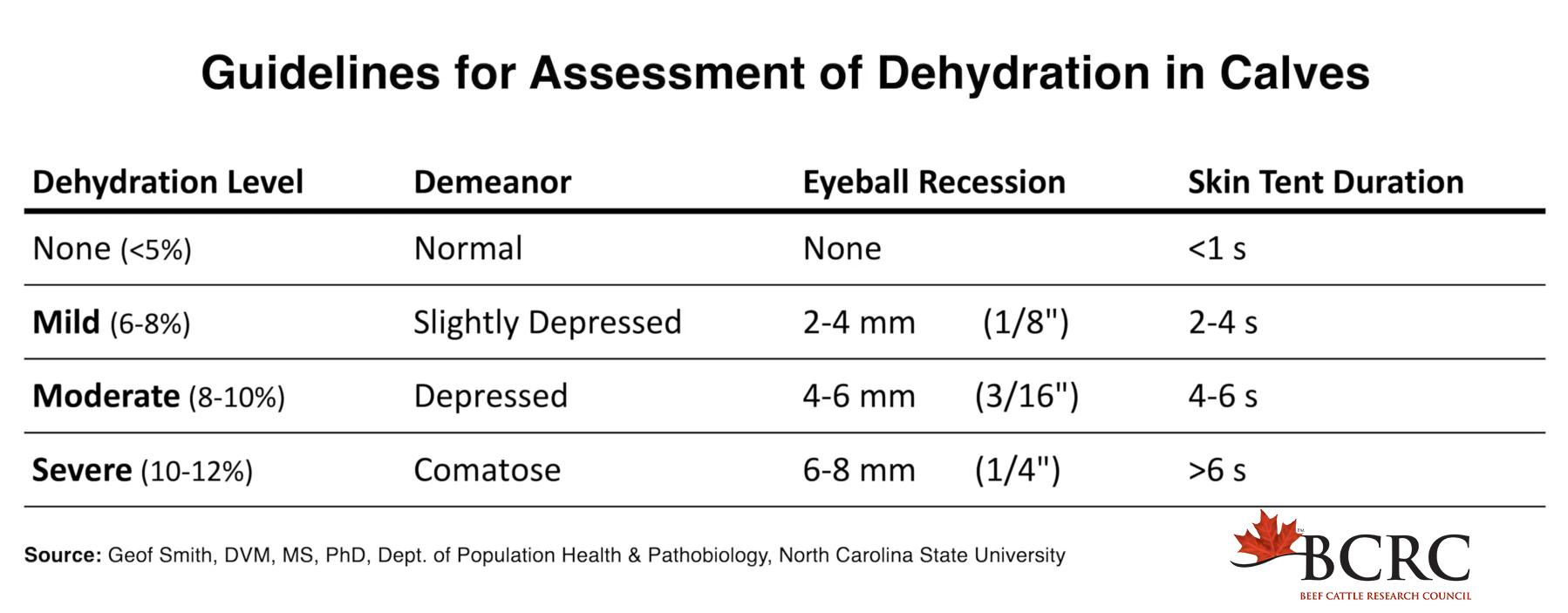
Dehydration occurs when fluid loss exceeds fluid intake, leading to a reduction in total body water and disruption of fluid balance. Within the framework of homeostasis, dehydration affects both fluid volume and electrolyte concentration, impairing cellular function and circulation. Common causes include diarrhea, vomiting, excessive sweating, inadequate water intake, and disease conditions affecting fluid retention. As dehydration progresses, there is a decrease in plasma volume, resulting in reduced tissue perfusion and potential organ dysfunction. Electrolyte imbalances, particularly involving sodium and potassium, further complicate the condition. Clinically, animals may present with sunken eyes, dry mucous membranes, reduced skin elasticity, and lethargy. Severe dehydration can lead to hypovolemic shock. Restoration of homeostasis involves fluid replacement therapy (oral or intravenous) and correction of electrolyte imbalances.
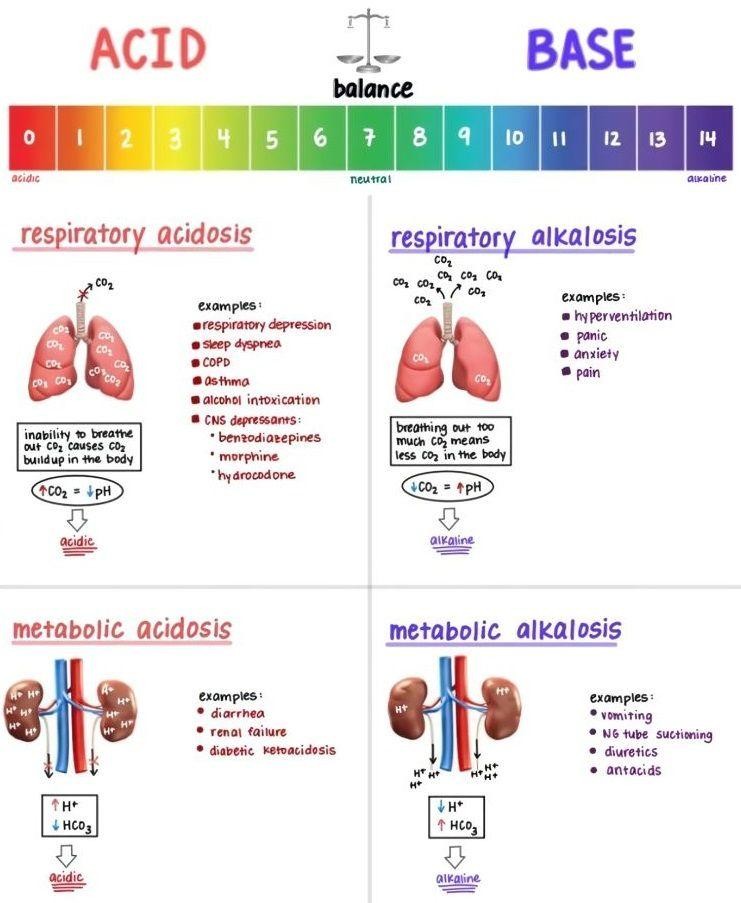
Acidosis and alkalosis refer to disturbances in acid–base balance, where blood pH falls below or rises above the normal physiological range, respectively. These conditions directly challenge homeostasis by altering enzyme activity and cellular metabolism. Acidosis may result from increased acid production (e.g., lactic acidosis), loss of bicarbonate (e.g., diarrhea), or impaired CO₂ elimination (respiratory acidosis). Alkalosis may occur due to excessive loss of acids (e.g., vomiting) or increased CO₂ loss through hyperventilation (respiratory alkalosis). The body attempts to restore balance through buffering systems, respiratory adjustments, and renal compensation. However, severe or prolonged imbalances can lead to neurological, muscular, and cardiovascular dysfunction.
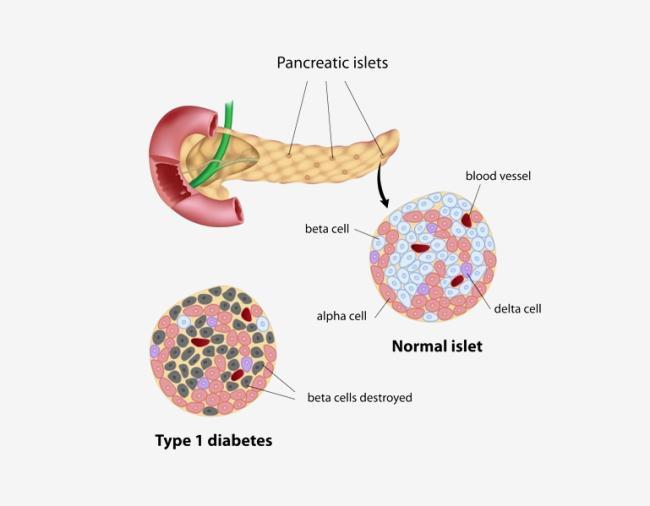
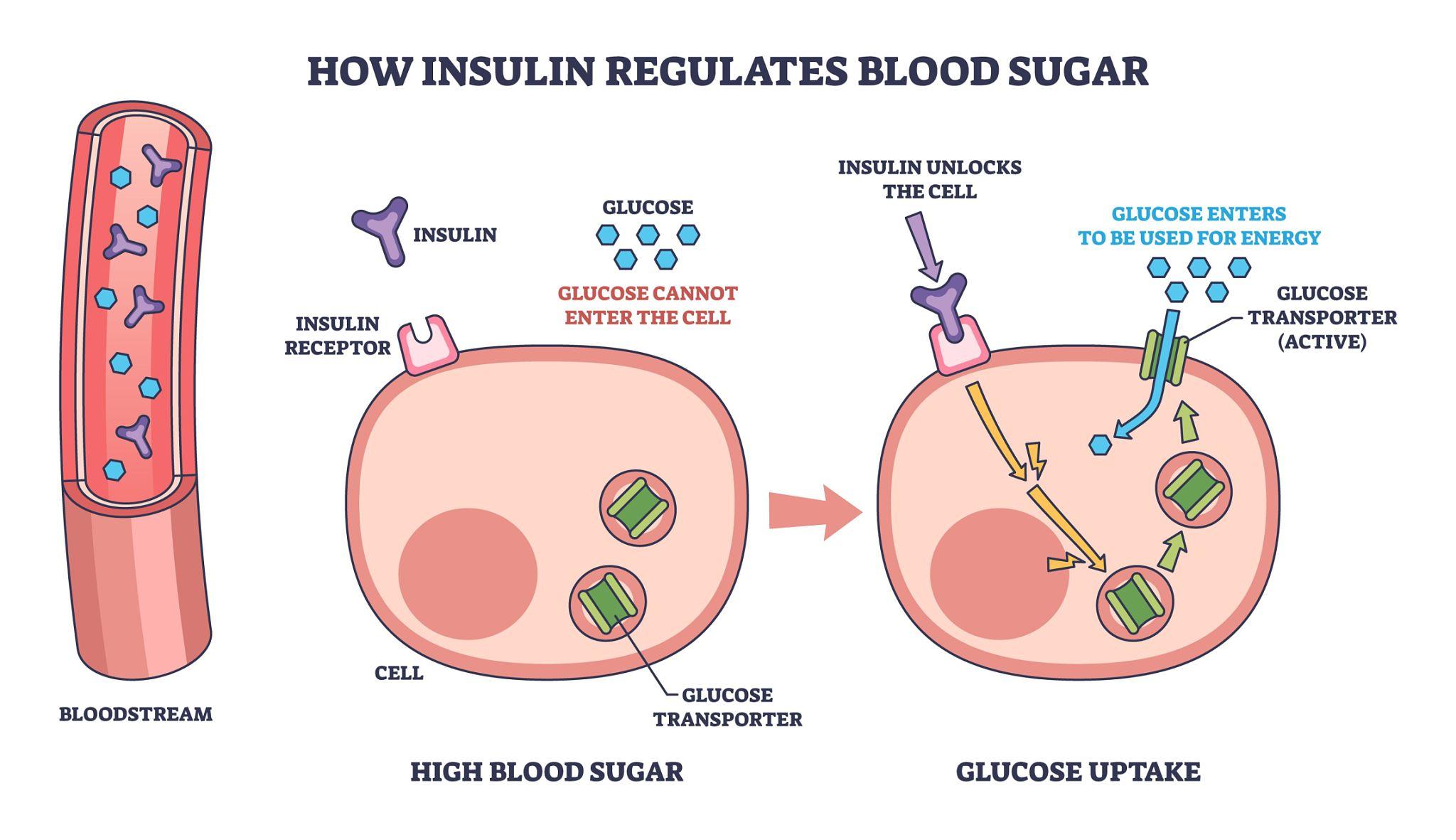
Diabetes Mellitus is a metabolic disorder characterized by chronic hyperglycemia due to insufficient insulin production or impaired insulin action. It represents a failure of glucose homeostasis. In affected animals, glucose cannot effectively enter cells, leading to elevated blood glucose levels and reduced cellular energy availability. The body compensates by increasing fat and protein breakdown, which may result in weight loss and, in severe cases, ketoacidosis. Common clinical signs include excessive thirst (polydipsia), increased urination (polyuria), increased appetite (polyphagia), and weight loss. Management involves insulin therapy, dietary control, and regular monitoring of blood glucose levels.
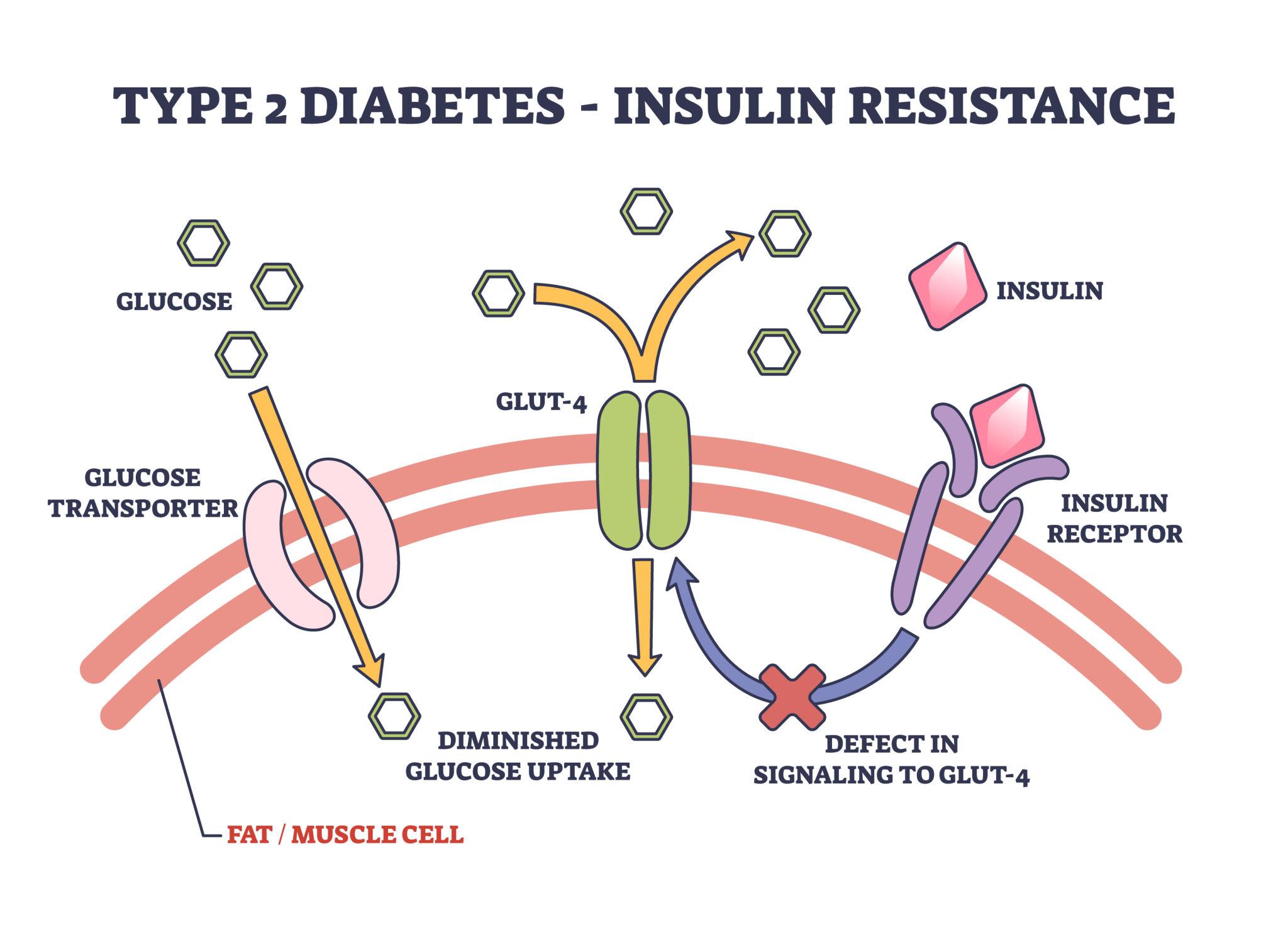
Shock is a life-threatening condition characterized by inadequate tissue perfusion and oxygen delivery, leading to cellular and organ dysfunction. It represents a severe breakdown of circulatory and metabolic homeostasis. There are several types of shock, including hypovolemic (due to fluid loss), cardiogenic (due to heart failure), distributive (e.g., septic shock), and obstructive shock. Regardless of the cause, the result is reduced oxygen delivery to tissues and impaired removal of metabolic waste. The body initially compensates through increased heart rate, vasoconstriction, and hormonal responses. However, if the underlying cause is not corrected, shock progresses to irreversible organ damage and death. Clinical signs include rapid pulse, pale mucous membranes, prolonged capillary refill time, and altered mental status. Immediate veterinary intervention-often involving fluid therapy, oxygen supplementation, and treatment of the underlying cause-is critical for survival.
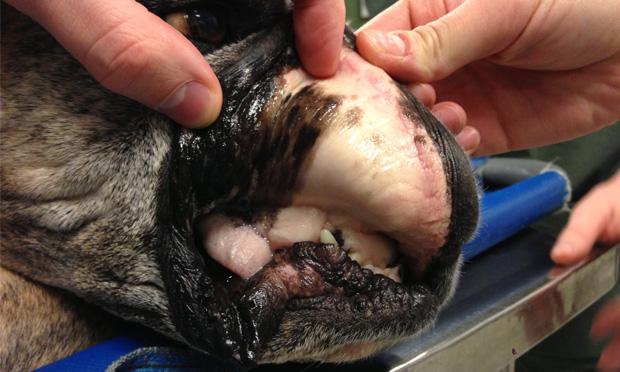
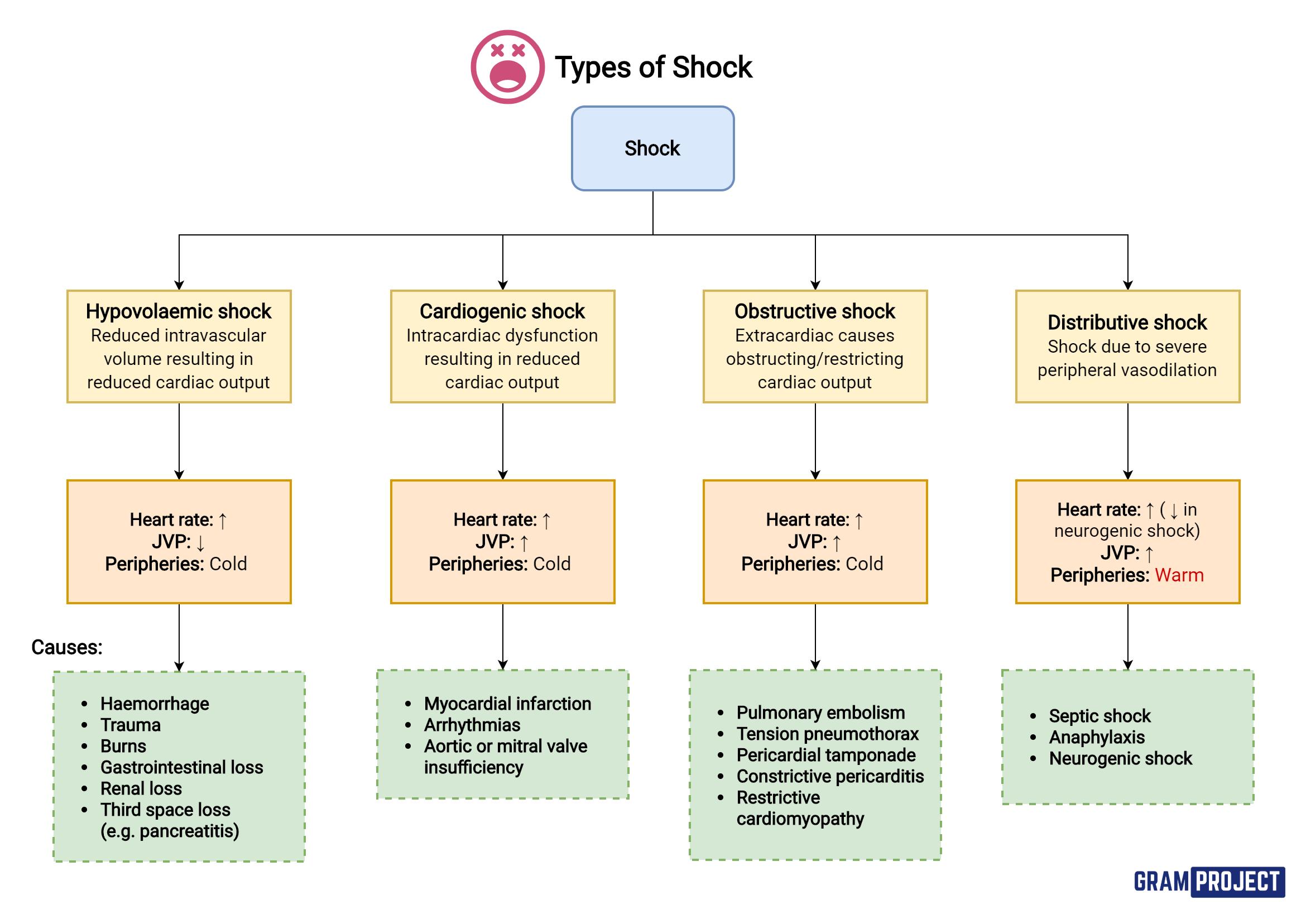
Hypothermia and hyperthermia are disturbances in thermoregulation, where body temperature falls below or rises above the normal range, respectively. Hypothermia occurs when heat loss exceeds heat production, commonly seen in neonates, small animals, or those exposed to cold environments. It leads to slowed metabolism, reduced cardiac output, and impaired neurological function. Hyperthermia, on the other hand, results from excessive heat production or inadequate heat dissipation. Heat stress or heat stroke is a common cause, particularly in animals with limited cooling mechanisms. This condition can lead to protein denaturation, organ failure, and death if not managed promptly. The body normally regulates temperature through mechanisms such as vasodilation, vasoconstriction, sweating, and behavioral responses. When these mechanisms fail, clinical intervention is required. Treatment involves gradual warming in hypothermia or controlled cooling in hyperthermia, along with supportive care.

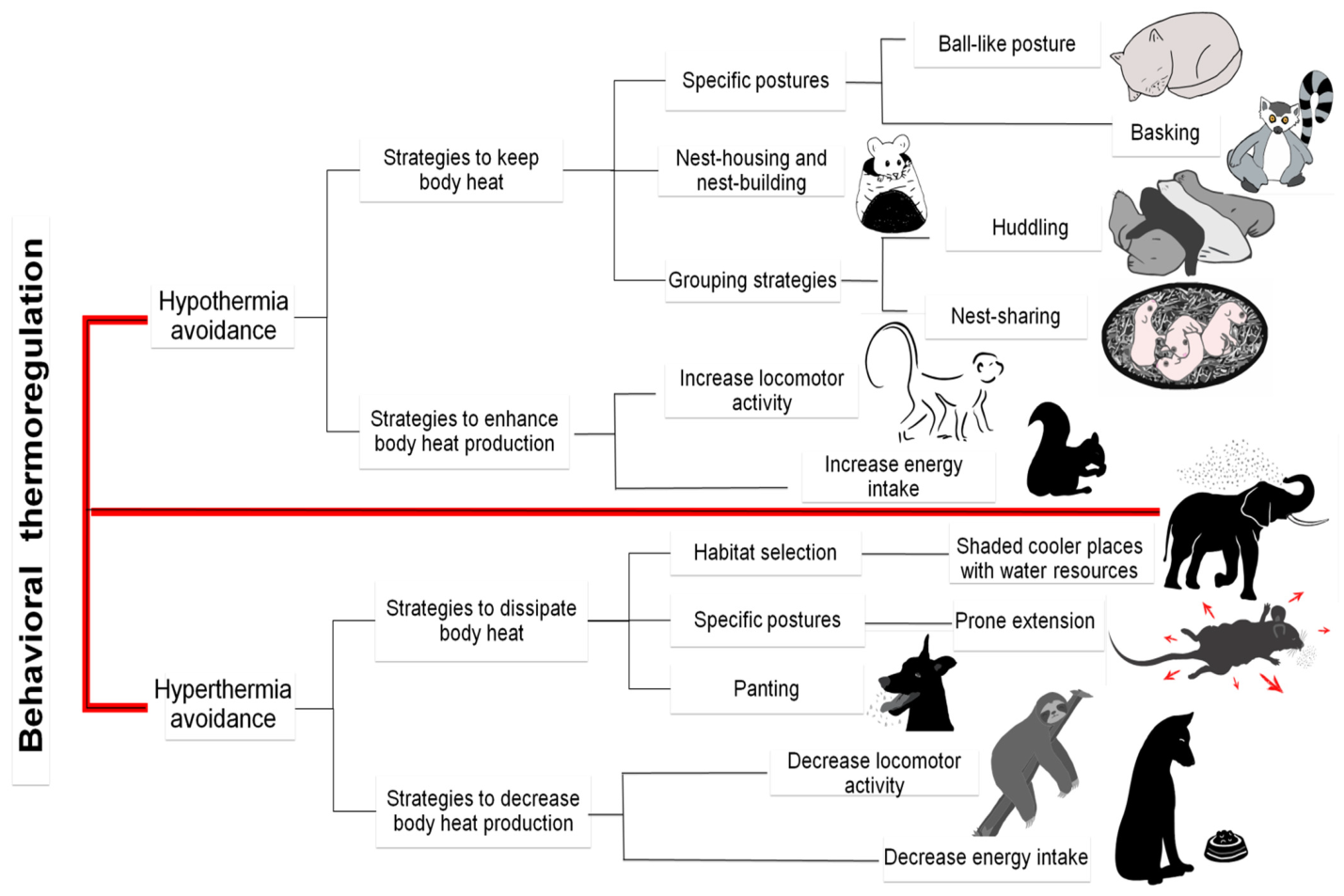
Stress is a physiological and behavioral response to internal or external challenges (stressors) that threaten an animal’s stability. While short-term stress responses are adaptive and help restore balance, prolonged or chronic stress can disrupt homeostasis, leading to significant negative effects on health, productivity, and welfare.
The stress response in animals is primarily mediated by two interconnected systems:
The hypothalamus initiates the process by releasing signals that activate both pathways. The SAM system triggers the release of catecholamines (e.g., adrenaline), increasing heart rate, blood pressure, and energy availability. Meanwhile, the HPA axis leads to the release of cortisol from the adrenal cortex.

Acute stress is short-lived and often beneficial. It prepares the animal for a 'fight-or-flight' response by mobilizing energy reserves, enhancing alertness, and temporarily suppressing non-essential functions such as digestion and reproduction.
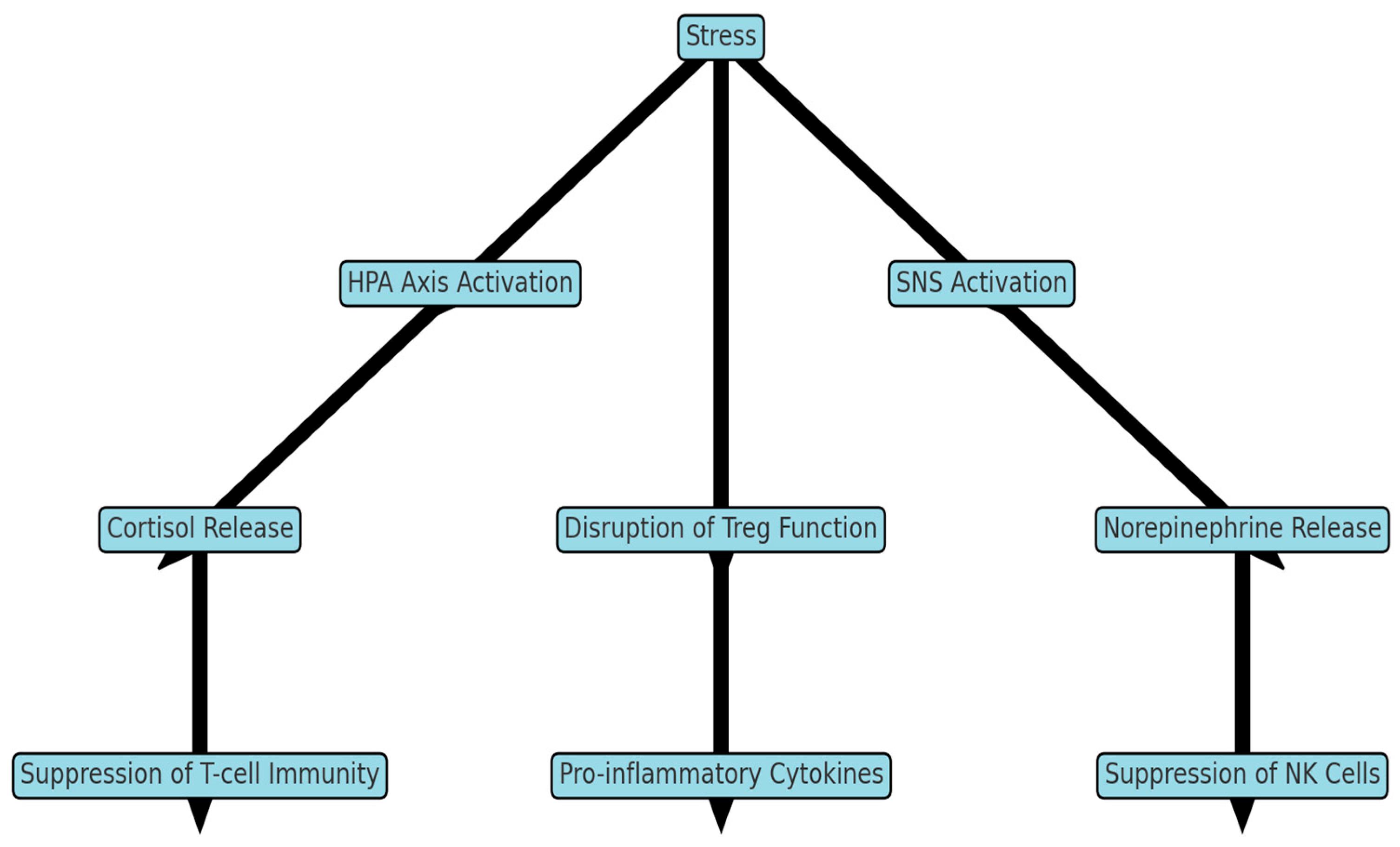
In contrast, chronic stress results from prolonged exposure to stressors such as poor nutrition, overcrowding, disease, or environmental extremes. Persistent elevation of cortisol can have harmful effects, including:
Stress affects multiple body systems, disrupting homeostasis:
These widespread effects highlight how stress can destabilize the internal environment of the body.

Animals may also exhibit behavioral changes under stress, such as aggression, withdrawal, reduced feed intake, or abnormal repetitive behaviors. Environmental factors—such as handling, transport, housing conditions, and social interactions—play a significant role in determining stress levels, particularly in livestock and captive animals.
In veterinary medicine and animal production systems, stress is a major concern. For example, transport stress in livestock can lead to weight loss, reduced meat quality, and increased disease incidence. In companion animals, chronic stress may contribute to behavioral disorders and chronic illness. Managing stress through proper handling, nutrition, housing, and health care is essential for maintaining homeostasis and promoting animal welfare.
Stress is a powerful modifier of homeostasis, with both adaptive and detrimental effects. While acute stress responses are essential for survival, chronic stress can disrupt multiple physiological systems and compromise health.
Homeostasis—the maintenance of a stable internal environment—is a universal requirement for survival in animals. However, the mechanisms used to achieve this balance vary significantly across species. These differences reflect evolutionary adaptations to diverse environments, diets, and physiological demands. For veterinary students, understanding species-specific variations in homeostasis is essential for accurate diagnosis, treatment, and animal management.
Animals differ markedly in how they regulate body temperature. Most mammals are endothermic and maintain a relatively constant body temperature, but the mechanisms of heat loss vary. For example, dogs rely heavily on panting, whereas horses and humans use sweating as a primary cooling mechanism.
Some species are adapted to extreme environments. Desert animals such as camels can tolerate significant fluctuations in body temperature and conserve water efficiently, while Arctic species possess thick insulation and countercurrent heat exchange systems to minimize heat loss. In contrast, birds have higher baseline body temperatures and unique respiratory adaptations that support high metabolic rates.
Species differences in water metabolism are particularly evident in animals living in arid versus aquatic environments. Desert-adapted animals conserve water through highly efficient kidneys that produce concentrated urine and dry feces. Conversely, aquatic animals face challenges in maintaining electrolyte balance due to constant exposure to water, requiring specialized osmoregulatory mechanisms.
Ruminants also exhibit unique fluid dynamics due to the large volume of fluid within the rumen, which plays a role in digestion and nutrient absorption.
Energy metabolism varies widely among species, particularly between monogastric animals and ruminants. In monogastrics (e.g., dogs and pigs), glucose is primarily derived directly from dietary carbohydrates. In contrast, ruminants rely heavily on microbial fermentation in the rumen, producing volatile fatty acids (VFAs) as their main energy source. As a result, blood glucose levels in ruminants are maintained largely through gluconeogenesis rather than direct absorption.
These differences influence how diseases such as ketosis or metabolic disorders present and are managed in different species.
There are also notable species differences in respiratory physiology. Mammals use a bidirectional (tidal) breathing system, whereas birds have a highly efficient unidirectional airflow system supported by air sacs. This allows for continuous oxygen exchange and supports the high metabolic demands of flight.

Aquatic animals such as fish utilize gills for gas exchange, extracting dissolved oxygen from water. These adaptations illustrate how different species maintain oxygen and carbon dioxide balance in varying environments.
Although the basic principles of acid–base balance are consistent across species, the relative importance of respiratory versus renal mechanisms can vary. For example, animals adapted to high altitudes may exhibit enhanced respiratory efficiency to compensate for lower oxygen availability, influencing acid–base dynamics.
Homeostatic mechanisms are broadly conserved across animals, but the specific strategies used to maintain internal balance vary according to species, environment, and physiology. These differences are critical for veterinary practitioners to understand, as they influence both normal function and disease processes. A strong appreciation of species-specific homeostasis enables more accurate clinical assessment and effective animal care.
Cellular physiology is the study of how cells function, interact, and maintain life. It forms the foundation of all biological processes because the cell is the basic structural and functional unit of life. In veterinary medicine, understanding cellular physiology is essential for interpreting how diseases develop, how tissues respond to injury, and how treatments exert their effects.
Every organ system, whether cardiovascular, digestive, or nervous, depends on the proper functioning of its individual cells. When cellular processes are disrupted, this dysfunction can manifest as clinical disease. Thus, cellular physiology provides the critical link between molecular biology and whole-animal medicine.
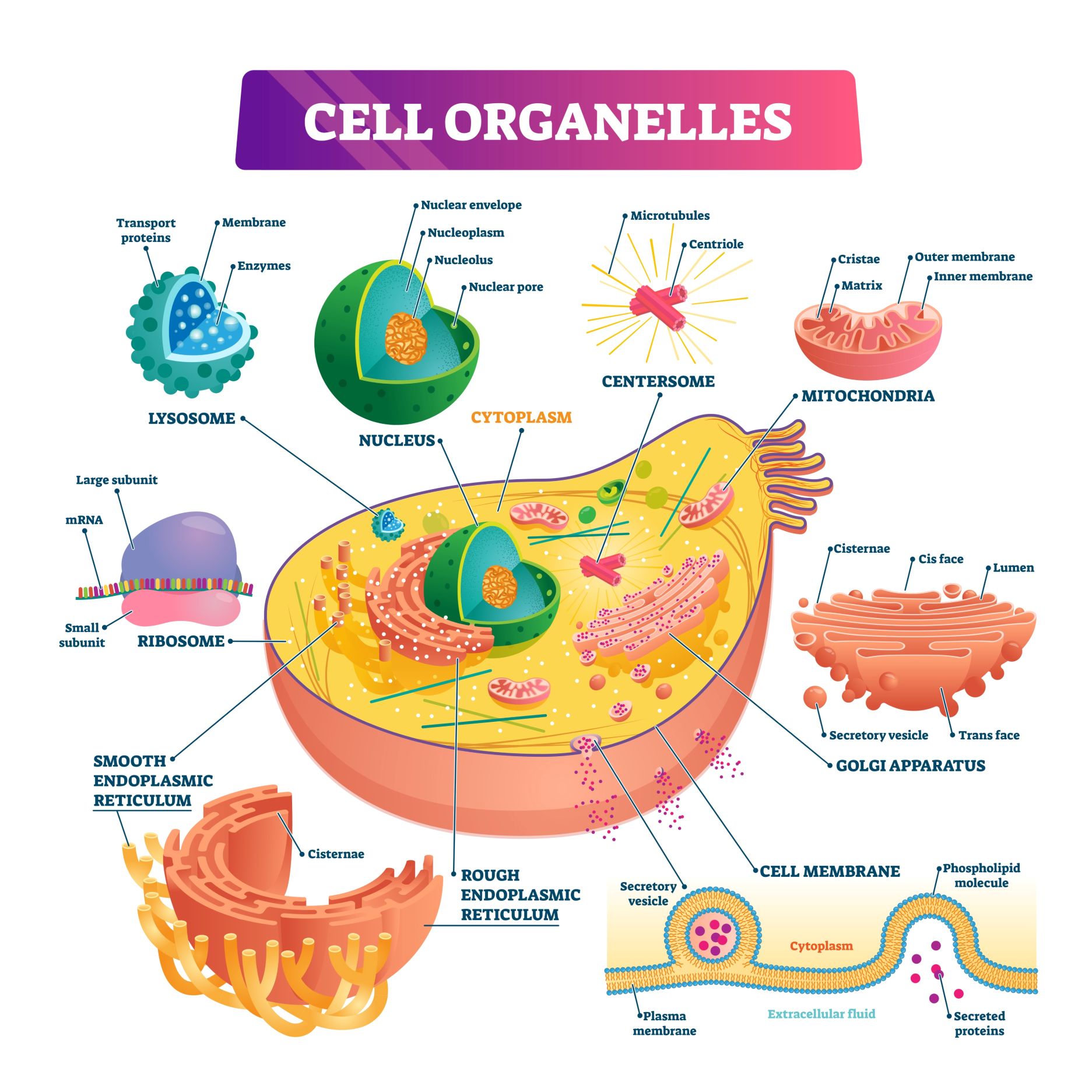
Animal cells are highly organized structures composed of specialized components known as organelles. Each organelle performs specific functions necessary for cell survival.
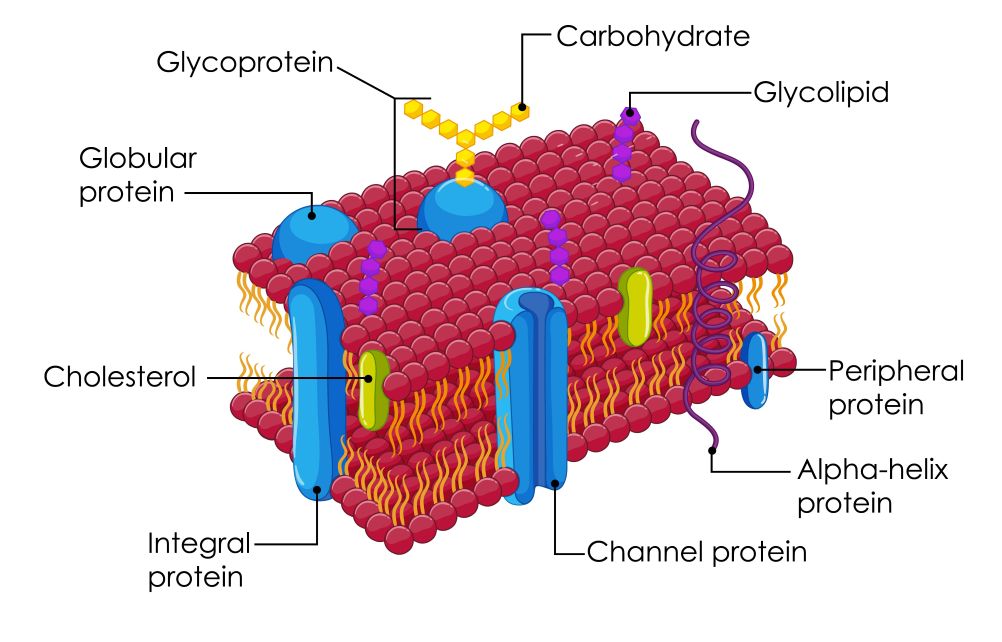
The cell membrane (plasma membrane) is a dynamic, selectively permeable barrier that separates the internal environment of the cell from the extracellular space. It is composed primarily of a phospholipid bilayer with embedded proteins, cholesterol, and carbohydrates. This structure allows the membrane to regulate the movement of substances in and out of the cell while also facilitating communication with other cells.
Within the cell, the cytoplasm contains various organelles suspended in a fluid matrix known as cytosol. Key organelles include:
The coordinated function of these structures ensures that the cell can carry out metabolism, growth, and repair.
The plasma membrane is central to cellular physiology because it controls the internal environment of the cell. A key concept is selective permeability, meaning the membrane allows some substances to pass while restricting others. This property is essential for maintaining appropriate concentrations of ions, nutrients, and waste products.
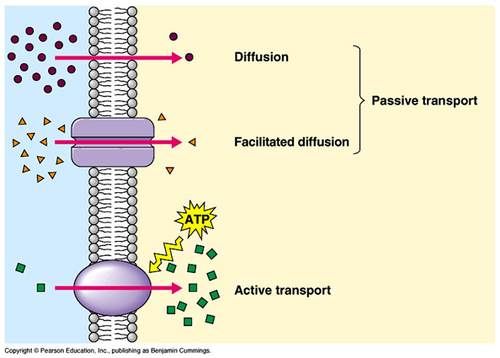
Substances cross the membrane through several mechanisms:
This process does not require energy and occurs along a concentration gradient.
Requires energy (ATP) to move substances against their concentration gradient.
Example: Na⁺/K⁺ ATPase pump, which maintains cellular ion gradients.
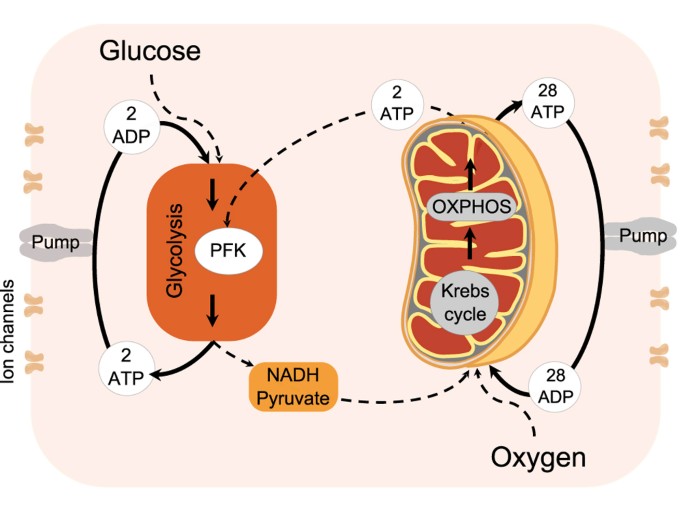
Cells require energy to perform essential functions such as transport, synthesis, and movement. This energy is stored and utilized in the form of ATP (adenosine triphosphate).
Energy production occurs primarily in the mitochondria through:
Oxygen plays a critical role in efficient ATP production. In conditions of hypoxia, cells switch to anaerobic metabolism, resulting in reduced ATP production and accumulation of lactic acid.
In veterinary medicine, impaired cellular metabolism is seen in conditions such as:
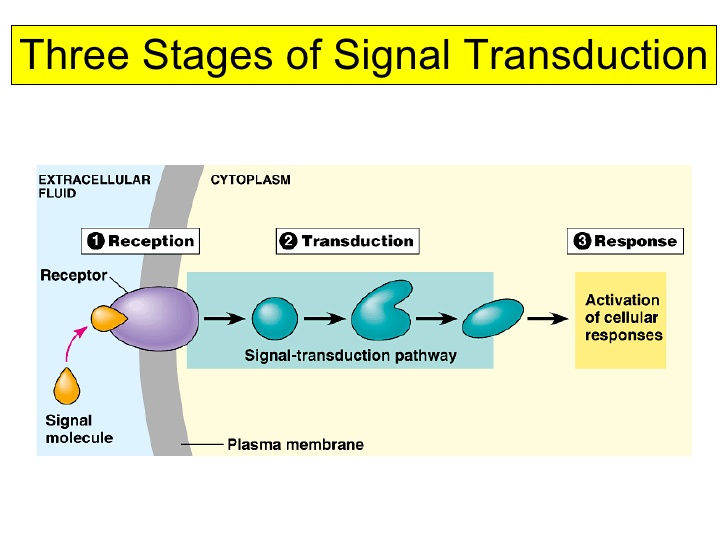
Cells must communicate to coordinate functions within tissues and organ systems. This communication occurs through chemical signals such as hormones, neurotransmitters, and cytokines.
Cell signaling typically involves:
There are different types of signaling:
Disruptions in signaling pathways can lead to diseases such as cancer, endocrine disorders, and immune dysfunction.
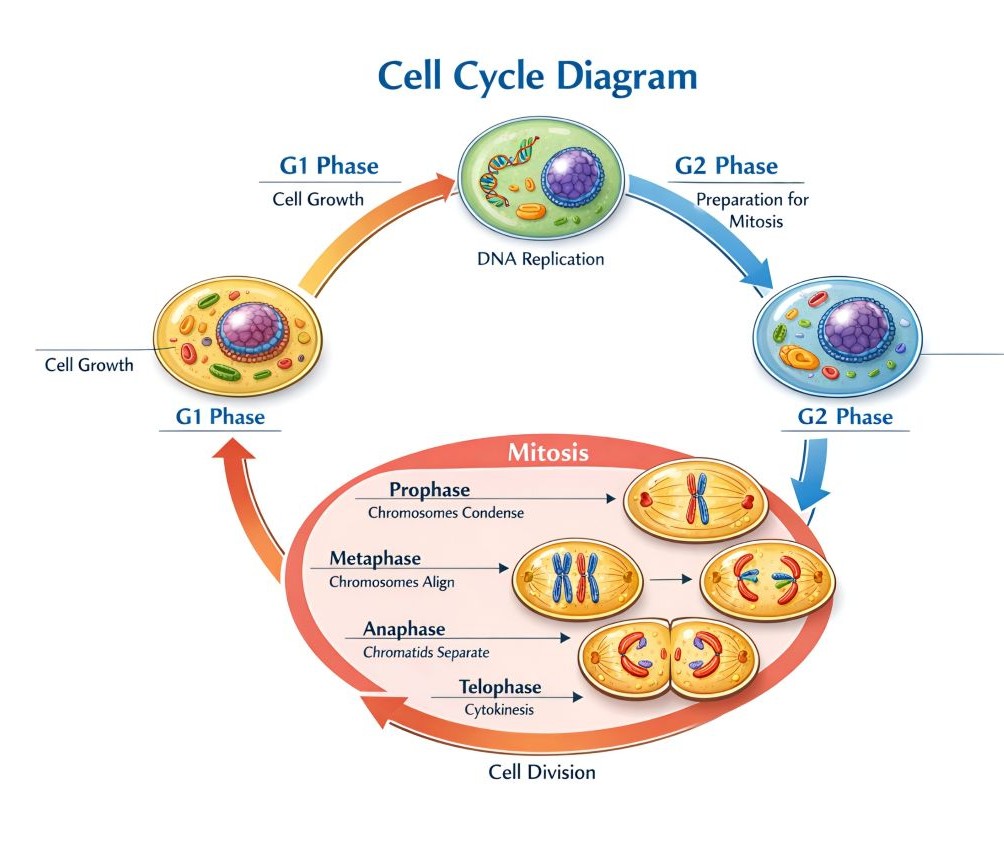
Cells reproduce through the cell cycle, which includes:
Controlled cell division is essential for:
Loss of control over the cell cycle can result in neoplasia (cancer), while inadequate cell division can impair healing.
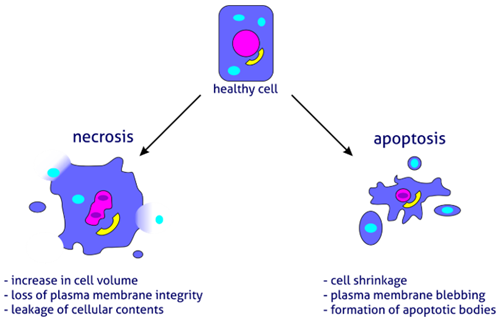
Cell death is a normal and necessary process but can also occur pathologically.
In veterinary medicine:
Cells respond to stress through adaptive changes:
These adaptations allow cells to survive adverse conditions, but prolonged stress can lead to injury and disease.

When stress exceeds the cell's ability to adapt, cell injury occurs.
Cellular physiology provides the fundamental framework for understanding how animals function in both health and disease. By examining processes such as membrane transport, energy metabolism, cell signaling, and cell death, veterinary students gain insight into the mechanisms that underlie clinical conditions. A solid grasp of cellular physiology enables veterinarians to move beyond symptom recognition and toward a deeper understanding of disease processes, ultimately improving diagnosis, treatment, and animal care.
The cardiovascular system is responsible for the transport of oxygen, nutrients, hormones, and metabolic waste products throughout the body. It plays a central role in maintaining internal stability and supporting the function of all other organ systems. In veterinary medicine, a solid understanding of cardiovascular physiology is essential for recognizing disease processes, interpreting clinical signs, and implementing effective treatment strategies.
At its core, the cardiovascular system consists of the heart, blood vessels, and blood. Together, these components ensure that tissues receive adequate oxygen and nutrients while facilitating the removal of carbon dioxide and other waste products. The system also contributes to thermoregulation, immune defense, and acid–base balance.
The heart is a muscular organ that functions as a pump, driving blood through two distinct circuits:
The heart consists of four chambers:
Blood flow is unidirectional due to the presence of valves:
These valves prevent backflow and ensure efficient circulation.

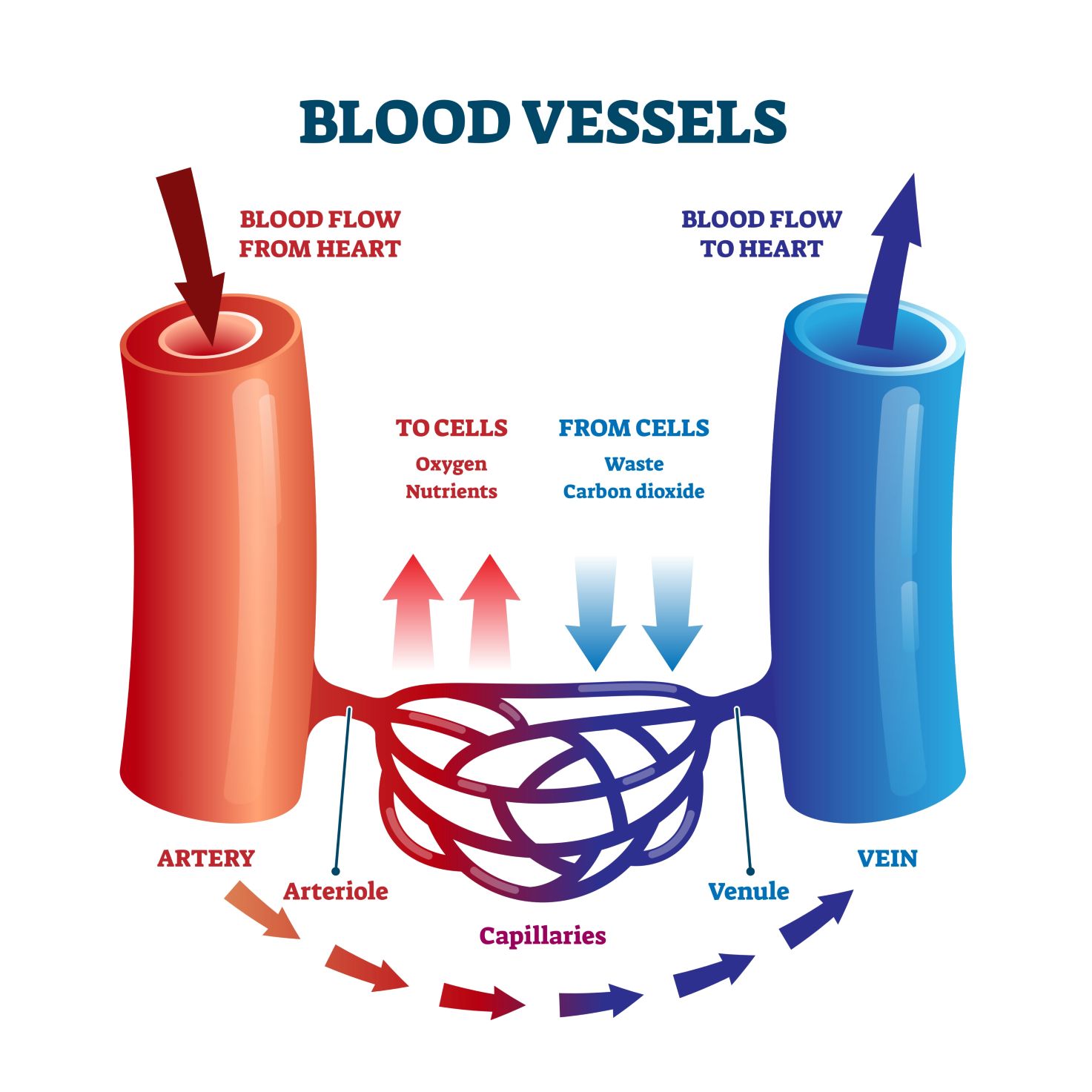
Blood vessels form a continuous network that transports blood:
The structure of each vessel type is adapted to its function, with arteries having thicker muscular walls and veins containing valves to prevent backflow.
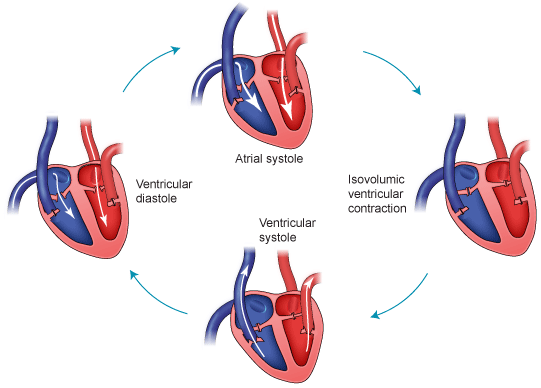
The cardiac cycle refers to the sequence of events that occur during one heartbeat and consists of:
Coordinated contraction ensures efficient blood flow.
The heart has an intrinsic conduction system that allows it to beat rhythmically without external stimulation.
Key components include:
Electrical impulses originate in the SA node and spread through the heart, resulting in coordinated contraction.
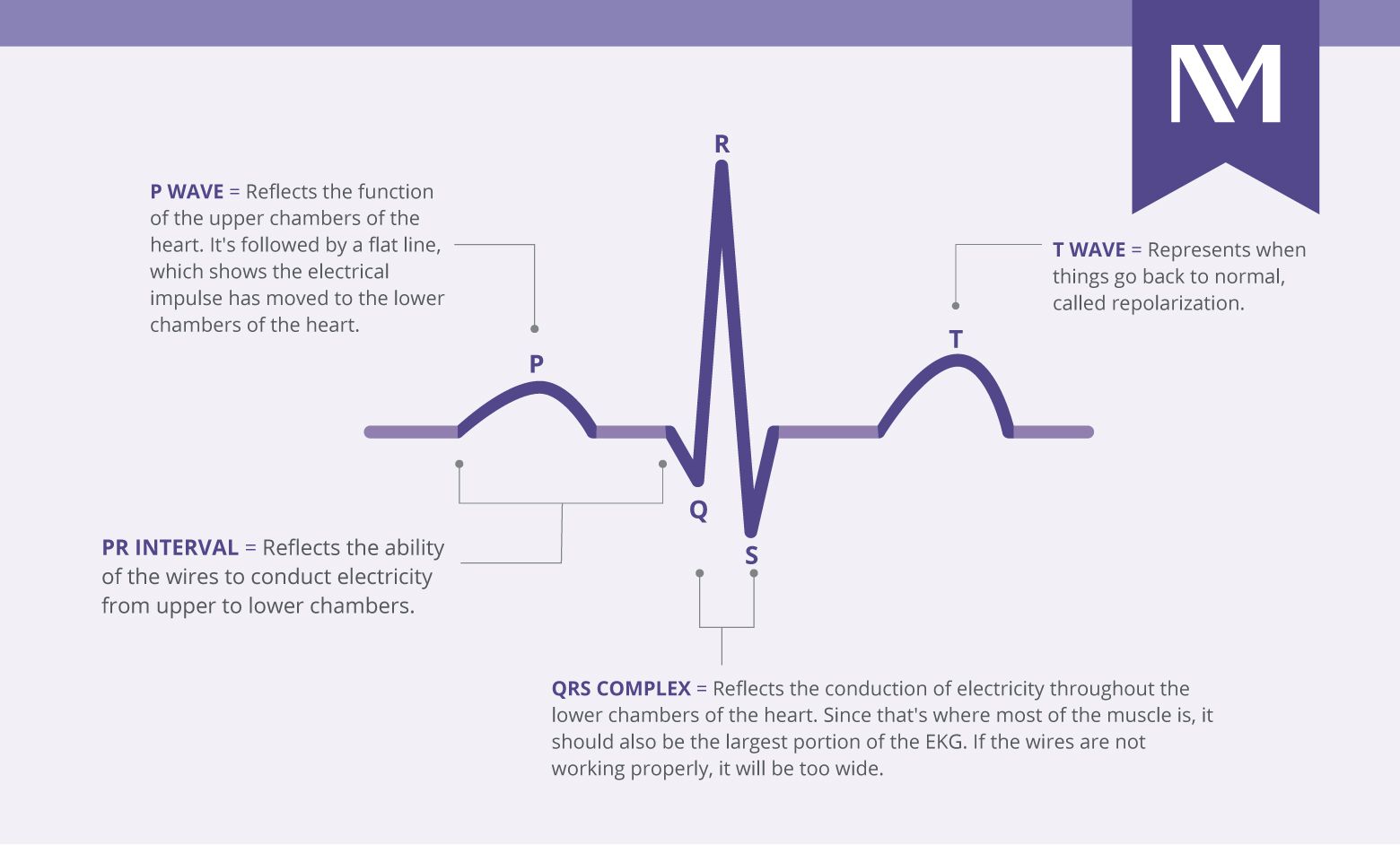
An electrocardiogram (ECG or EKG) is a non-invasive medical test that records the electrical activity of your heart over a period of time. It captures the tiny electrical impulses that trigger your heart muscle to contract and pump blood, displaying them as a line graph of "waves".
Key Components of the ECG Wave
A standard heartbeat on an ECG consists of three main parts, each representing a specific stage of the heart’s electrical cycle:
Cardiac output (CO) is the volume of blood pumped by the heart per minute:
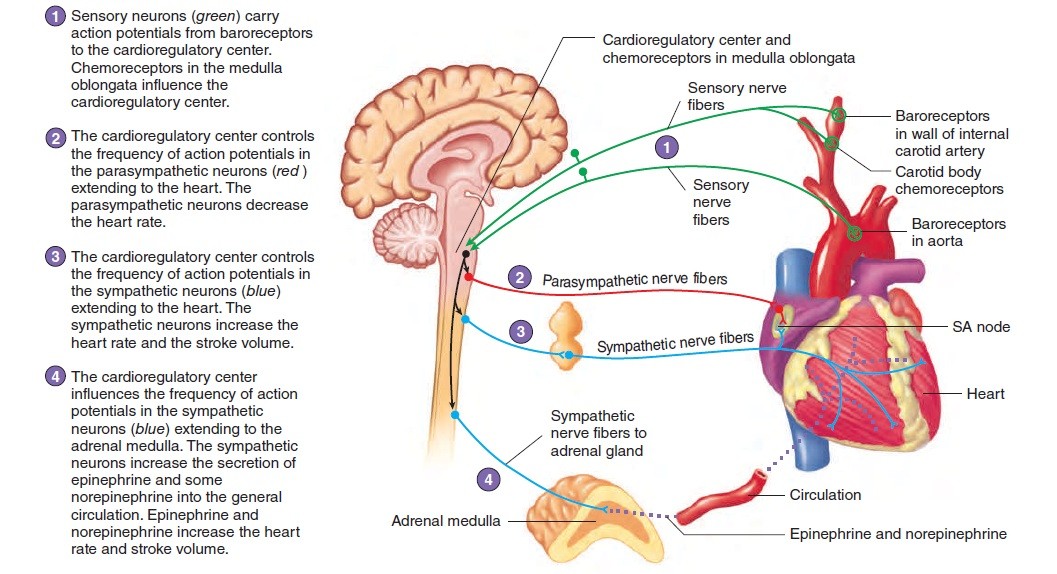
Cardiac activity is tightly regulated by:
Blood flow is governed by basic physical principles:
Arterioles play a major role in regulating peripheral resistance and, therefore, blood pressure.
Blood pressure is maintained through short- and long-term mechanisms:

Capillaries are the sites of exchange between blood and tissues. Substances move across capillary walls by:
Proper balance between these forces ensures adequate tissue perfusion and prevents edema.
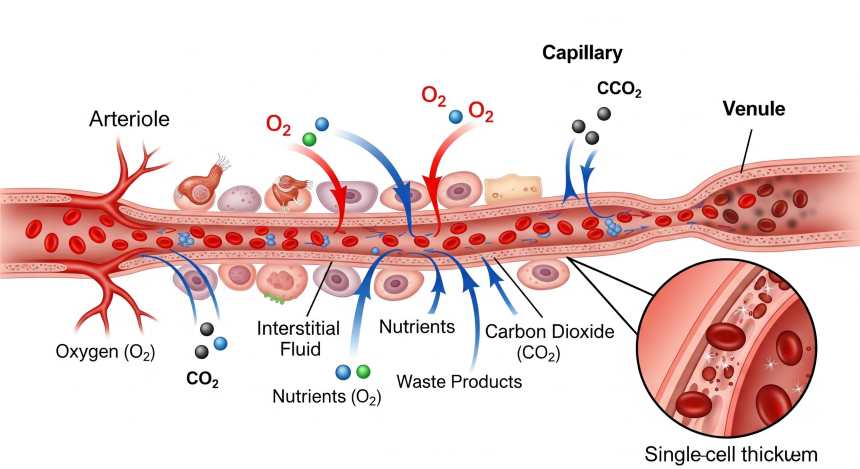
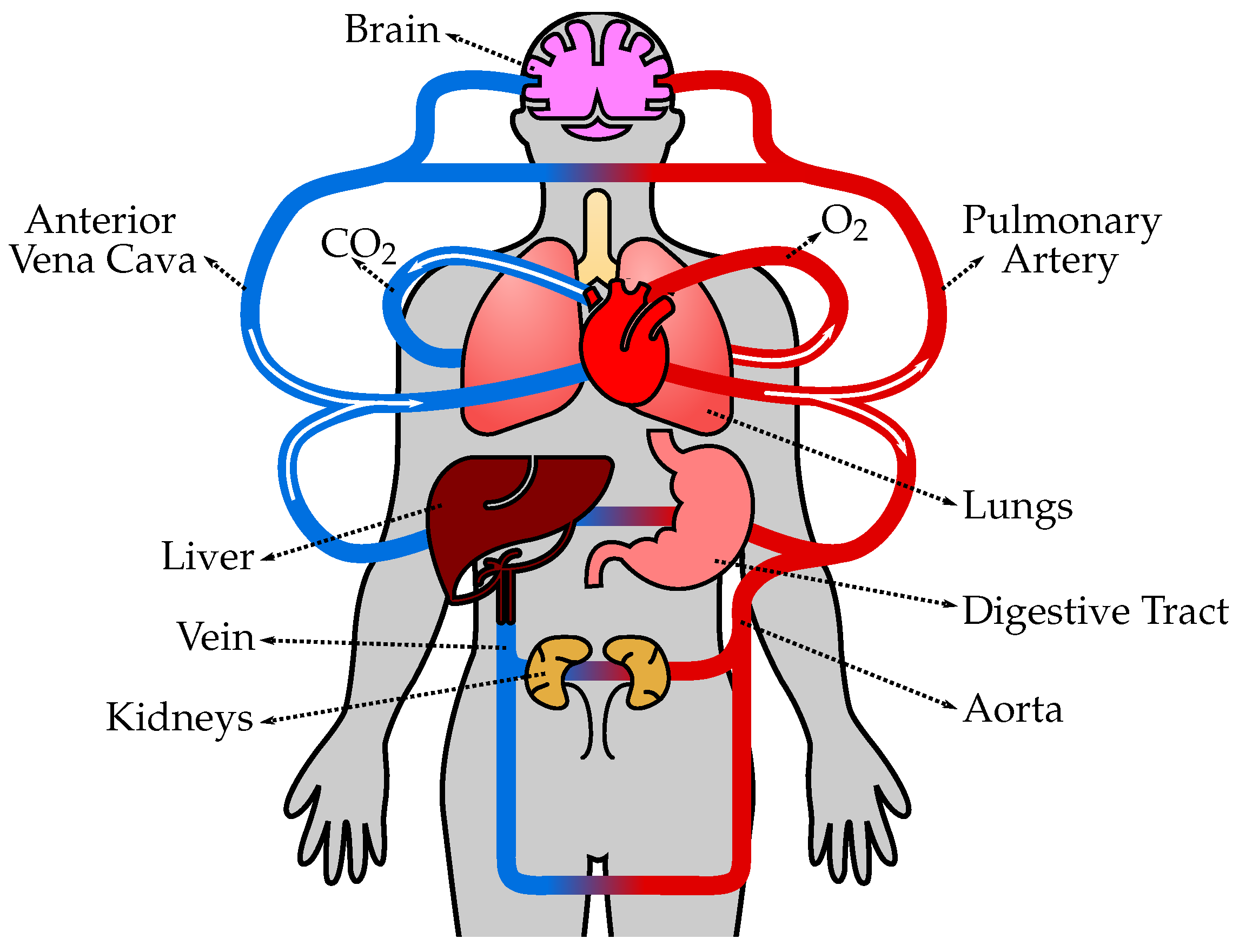
The cardiovascular system works closely with:
This integration is essential for maintaining overall physiological balance.
Different animal species exhibit variations in cardiovascular function. Smaller species generally have faster heart rates. Key differences include ventricular depolarization patterns (Category A vs. B), coronary collateral circulation, and heart shape (e.g., blunter apex in dogs vs. conical in sheep):
Comparative Models:
These differences influence disease presentation and treatment strategies.
Sheep heart
Canine heart
During exercise:
Training improves cardiovascular efficiency, particularly in athletic animals such as horses.
When normal cardiovascular function is disrupted, disease occurs.
Occurs when the heart cannot meet the body's demands.
A life-threatening condition characterized by inadequate tissue perfusion.
Types include:
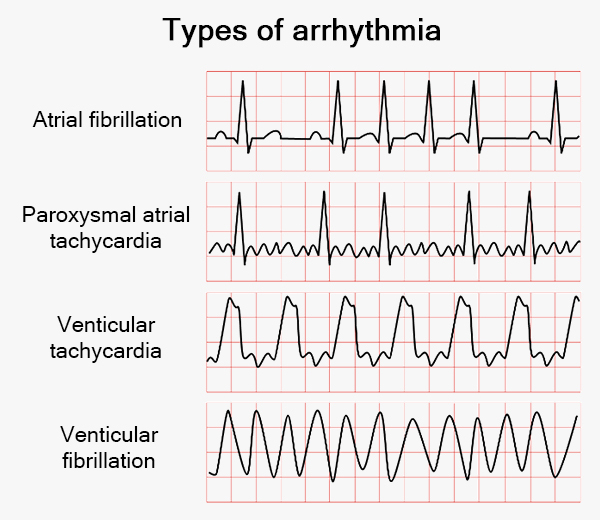
An arrhythmia is an abnormal heart rhythm, where the heart beats too fast (tachycardia), too slow (bradycardia), or irregularly. Caused by faulty electrical signals, it often feels like a fluttering or skipping beat, accompanied by dizziness or chest pain. It is diagnosed via ECG, Holter monitor, or echocardiogram. Risk factors that increase the risk include aging, underlying heart disease, high blood pressure, and excessive stress.
Hypertension, or high blood pressure, is a chronic condition where blood force against artery walls is consistently too high, often causing no symptoms until serious damage occurs (the "silent killer"). It is managed through lifestyle changes—like reducing sodium and increasing exercise—and medication to prevent heart attack, stroke, and kidney damage.
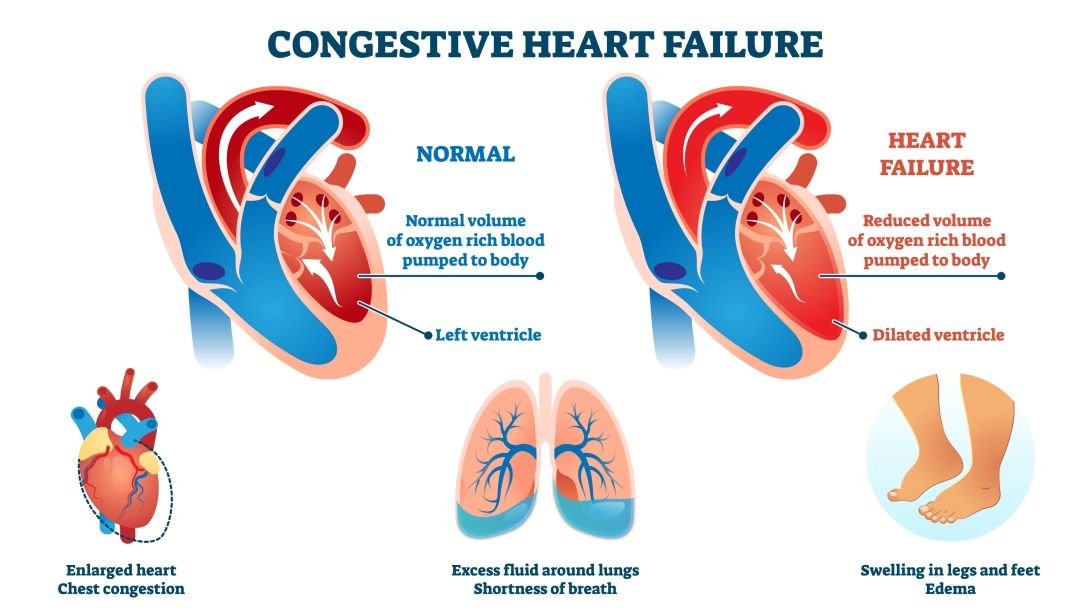
Accumulation of fluid in tissues due to imbalances in capillary pressures.
The cardiovascular system is central to maintaining life by ensuring effective circulation of blood and maintaining tissue perfusion. Its function depends on the coordinated activity of the heart, blood vessels, and regulatory systems. A strong understanding of cardiovascular physiology allows veterinary professionals to interpret clinical signs, understand disease mechanisms, and apply appropriate treatments. It serves as a critical bridge between basic science and clinical practice.

The respiratory system is responsible for the exchange of gases between the body and the external environment, ensuring adequate oxygen supply for cellular metabolism and removal of carbon dioxide, a metabolic waste product. In veterinary medicine, a thorough understanding of respiratory physiology is essential for diagnosing and managing diseases that impair breathing, oxygenation, and acid–base balance. Beyond gas exchange, the respiratory system also contributes to thermoregulation, acid–base homeostasis, vocalization, and defense against inhaled pathogens. Its function is closely integrated with the cardiovascular and nervous systems, forming a coordinated network that maintains internal stability under varying physiological and environmental conditions.
The respiratory system can be divided into two main components:
These structures are responsible for filtering, warming, and humidifying inhaled air.
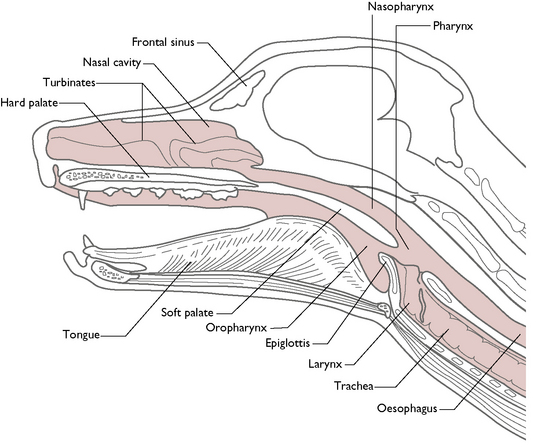
The lower tract conducts air to the lungs and facilitates gas exchange.
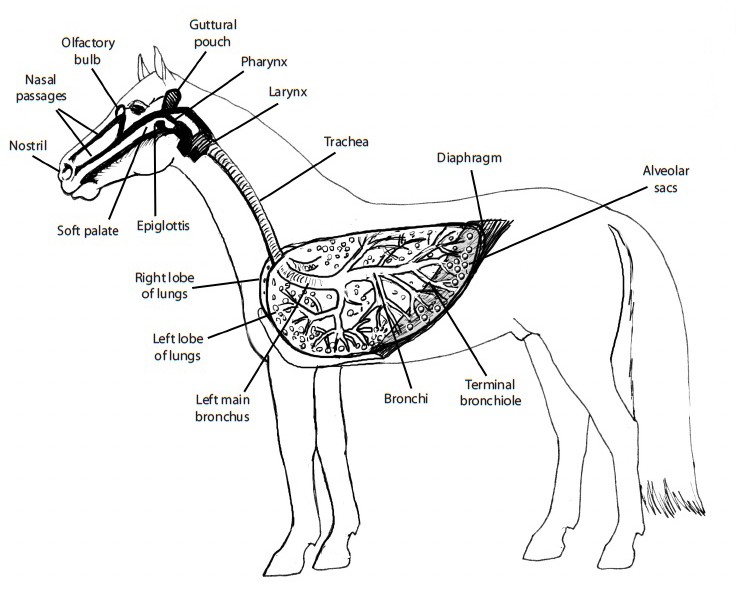
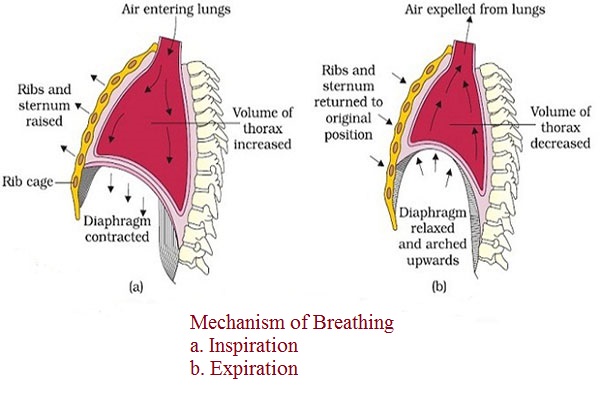
Breathing, or ventilation, involves the movement of air into and out of the lungs.
The process of breathing relies on pressure gradients and the elasticity of lung tissue.
Gas exchange occurs in the alveoli, which are small air sacs with thin walls and a rich blood supply.
The key process is Diffusion, where gases move from areas of higher concentration to lower concentration:
Efficient gas exchange depends on:
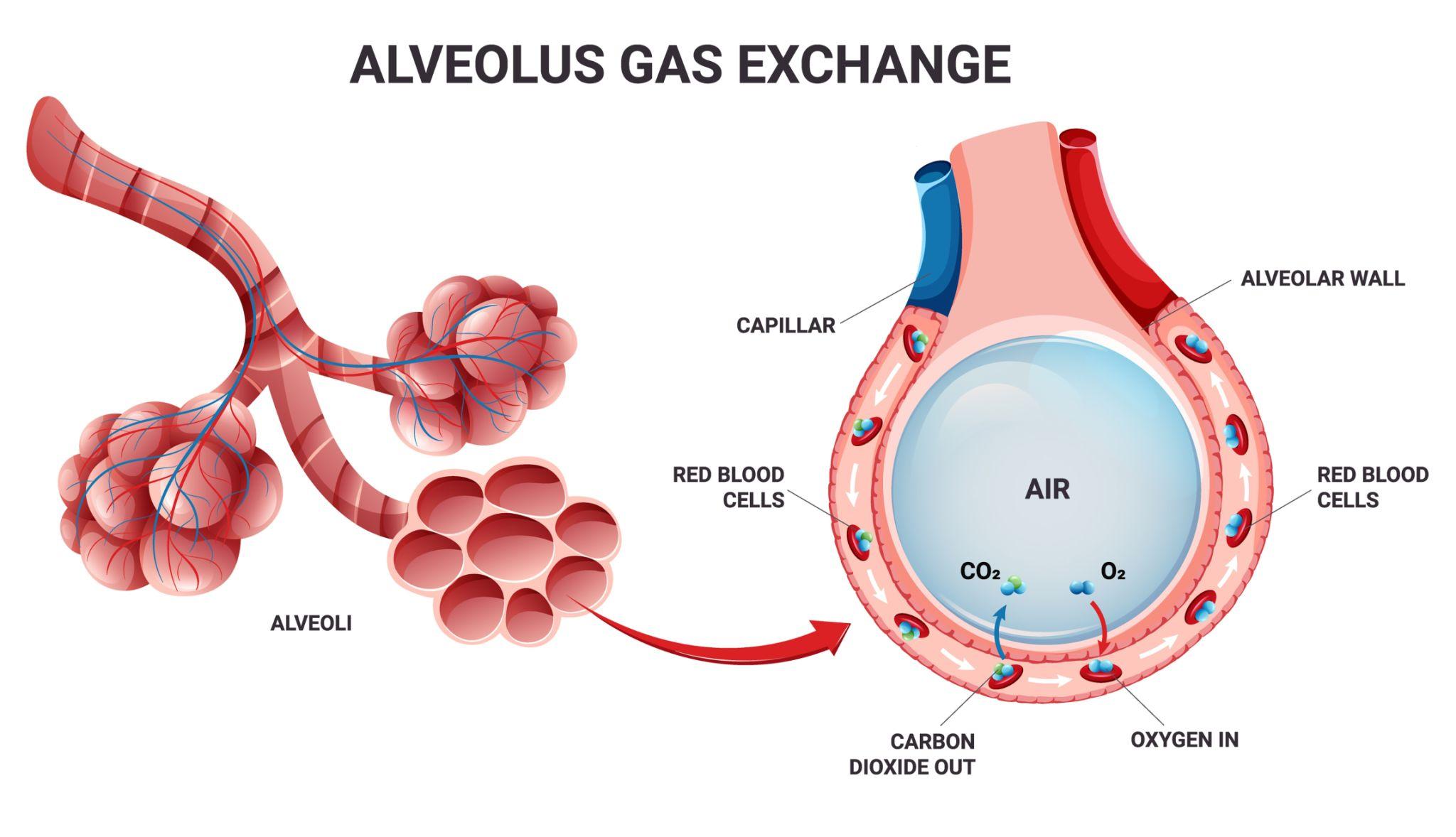
The balance between oxygen delivery and carbon dioxide removal is critical for maintaining cellular function.
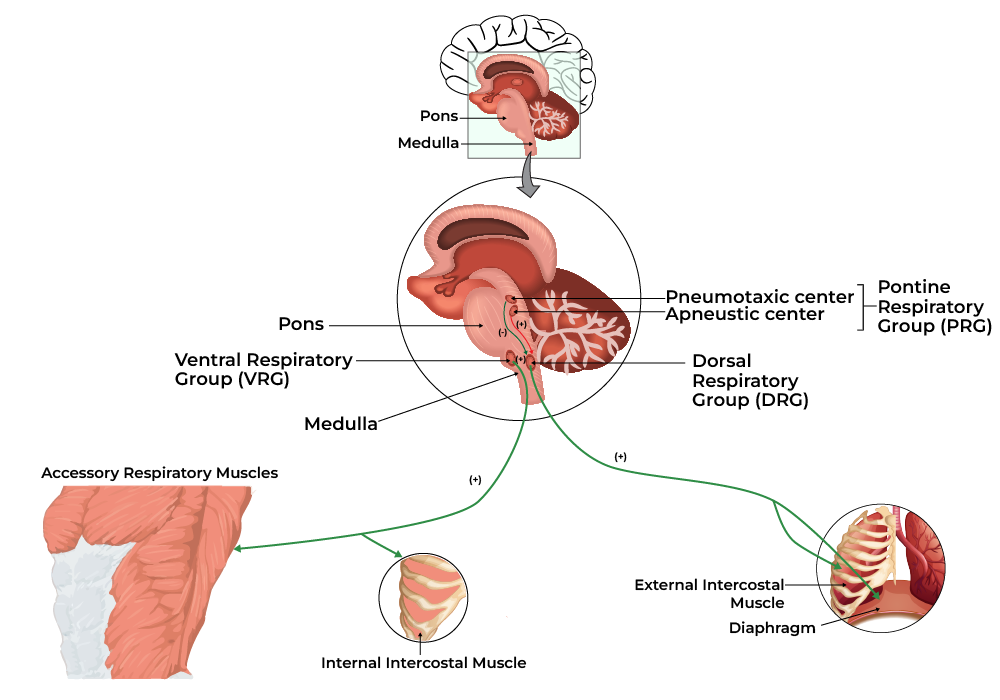
Respiration is controlled by neural and chemical mechanisms.
An increase in carbon dioxide or a decrease in pH stimulates increased ventilation.
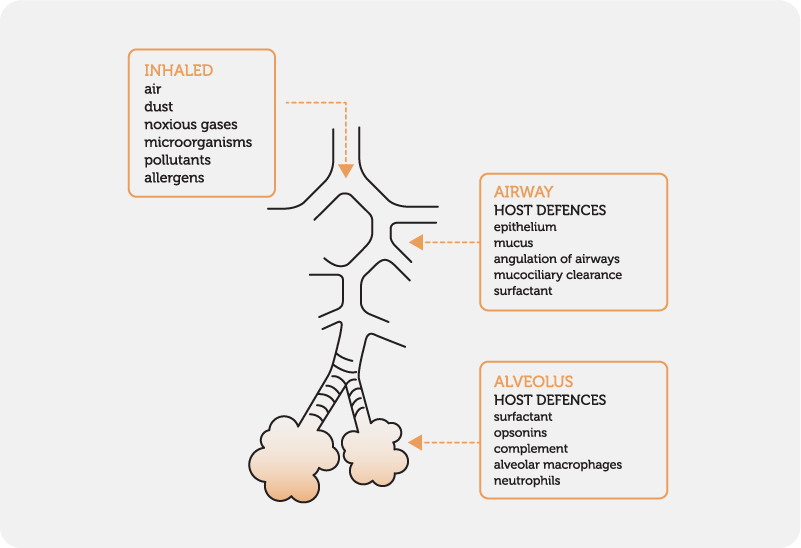
The respiratory system has several protective mechanisms:
These defenses help prevent infection and maintain airway integrity.
The respiratory system works closely with:
The respiratory system plays a major role in maintaining blood pH by regulating carbon dioxide levels.
This interaction between the respiratory and renal systems is essential for maintaining homeostasis.
Different animal species exhibit unique respiratory adaptations:
These differences influence disease susceptibility and clinical management.
During exercise:
In athletic animals, such as horses, the respiratory system is highly adapted to meet increased metabolic demands.
Respiratory diseases interfere with ventilation, gas exchange, or both.
The respiratory system is vital for maintaining life by ensuring efficient gas exchange and supporting acid–base balance. Its function depends on coordinated ventilation, diffusion, and perfusion processes. For veterinary professionals, a strong understanding of respiratory physiology is essential for diagnosing disease, managing clinical cases, and supporting animal health across species.

The digestive system is responsible for the ingestion, breakdown, absorption, and elimination of food. It plays a critical role in maintaining energy balance, supporting growth and production, and sustaining overall health in animals. In veterinary medicine, understanding digestive physiology is essential for diagnosing gastrointestinal diseases, formulating appropriate diets, and managing metabolic disorders. The digestive system is not merely a conduit for food passage; it is a complex, highly regulated system involving mechanical processes, enzymatic digestion, microbial fermentation, and coordinated motility. Its function is closely integrated with other physiological systems, including the endocrine, nervous, and immune systems.
The digestive system consists of the alimentary canal and accessory organs.
A continuous tube extending from the mouth to the anus, including:
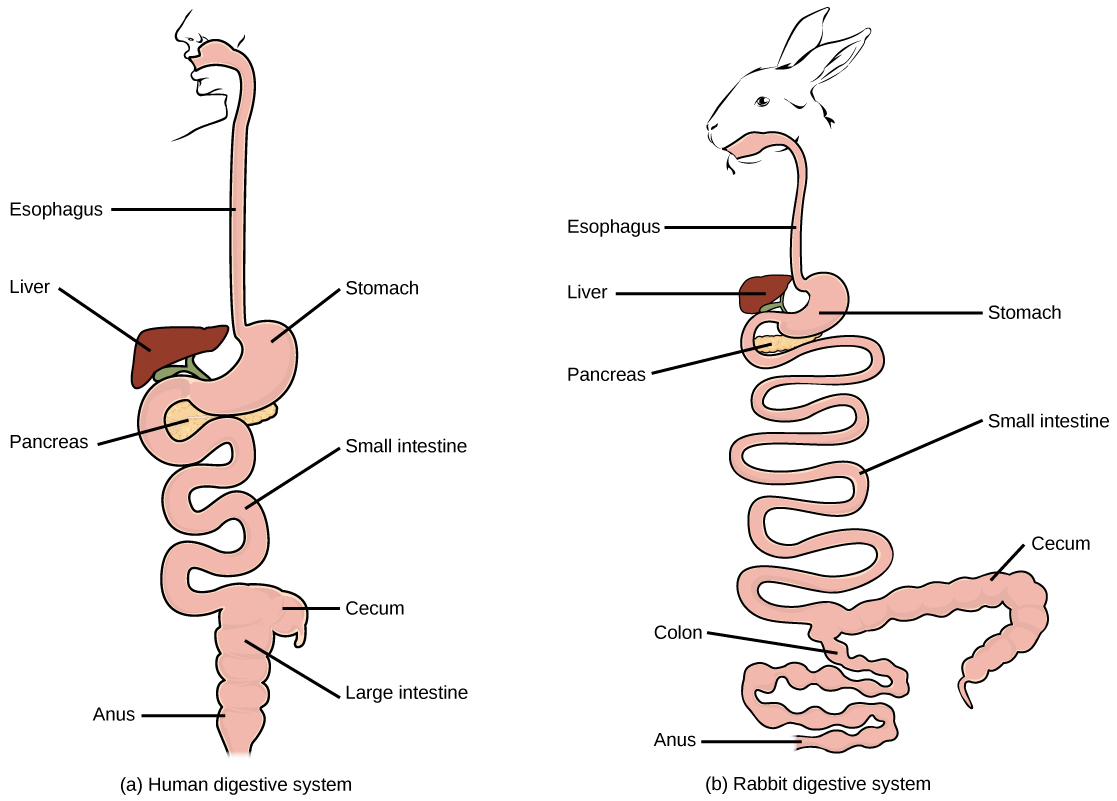
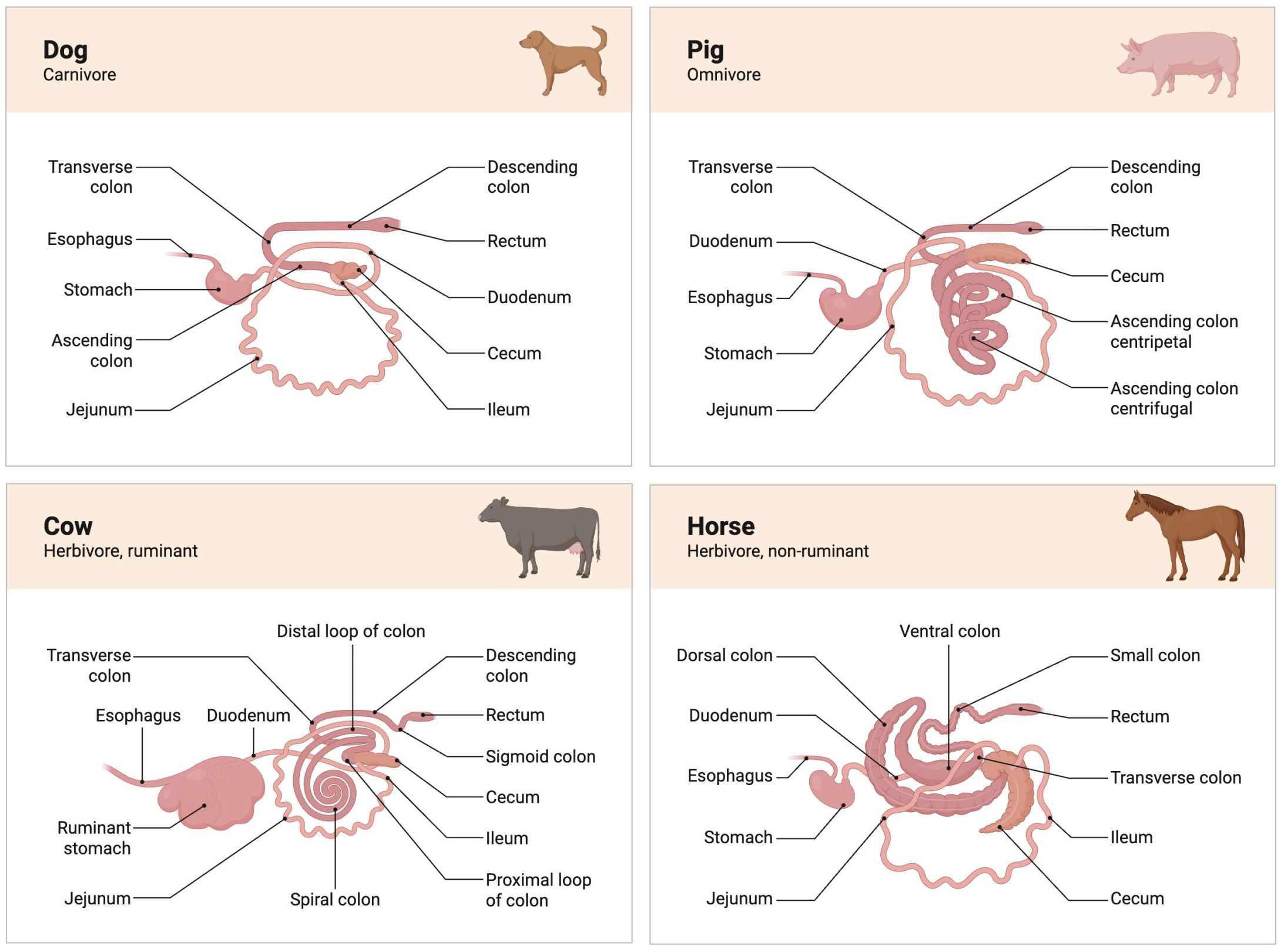
Each component contributes to digestion and absorption through specialized functions.
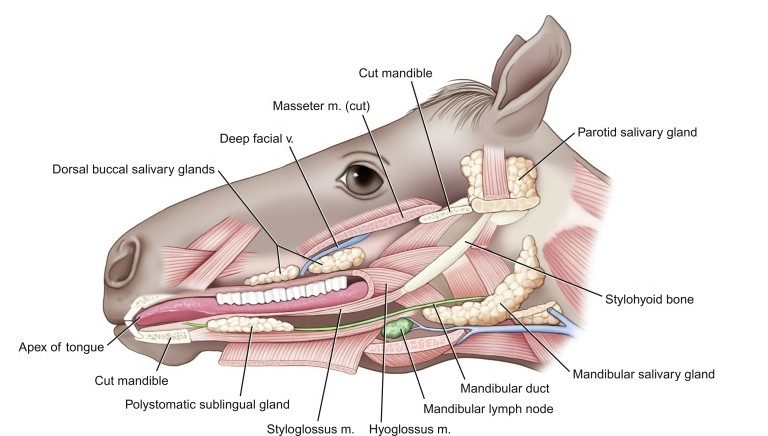
Digestion begins in the oral cavity, where food is ingested and mechanically processed.
Salivary secretion is regulated by the autonomic nervous system and is essential for proper digestion, especially in herbivores.
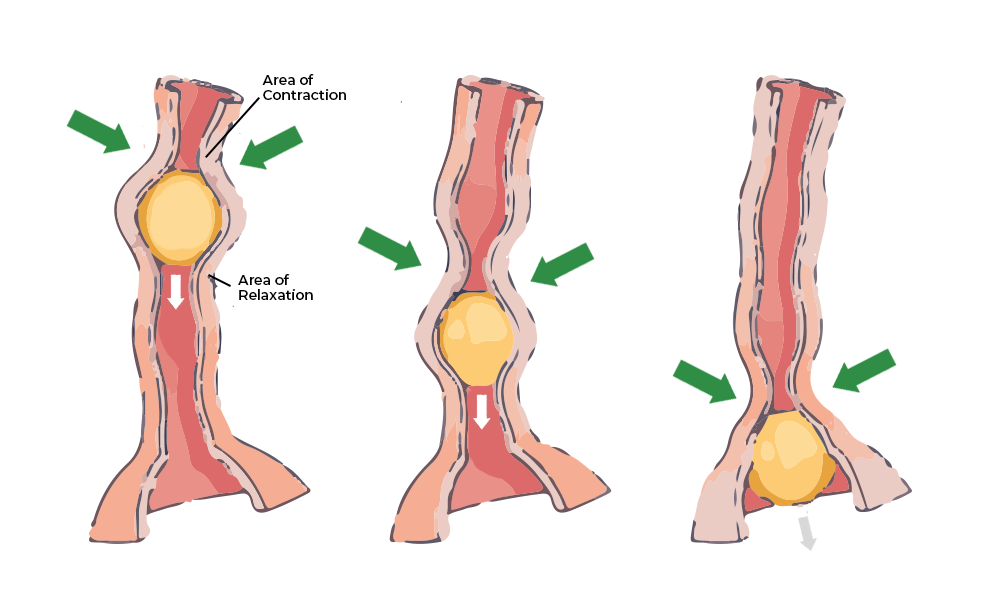
Swallowing is a coordinated reflex involving voluntary and involuntary phases. The esophagus transports food to the stomach via peristalsis, a wave-like contraction of smooth muscle. Dysfunction of this process can lead to conditions such as regurgitation or esophageal obstruction.
The stomach serves as a reservoir and initiates protein digestion.
Gastric motility ensures proper mixing and gradual emptying into the small intestine.

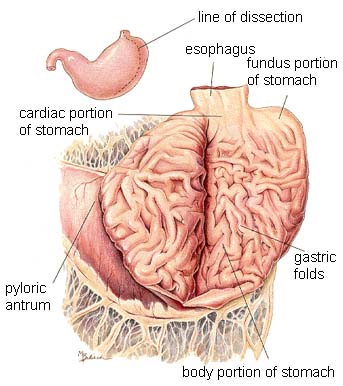
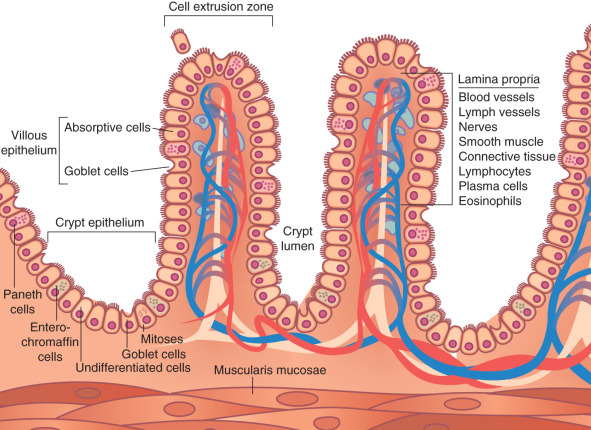
The small intestine is the primary site for digestion and nutrient absorption.
Enzymes from the pancreas and intestinal mucosa break down:
The intestinal lining is specialized with villi and microvilli, increasing surface area.
Nutrients are absorbed via:
Efficient absorption is critical for maintaining energy and nutrient balance.
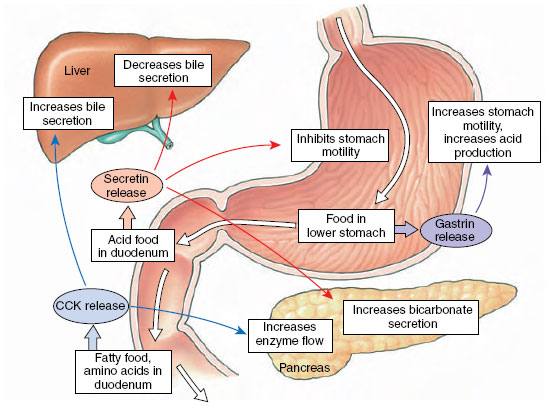
The liver is a central metabolic organ that:
Stores and concentrates bile, releasing it into the small intestine when needed.
Has both exocrine and endocrine functions:

The large intestine is primarily responsible for:
In some species, it also supports microbial fermentation, contributing to digestion of fibrous material.
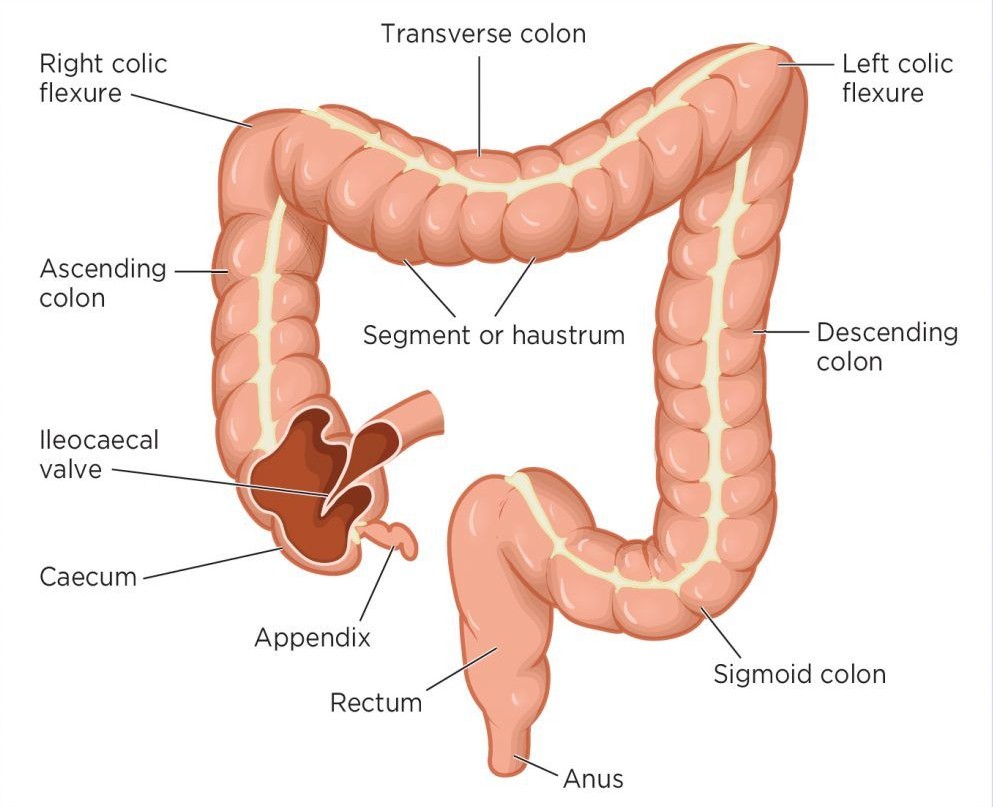
Digestive processes depend on coordinated movement of the gastrointestinal tract, known as motility.
A key mechanism is Peristalsis, which propels contents through the digestive tract.
These systems ensure that digestion is synchronized with nutrient availability.
A defining feature of veterinary digestive physiology is the variation among species.
These differences have major implications for nutrition, disease, and treatment.
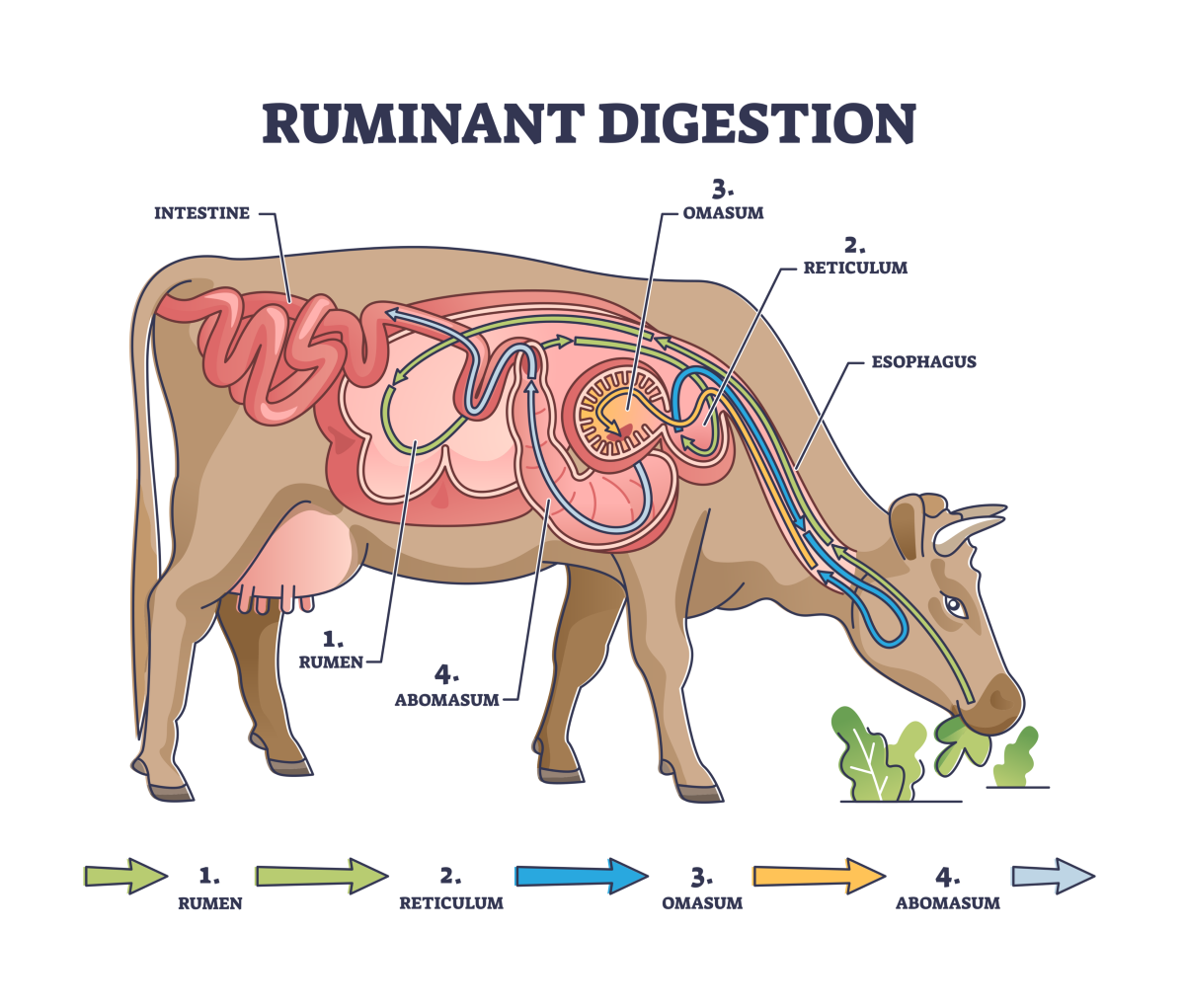
The digestive system interacts with:
Disruption of digestive function can occur at multiple levels:
The digestive system is a complex and highly coordinated system essential for sustaining life. It involves mechanical, chemical, and microbial processes that convert food into usable nutrients while eliminating waste. For veterinary professionals, understanding digestive physiology provides the foundation for recognizing disease, implementing treatment strategies, and optimizing animal health and productivity. Its study highlights the importance of species differences and the integration of multiple physiological systems.
The urinary system plays a fundamental role in maintaining internal balance by regulating fluid volume, electrolyte composition, and waste excretion. It is essential for preserving the stability of the internal environment, making it a key component of Homeostasis. In veterinary medicine, understanding urinary physiology is critical for diagnosing renal disease, managing fluid therapy, and addressing metabolic and electrolyte imbalances. The urinary system not only eliminates metabolic waste products but also contributes significantly to acid–base regulation, blood pressure control, and endocrine functions. Dysfunction of this system can lead to serious, often life-threatening conditions, emphasizing its clinical importance across all animal species.
The urinary system consists of:
Among these, the kidneys are the most complex and functionally significant structures.
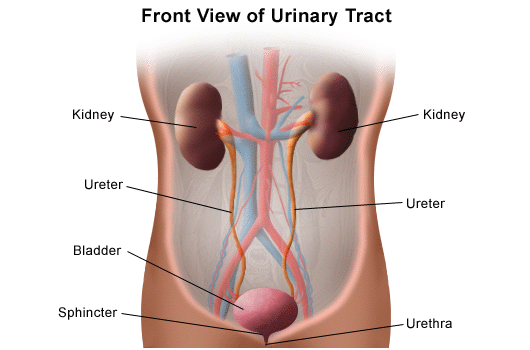
The kidney is composed of two main regions:
The functional unit of the kidney is the nephron, which is responsible for urine formation.

Each segment has specialized roles in filtration, reabsorption, and secretion.
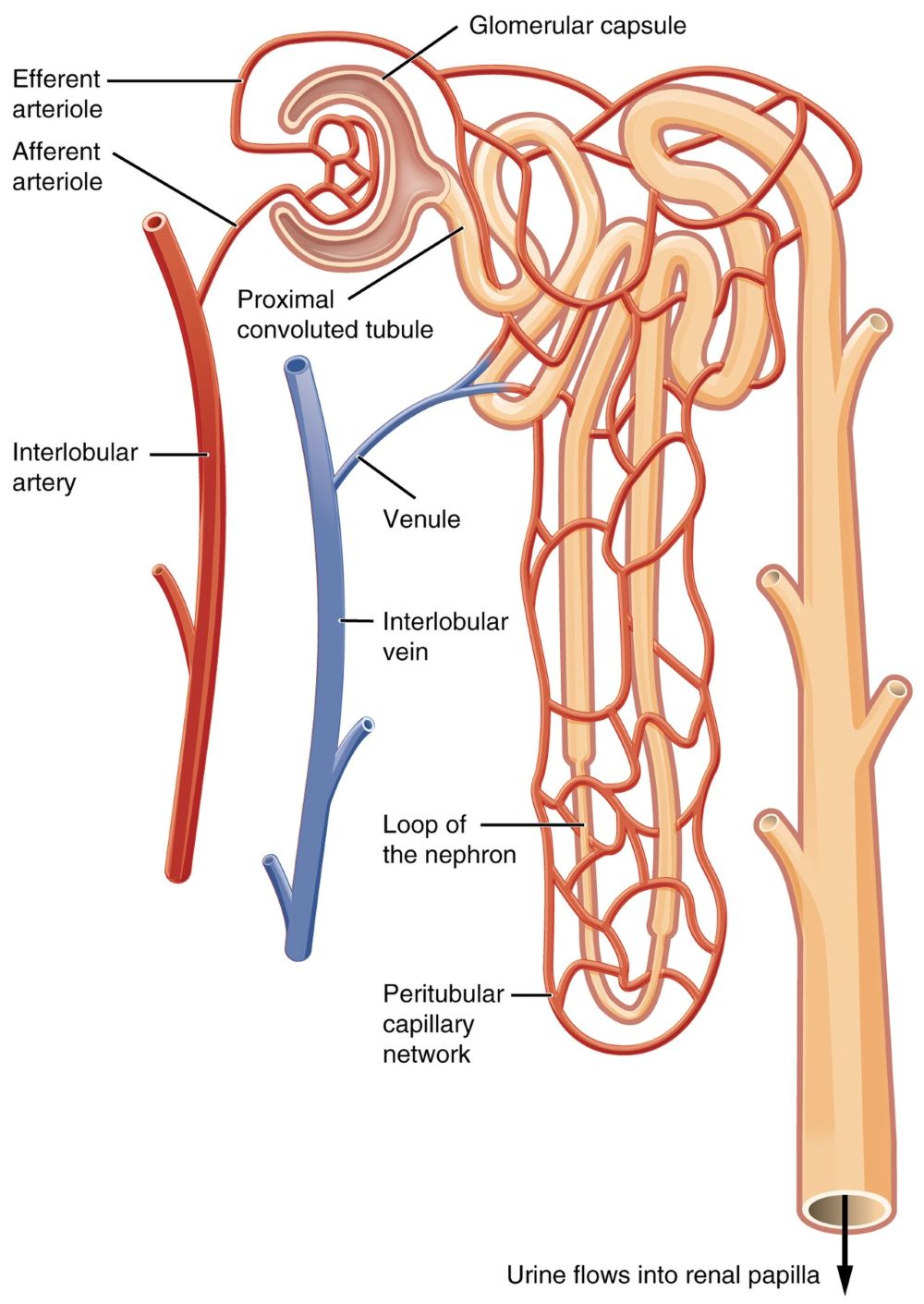
The kidneys receive a significant portion of cardiac output, reflecting their importance in filtration and regulation.
The process by which plasma is filtered from the blood into the nephron is known as Glomerular Filtration.
The rate of filtration, known as the glomerular filtration rate (GFR), is a key indicator of kidney function.
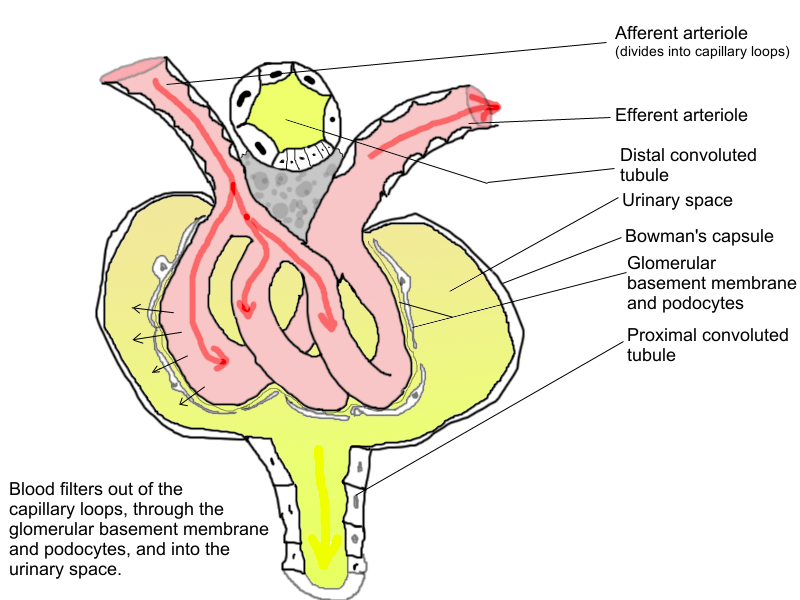
After filtration, the filtrate undergoes extensive modification as it passes through the nephron.
These processes ensure that essential substances are conserved while waste products are excreted.
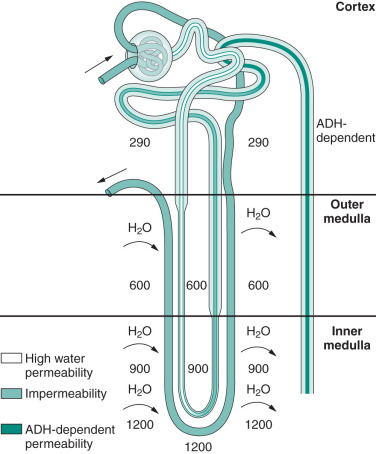
The kidney regulates water balance by adjusting urine concentration.
A key mechanism is the countercurrent system in the loop of Henle, which establishes a concentration gradient in the medulla.
This ability is critical for survival, especially in animals exposed to varying water availability.
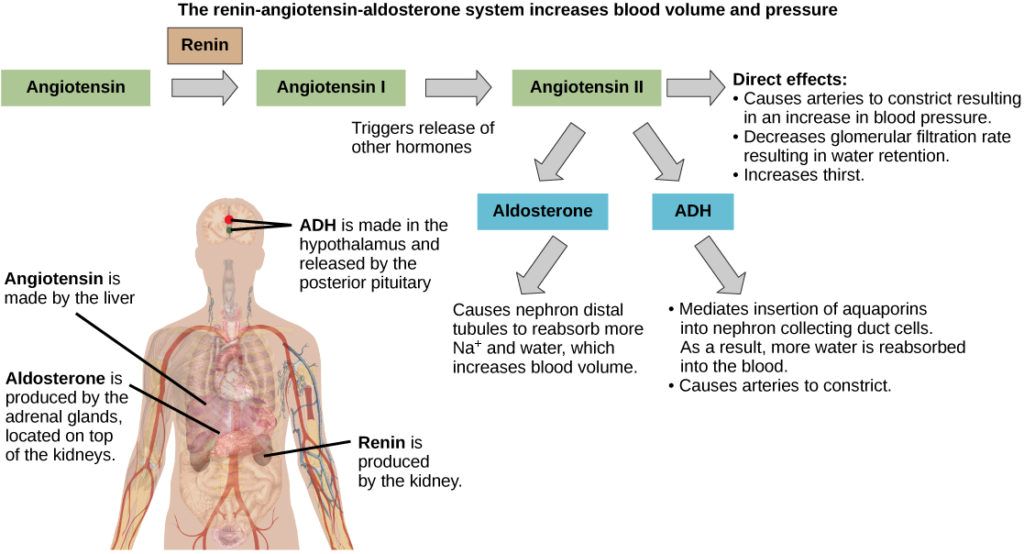
The kidneys maintain proper levels of:
This regulation ensures stable blood volume and pressure.
The urinary system plays a crucial role in maintaining blood pH.
Mechanisms include:
These processes work alongside the respiratory system to maintain acid–base homeostasis.
The urinary system interacts with:
Urine formation involves three main processes:
The final urine contains:
Urine is transported via the ureters to the bladder, stored, and eventually expelled through the urethra.
Urination is controlled by a combination of voluntary and involuntary mechanisms.
Disruption of these mechanisms can lead to urinary retention or incontinence.
Different animals exhibit adaptations in renal function:
These differences are important in diagnosis and treatment.
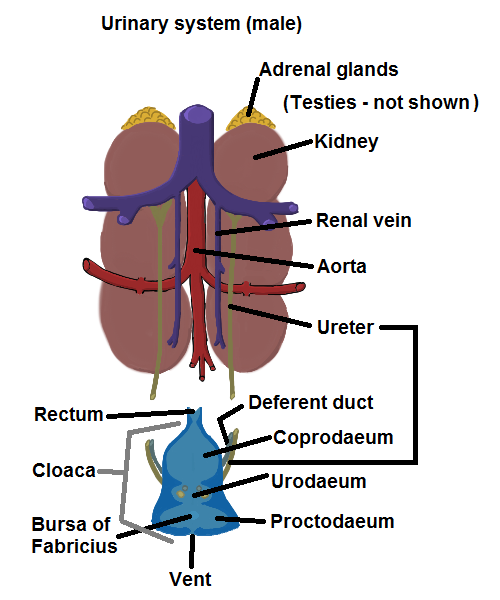
Avian urinary system
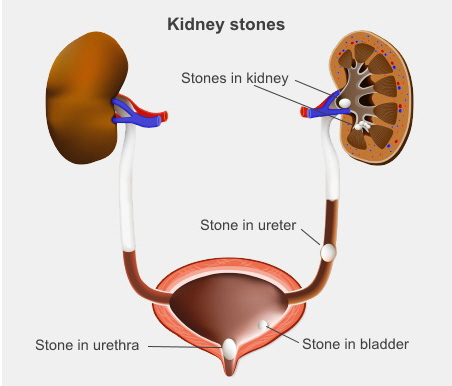
Disruption of urinary function can result in a range of conditions:
The urinary system is essential for maintaining internal balance by regulating fluid, electrolytes, and waste excretion. Its function is closely integrated with other physiological systems, making it central to overall health. For veterinary professionals, a thorough understanding of urinary physiology provides the foundation for diagnosing and managing a wide range of clinical conditions, from dehydration to renal failure.
The endocrine system is a network of glands and tissues that produce and secrete hormones, which regulate a wide range of physiological processes including growth, metabolism, reproduction, and stress responses. Unlike the nervous system, which provides rapid and short-lived control, the endocrine system exerts slower but longer-lasting effects on target organs. In veterinary medicine, understanding endocrine physiology is essential for diagnosing and managing hormonal disorders, interpreting metabolic diseases, and appreciating how different systems in the body are integrated. Many clinical conditions—such as diabetes mellitus, hypothyroidism, and Cushing’s disease—arise from endocrine dysfunction, highlighting the importance of this system.
Hormones are chemical messengers secreted into the bloodstream and carried to distant target cells. Their effects depend on the presence of specific receptors.
A central concept in endocrine physiology is Hormonal regulation, where hormone secretion is tightly controlled to maintain internal balance.
Hormones can be classified based on their chemical structure:
The type of hormone determines how it is transported, how it interacts with cells, and how long it remains active.

Peptide hormones
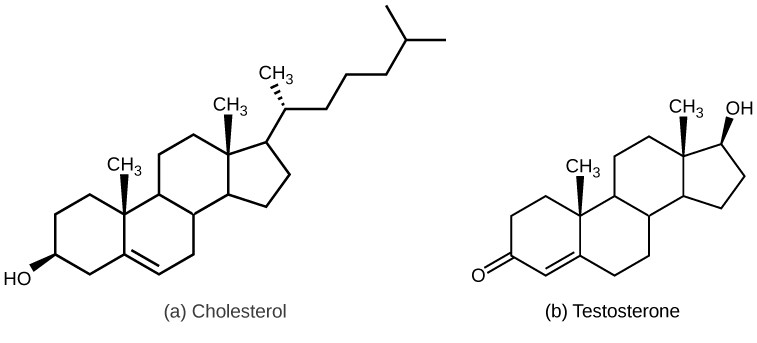
Steroid hormones
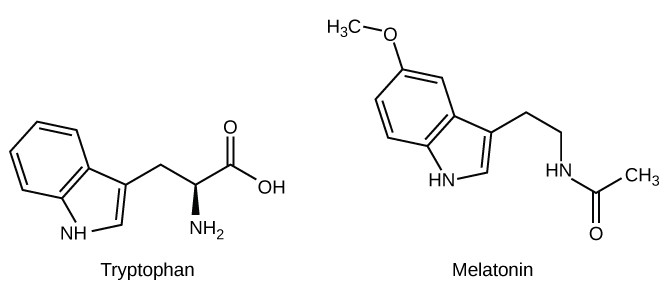
Amine hormones
Hormones exert their effects through receptor binding.

Mechanism of hormone action
Hormone release is regulated by feedback mechanisms, primarily Negative feedback.
Example: Thyroid hormones inhibit further release of TSH
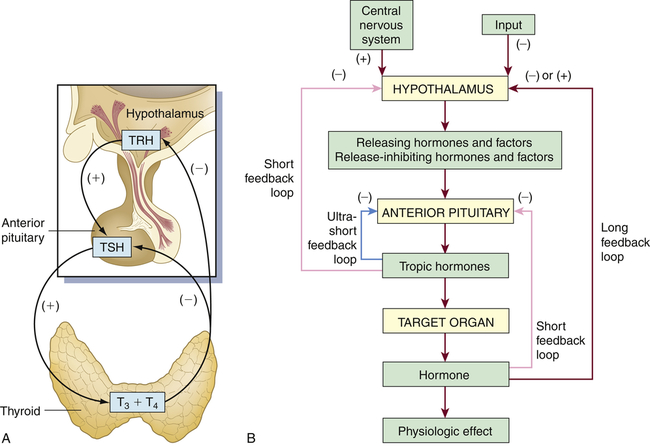
Hormone feedback loops
Acts as the link between the nervous and endocrine systems.
Known as the "master gland" because it regulates other endocrine glands.
Anterior pituitary:
Posterior pituitary:
Produces:
Functions:
Secrete parathyroid hormone (PTH), which regulates calcium and phosphorus balance.
Located near the kidneys and composed of:
Cortex:
Medulla:
Contains islets of Langerhans:
These hormones regulate reproduction and secondary sexual characteristics.
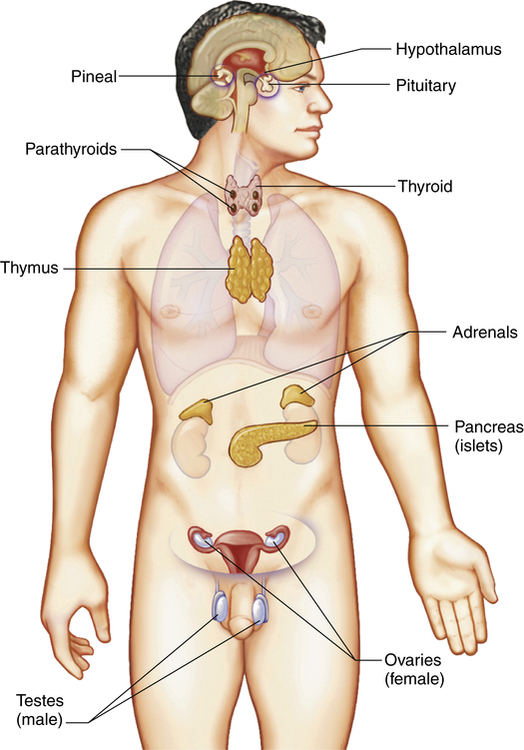
Endocrine glands
The endocrine system interacts closely with:
The endocrine system maintains internal balance by regulating:
Hormonal regulation ensures that physiological processes remain within normal limits despite changing conditions.
Endocrine disorders arise from:
These differences are important for diagnosis and treatment.
The endocrine system is a vital regulatory network that coordinates long-term physiological processes through hormone signaling. Its influence extends across all body systems, ensuring proper growth, metabolism, and adaptation to environmental changes. For veterinary professionals, a strong understanding of endocrine physiology is essential for recognizing disease, interpreting clinical signs, and providing effective treatment. It serves as a critical bridge between basic physiology and clinical medicine.
The nervous system is a highly specialized and complex system responsible for the rapid coordination and regulation of body functions. It enables animals to perceive their environment, process information, and respond appropriately through motor and behavioral outputs. In contrast to the endocrine system, which acts through slower hormonal signaling, the nervous system provides fast, precise, and short-duration control. In veterinary medicine, understanding nervous system physiology is essential for diagnosing neurological disorders, interpreting clinical signs such as paralysis or seizures, and managing conditions affecting behavior, movement, and organ function. The nervous system is also central to integrating the activities of all other systems, making it fundamental to overall animal health.
The nervous system is divided into two major components:
The CNS serves as the control center, integrating sensory information and generating responses.
The PNS connects the CNS to the rest of the body and is further divided into:
These systems work in balance to maintain internal stability.
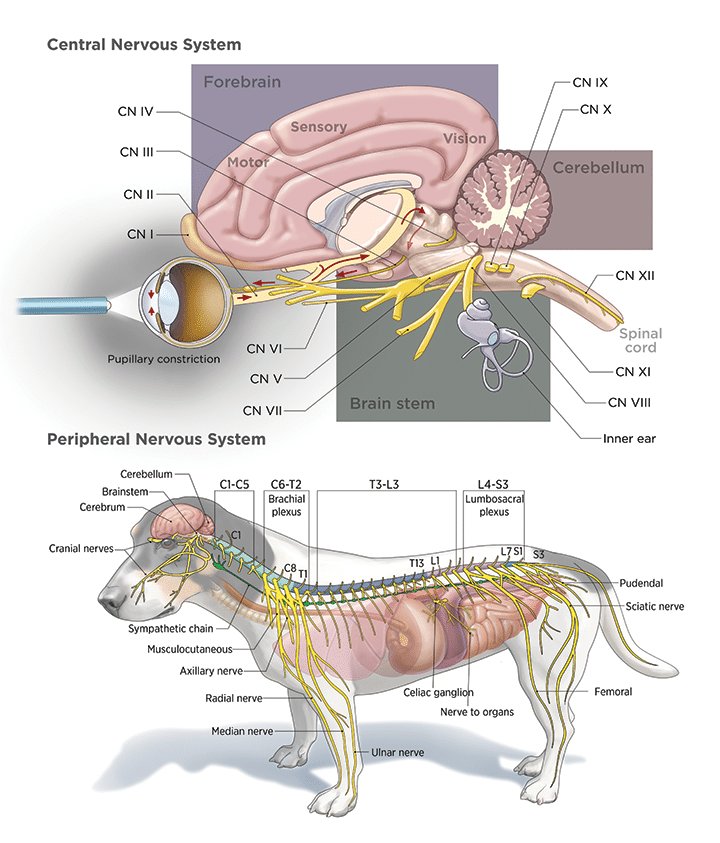
Canine Nervous System
The functional unit of the nervous system is the neuron. A neuron consists of:
Neurons communicate via electrical and chemical signals, allowing rapid transmission of information throughout the body.
Supporting cells, known as glial cells, provide structural support, insulation, and protection.
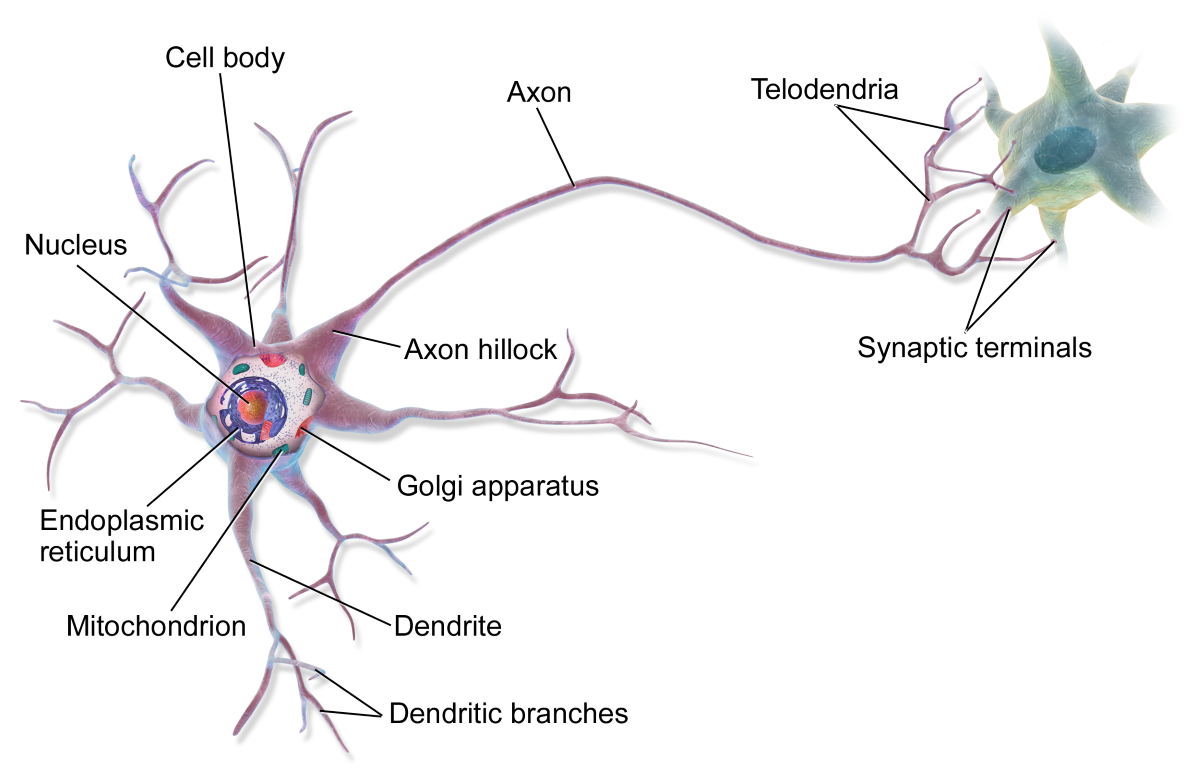
Structure of the neuron
Communication within the nervous system depends on the generation and propagation of electrical signals.
A key concept is the Action Potential, which is a rapid change in membrane potential that travels along the axon.
This process allows for rapid and directional signal transmission.
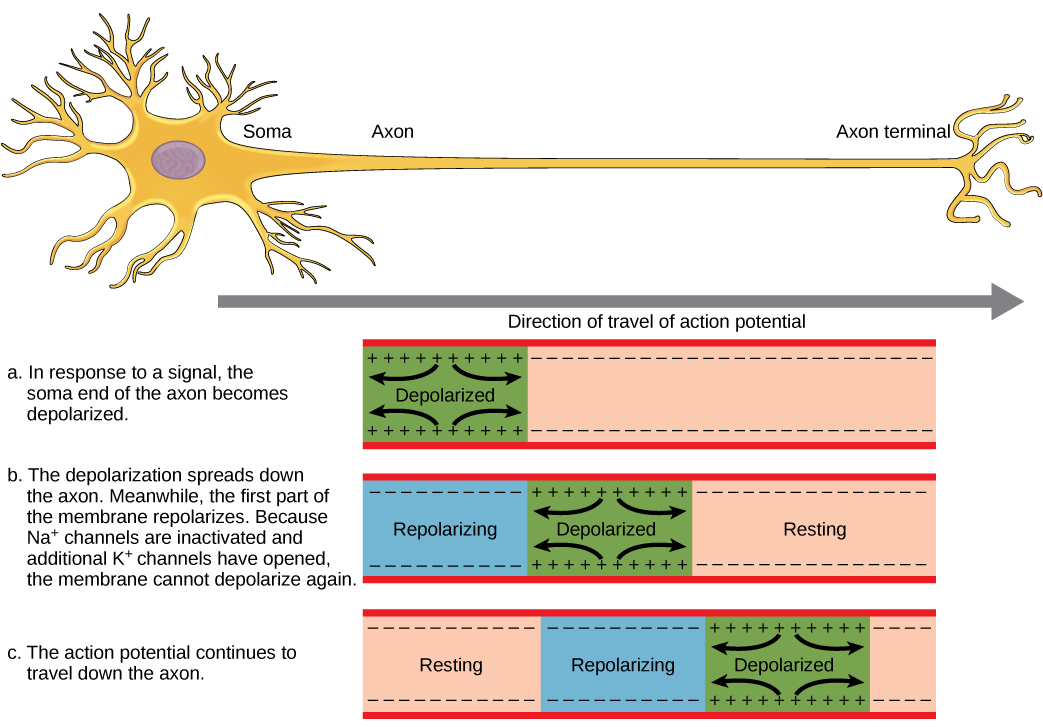
Nerve impulse conduction
Neurons communicate with other cells at specialized junctions called synapses.
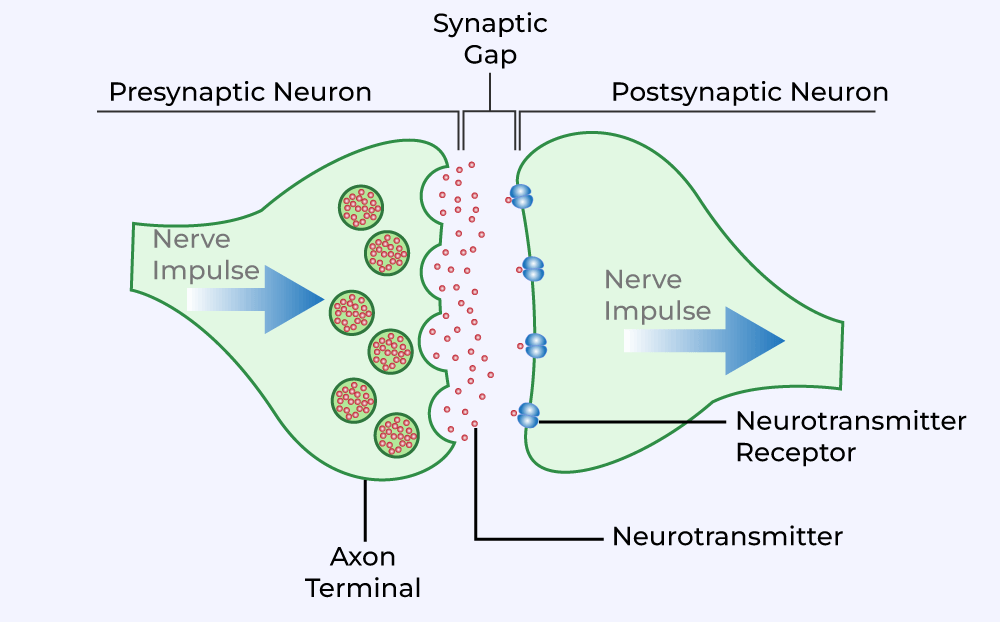
Synaptic Transmission
The type of neurotransmitter determines whether the signal is excitatory or inhibitory.
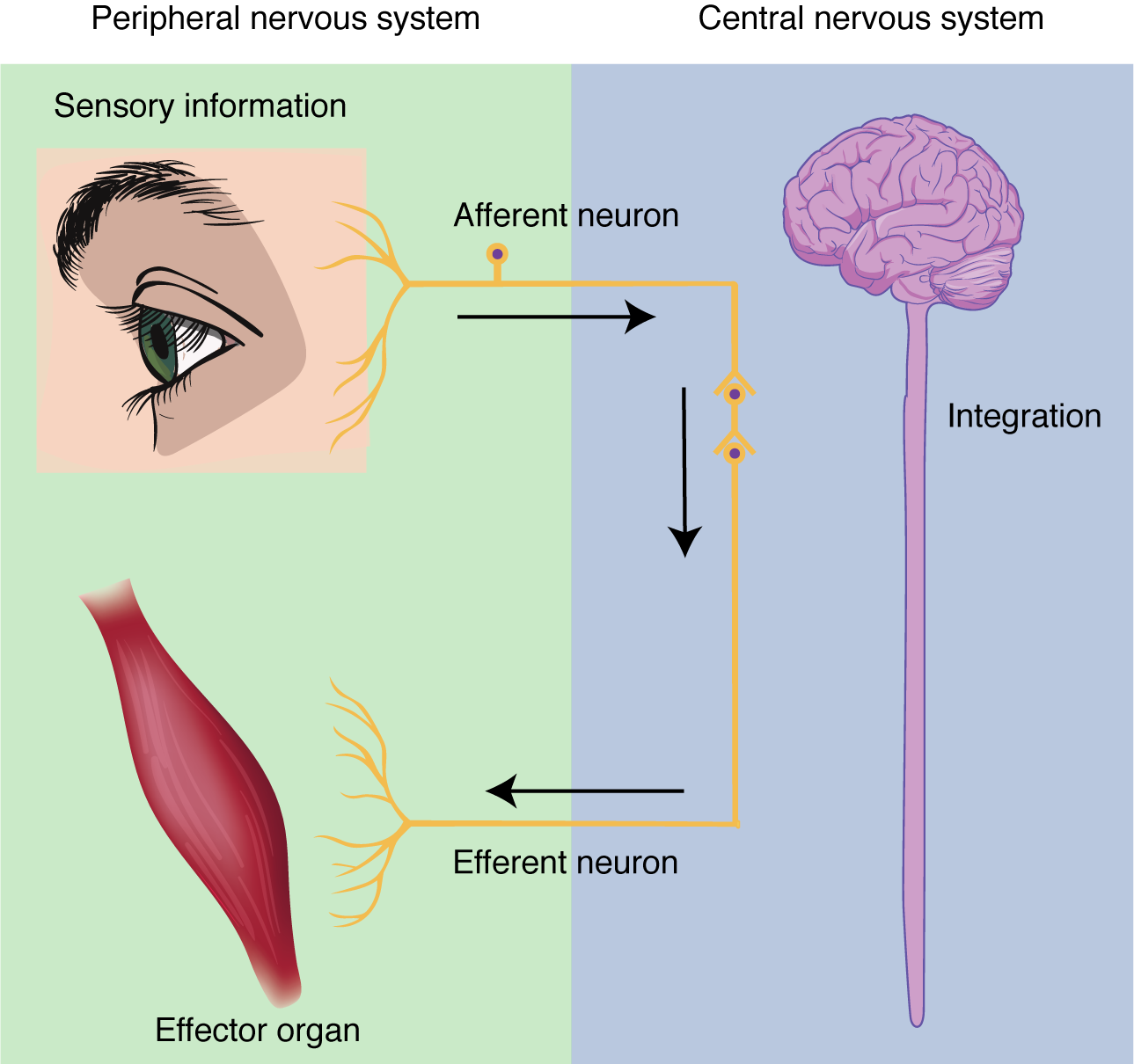
Functional division of the nervous system
A reflex is a rapid, automatic response to a stimulus.
A typical reflex arc includes:
Reflexes are important for protection and basic physiological functions.
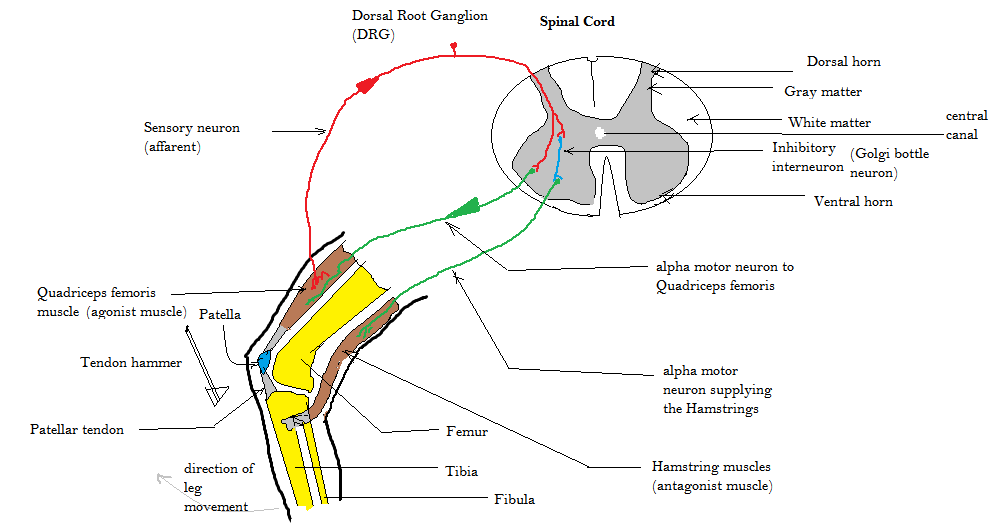
Components of the reflex arc
The brain is divided into several regions:
Each region has specialized roles, but they work together to ensure coordinated function.
The spinal cord serves as:
Damage to the spinal cord can result in loss of sensation and motor function below the site of injury.
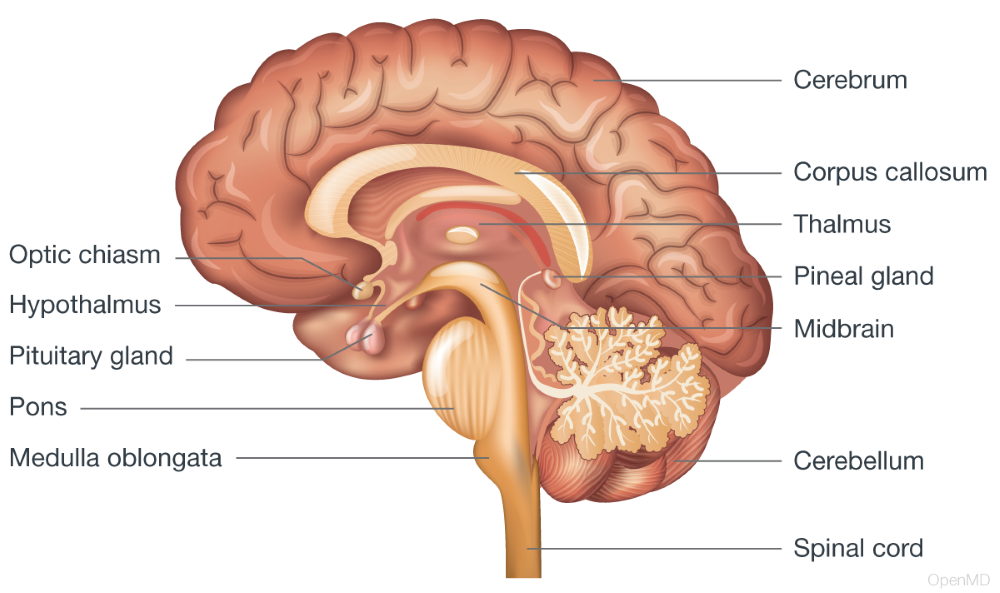
Components of the human brain
The ANS regulates involuntary processes such as:
Balance between these systems is essential for maintaining normal function.
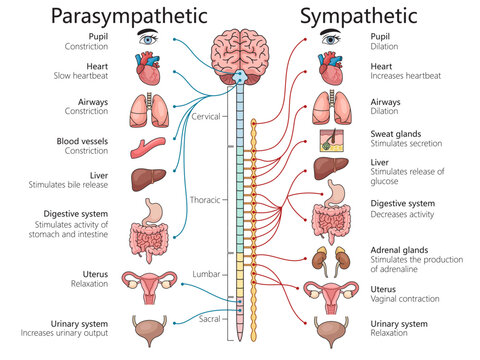
The Autonomic nervous system
The nervous system interacts with:
Animals rely on specialized receptors to detect environmental changes:
These inputs are processed by the CNS to generate appropriate responses.
The Autonomic nervous system
Neurological diseases can affect any part of the nervous system.
Common Mechanisms
The nervous system is a complex and highly coordinated system responsible for rapid communication and control within the body. Through electrical and chemical signaling, it integrates sensory input, processes information, and produces appropriate responses. For veterinary professionals, a strong understanding of nervous system physiology is essential for diagnosing and managing neurological conditions and ensuring effective clinical care. It forms a critical link between basic physiology and clinical practice.
The reproductive system is responsible for the production of offspring and the continuation of species. In veterinary medicine, it holds particular importance not only for animal health but also for livestock productivity, genetic improvement, and population management. Understanding reproductive physiology enables veterinarians to manage breeding programs, diagnose reproductive disorders, and improve fertility outcomes in both companion and production animals. Reproduction is a highly coordinated process involving the interaction of anatomical structures, hormonal regulation, and behavioral factors. It is closely integrated with the endocrine system, which governs reproductive cycles, gamete production, and pregnancy.
The reproductive system differs between males and females but serves the common purpose of producing and delivering gametes.
The testes have two primary functions:
Spermatogenesis occurs within the seminiferous tubules and involves the transformation of germ cells into mature spermatozoa.
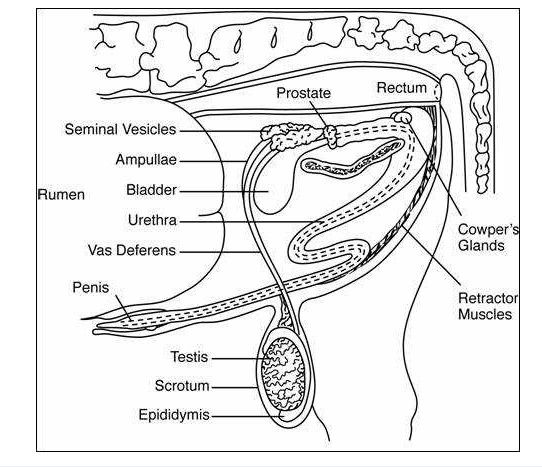
Each structure is specialized to support fertilization and, in females, the development of the fetus.
The ovaries perform two main roles:
Functions of the Uterus include:
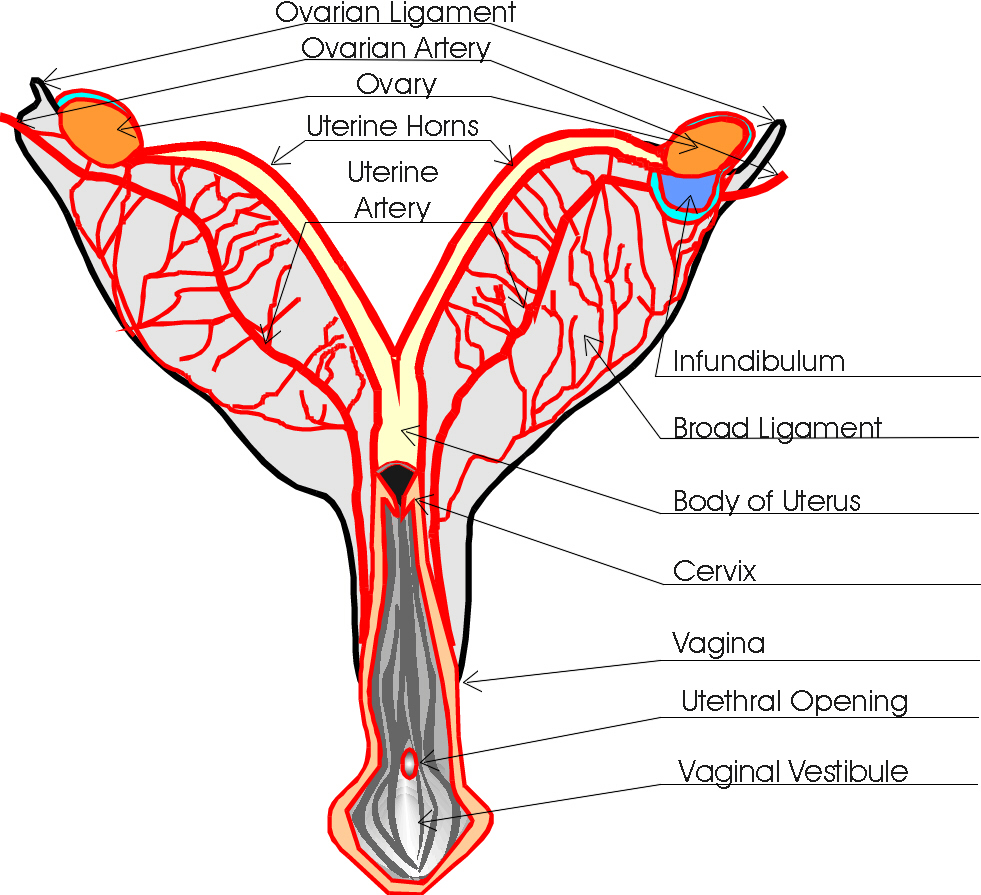
The process is regulated by the hypothalamic–pituitary–gonadal axis:
Testosterone is essential for:
After production, sperm move to the epididymis where they mature and gain motility. During ejaculation, sperm are transported through the vas deferens and mixed with secretions from accessory glands to form semen.
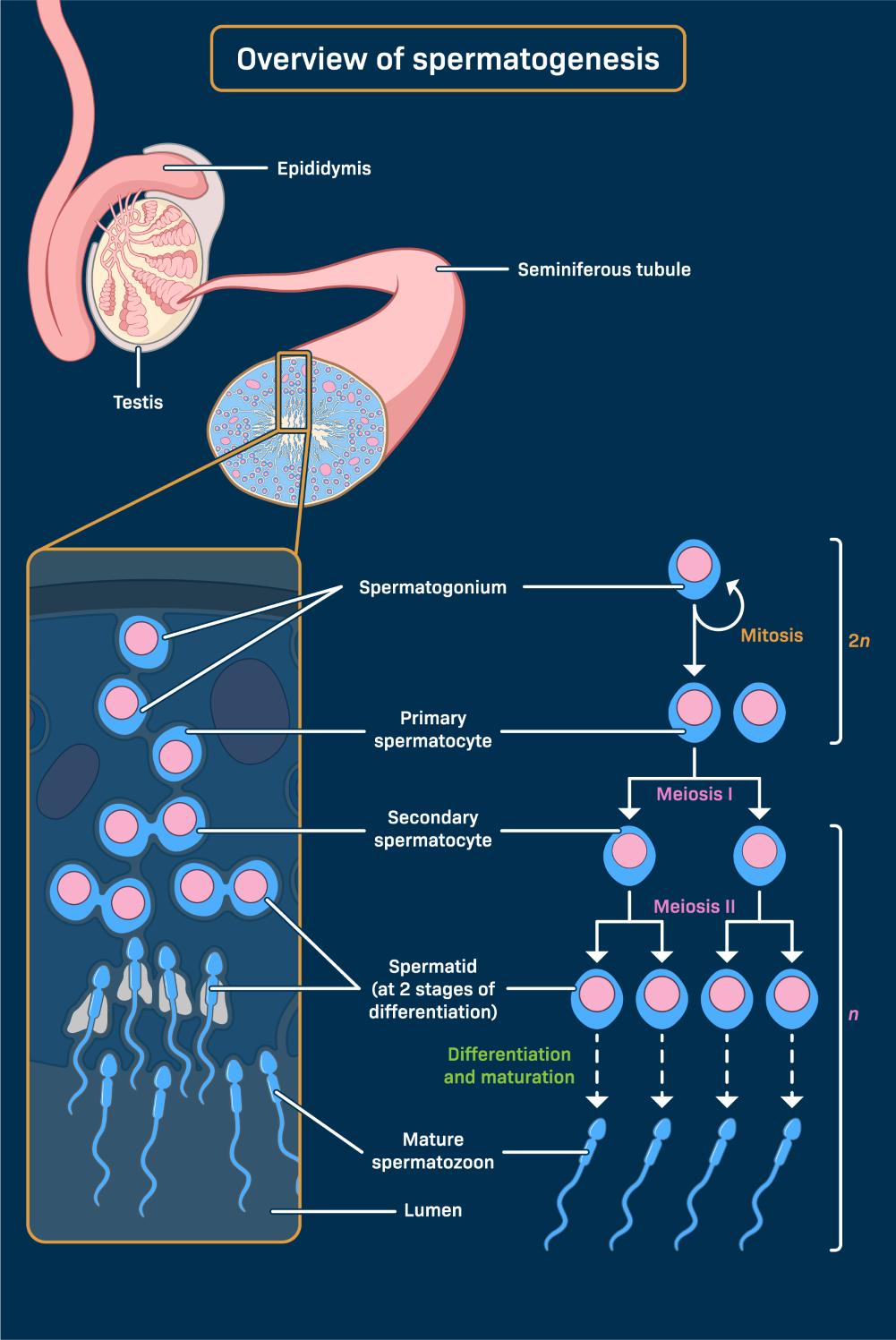
Unlike humans, most domestic animals exhibit an estrous cycle, which is a recurring reproductive cycle. For instance, the bovine estrous cycle lasts an average of 21 days and is divided into four distinct stages that facilitate the preparation of the reproductive tract for potential pregnancy.
Stages of the Bovine Estrous Cycle
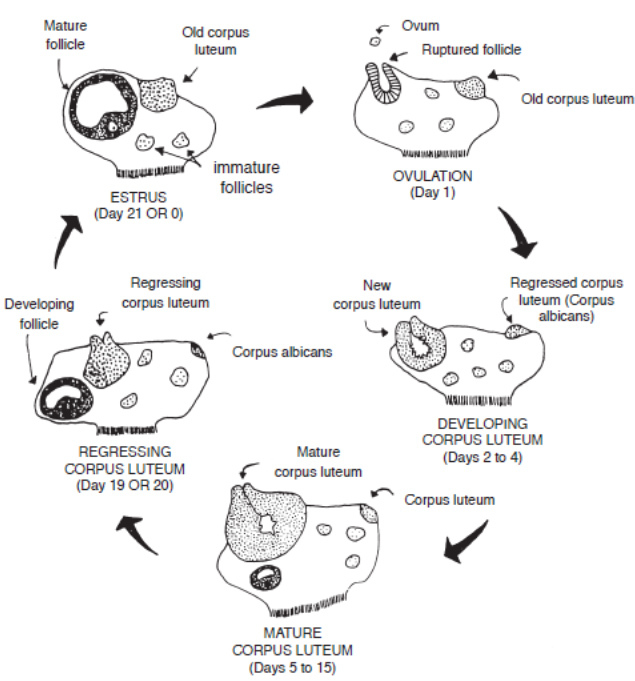
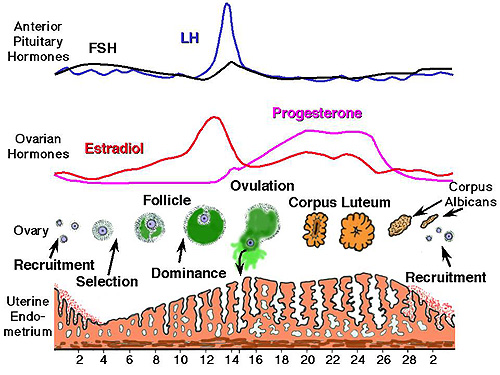
The hormonal regulation of reproduction in female animals is a sophisticated feedback system primarily governed by the hypothalamic-pituitary-gonadal (HPG) axis. It begins with the hypothalamus releasing Gonadotropin-Releasing Hormone (GnRH), which signals the anterior pituitary gland to secrete Follicle-Stimulating Hormone (FSH) and Luteinizing Hormone (LH).
Key Hormones and Their Roles
In species like cattle, this cycle operates in distinct "follicular waves," where the balance between these hormones determines whether a follicle will reach maturity or undergo regression. If fertilization does not occur, the uterus releases Prostaglandin F2α, which destroys the Corpus Luteum, causing progesterone levels to VIII and allowing a new cycle to begin.
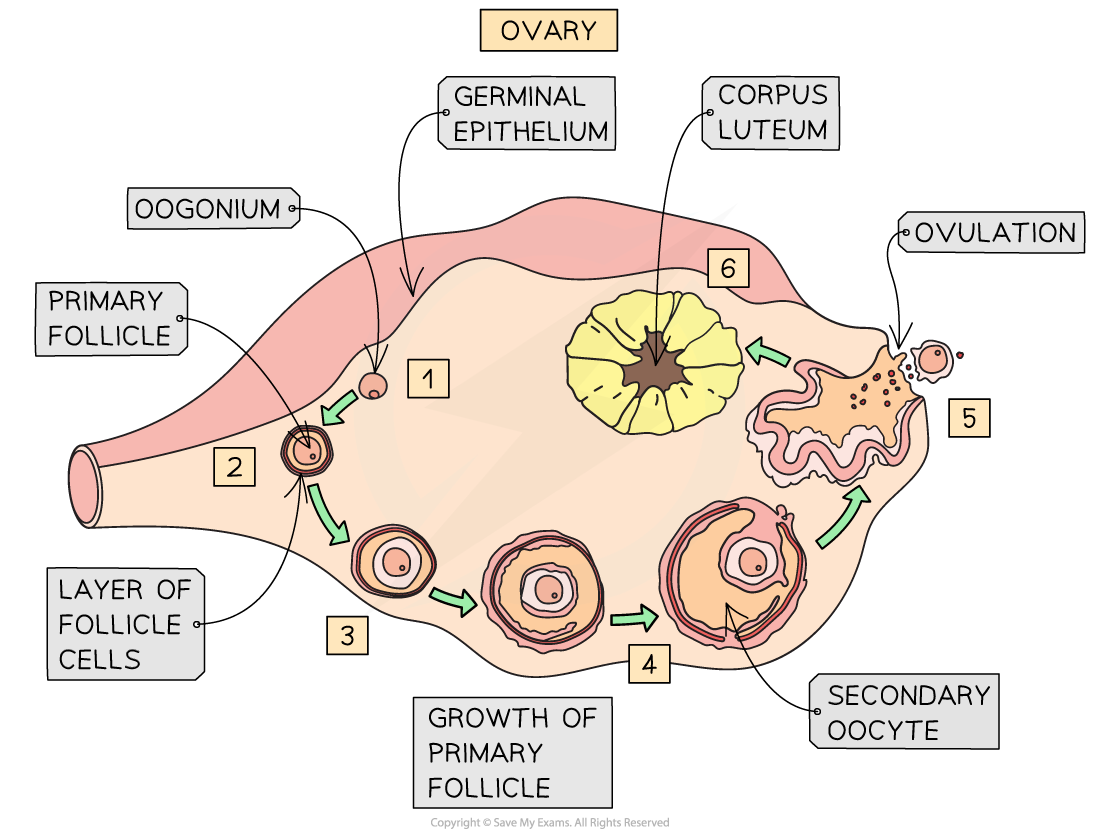
Oogenesis in animals is the complex biological process by which female gametes, or ova, are produced. In cattle, this journey begins before birth, when a female calf is born with a lifetime supply of primary oocytes housed within primordial follicles in her ovaries. These oocytes remain in a state of suspended animation until the animal reaches puberty. Once the estrous cycle begins, hormonal signals trigger groups of these follicles to grow in "waves."
Typically, in cattle, a single dominant follicle matures and undergoes the first meiotic division to become a secondary oocyte just before ovulation. Unlike sperm production, which is continuous, oogenesis is a cyclical and highly regulated event; if the egg is not fertilized after being released into the oviduct, the cycle resets, and the process begins anew with a different set of follicles.
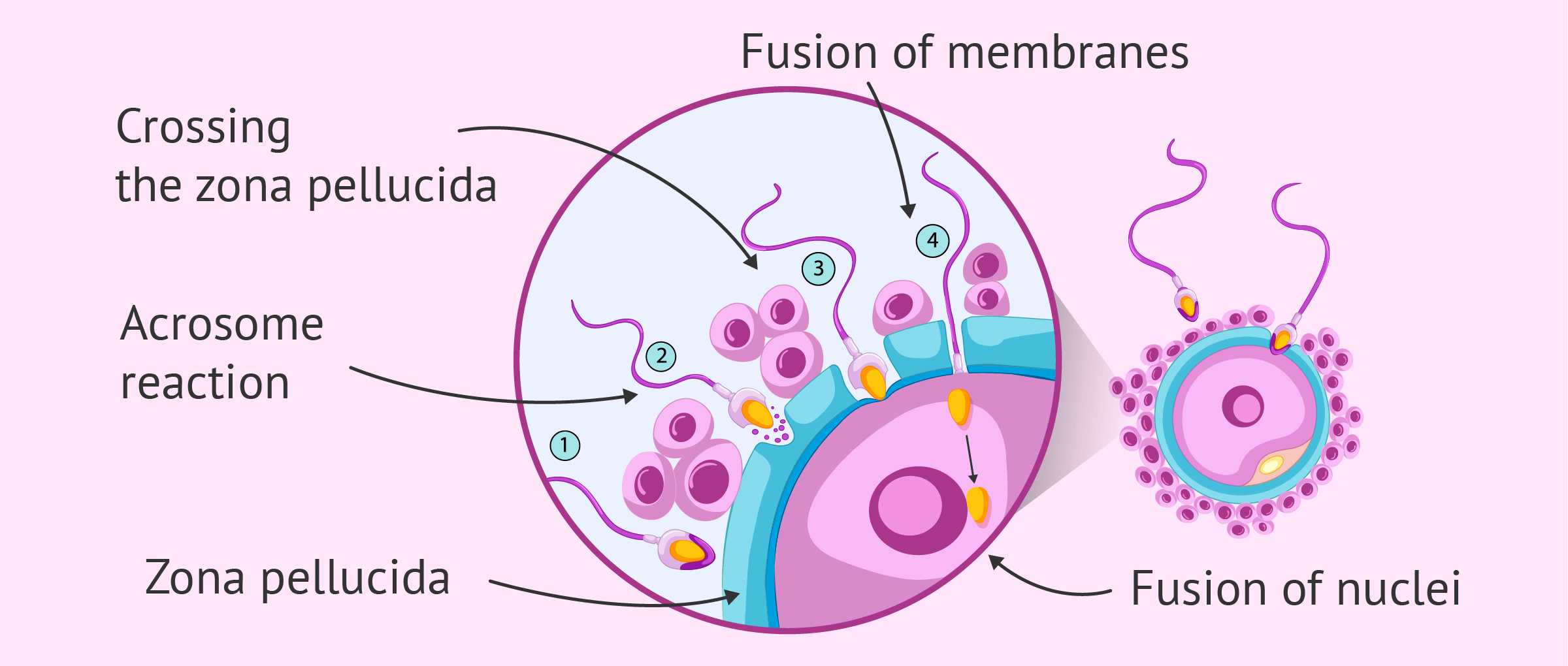
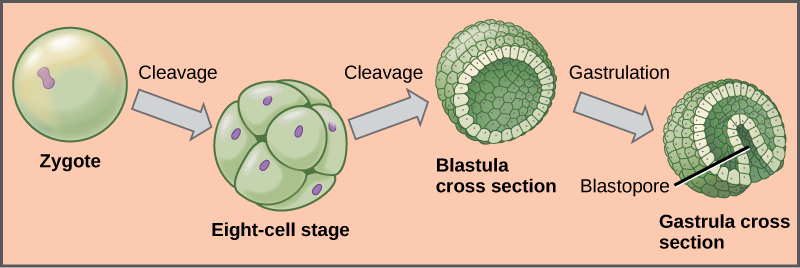
Fertilization is the critical union of the haploid sperm and oocyte within the oviduct, typically occurring in the ampulla. In cattle, once the sperm penetrates the zona pellucida and fuses with the oocyte plasma membrane, a cortical reaction occurs to prevent polyspermy. This fusion triggers the completion of the second meiotic division, forming a zygote.
Early development involves a series of rapid mitotic divisions known as cleavage, where the zygote transforms into a morula and subsequently a blastocyst. A pivotal moment in bovine reproduction is maternal recognition of pregnancy; around day 16, the embryo secretes Interferon-tau, which prevents the release of Prostaglandin F2$\alpha$, thereby maintaining the Corpus Luteum and progesterone production. The blastocyst eventually "hatches" from the zona pellucida to begin implantation in the uterine wall, marking the transition from the embryonic stage to the fetal stage.
Pregnancy and gestation represent the period from conception to parturition, varying significantly across species—ranging from approximately 63 days in dogs and cats to roughly 283 days in cattle. Once the embryo achieves maternal recognition of pregnancy, it undergoes implantation, where the fetal membranes attach to the endometrium to form the placenta. This organ is vital for the selective exchange of nutrients, gasses, and waste between the maternal and fetal circulations.
Clinical Veterinary Considerations
Parturition, or the process of giving birth, is a critical physiological event in veterinary medicine that is initiated by the "fetal stress" response. As the fetus reaches the end of its gestational term and outgrows the placenta's nutrient supply, it releases fetal cortisol, which triggers a cascade of hormonal shifts: a sharp decrease in maternal progesterone (the "progesterone block" is lifted) and a corresponding rise in estrogen and oxytocin.
Clinical Stages of Parturition
In veterinary practice, particularly in livestock management, parturition is divided into three clinical stages:
Clinicians must closely monitor these stages for signs of dystocia (difficult birth), which may require manual intervention, pharmaceutical support like oxytocin, or surgical procedures such as a Cesarean section. Following birth, the immediate focus shifts to neonatal care and ensuring the dam undergoes successful uterine involution and enters lactation to provide essential colostrum.

Following parturition, the mammary glands produce milk to nourish the newborn.
Lactation is essential for neonatal survival and immune protection through colostrum.

Understanding species differences is a cornerstone of veterinary medicine, as the "one size fits all" approach does not apply to reproductive physiology. These variations are often categorized by the type of estrous cycle and the specific anatomy of the placenta. For instance, while cattle and polyestrous domestic species cycle year-round, others are seasonally polyestrous, such as horses (long-day breeders) and sheep (short-day breeders), whose reproductive activity is triggered by changes in melatonin secretion. Dogs, by contrast, are monoestrous, typically experiencing only one or two cycles per year with a prolonged period of reproductive inactivity known as anestrus.
Furthermore, the mechanism of ovulation varies; while most domestic species are spontaneous ovulators, others like cats and camelids are induced ovulators, requiring the physical act of mating to trigger the LH surge. Anatomical differences also dictate clinical procedures; for example, the "interdigitating pads" of the porcine cervix make artificial insemination techniques vastly different from the relatively straightforward cervical rings found in bovine anatomy.
In veterinary practice, reproduction is closely linked to productivity.
Key factors influencing reproductive success:
Technologies such as artificial insemination and embryo transfer are widely used to improve reproductive outcomes.
Reproductive dysfunction can occur due to hormonal, structural, or infectious causes.
The reproductive system interacts with:
The reproductive system is a complex and highly regulated system essential for species survival and animal production. It involves coordinated interactions between anatomical structures, hormonal signals, and environmental factors. For veterinary professionals, a strong understanding of reproductive physiology is crucial for improving fertility, managing breeding, and addressing reproductive disorders. It represents a key area where physiology directly translates into clinical and economic outcomes.